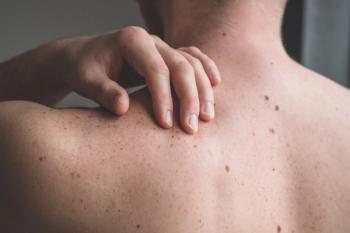
Immunotherapy Safely Treats Advanced Squamous Cell Carcinoma
An anti–PD-1 monoclonal antibody is safe and effective for patients with unresectable, locally advanced, or metastatic cutaneous squamous cell carcinoma.
A fully human anti–programmed death 1 (PD-1) monoclonal antibody is safe and effective for patients with unresectable, locally advanced, or metastatic cutaneous squamous cell carcinoma (CSCC).
There is no widely accepted standard of care for unresectable, locally advanced, or metastatic CSCC. Conventional chemotherapy can induce tumor response, but often is poorly tolerated among older patients with CSCC, said Kyriakos P. Papadopoulos, MD, of South Texas Accelerated Research Therapeutics (START) in San Antonio, at the 2017 American Society of Clinical Oncology (ASCO) Annual Meeting (abstract
Ultraviolet light–induced DNA damage causes hypermutation in most CSCCs, which have a higher mutation rate than any other tumor type in the Cancer Genome Atlas. “CSCC tumors may be responsive to PD-1 checkpoint blockade,” said Papadopoulos.
In the dose-escalation portion of the phase I study of the PD-1 blocker REGN2810, a durable, more than 19-month radiologic complete response was observed in 1 patient with metastatic CSCC.
Papadopoulos reported on two expansion cohorts of patients with distantly metastatic and locally advanced CSCC. All patients received 3-mg/kg REGN2810 by intravenous infusion over 30 minutes every 2 weeks for up to 48 weeks.
Research biopsies were performed at baseline and day 29 (and at progression, if possible). Tumor measurements were performed every 8 weeks to determine overall response rate (ORR).
The study enrolled 26 patients (10 with metastatic disease and 16 with locally advanced disease), with a median age of 72.5 years. The patients took a median 11 doses of REGN2810.
After a median of 7 months follow-up, the ORR was 46.2% (12 of 26 patients), and the disease control rate was 69.2% (18 of 26 patients). Median progression-free survival and overall survival have not been reached.
Among the 11 patients with confirmed responses, 1 patient had progressive disease at 21 weeks and 10 patients remain in response from more than 8 weeks to more than 40 weeks.
“REGN2810 produced rapid, deep, and durable tumor reductions in target lesions in both cohorts,” noted Papadopoulos.
The drug was also active across all programmed death ligand 1 (PD-L1) strata in CSCC, according to immunohistochemistry. Correlative studies are in progress, including PD-L1 status and whole exome tumor DNA sequencing.
The most common treatment-related adverse event of any grade was fatigue (19.2%). One grade 3 or higher event was noted for AST elevation, ALT elevation, arthralgia, and rash. Two patients discontinued treatment due to treatment-related adverse events. Two patients died within 30 days of the last dose, but this was considered unrelated to the drug.
“This is the first prospective study of a PD-1 inhibitor in patients with advanced CSCC. REGN2810 was generally well tolerated in this predominantly older population,” concluded Papadopoulos.
Both locally advanced and metastatic CSCC are highly responsive to the drug, “and durability is emerging,” he said. “A unifying characteristic of cutaneous malignancies appears to be responsiveness to immune checkpoint inhibition.”
An ongoing phase II pivotal trial of REGN2810 in patients with unresectable and locally advanced CSCC is underway.
Newsletter
Stay up to date on recent advances in the multidisciplinary approach to cancer.