A 58-Year-Old Woman on Gemcitabine Developed Swelling and Erythema of Both Legs
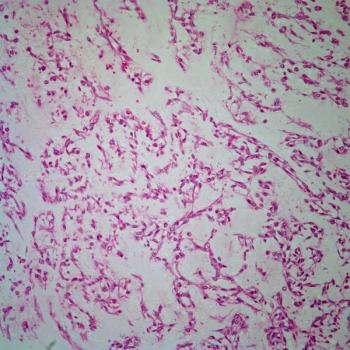
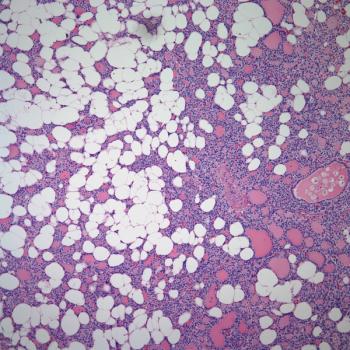
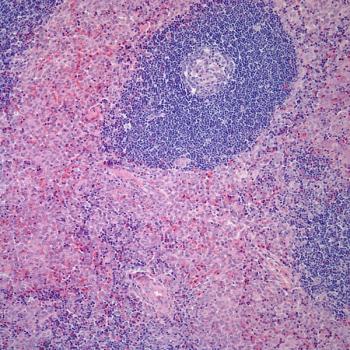
A 58-year-old woman was diagnosed with ovarian carcinoma and initially treated by surgery and adjunctive chemotherapy. Following a remission of 3 years, she developed biopsy-confirmed recurrent/metastatic disease involving bones, inguinal lymph nodes, and soft tissue of the back. Following a failure of response to platinum-based treatment, she was given gemcitabine (Gemzar) in a dose of 1000 mg/m2. Two days after her first infusion she developed tender swelling and mild to moderate erythema of both legs, particularly striking in the posterior aspect (see photo). The patient was afebrile.
Complete blood count was normal, and Doppler angiography failed to disclose vascular occlusion. Despite negative blood and skin aspirate cultures, intravenous vancomycin and cefazolin therapy were administered for presumed cellulitis. The eruption faded without residual abnormality in about 1 week. Two days following her next per-protocol gemcitabine infusion, the same type of eruption appeared in almost the exact same anatomical areas.
Which statement is true regarding this phenomenon?