
Carey K. Anders, MD, concludes with a look toward the future of HER2+ breast cancer treatment and provides advice to community oncologists treating patients with breast cancer.

Your AI-Trained Oncology Knowledge Connection!


Carey K. Anders, MD, concludes with a look toward the future of HER2+ breast cancer treatment and provides advice to community oncologists treating patients with breast cancer.

An overview of the design and rationale for the phase 2 BRIDGET study looking at the addition of tucatinib to HER2-directed antibody therapy in breast cancer.

An expert on metastatic breast cancer provides clinical insights gleaned from the HER2CLIMB-02 trial and discusses the design and rationale of the ongoing HER2CLIMB-05 study.

Following SABCS 2023, Carey K. Anders, MD, reviews recent updates from the KATHERINE and APHINITY clinical trials in HER2+ breast cancer.

The panelists conclude their discussion on HER2-positive breast cancer by underscoring the importance of preventive measures for brain metastases, enhanced strategies for managing leptomeningeal disease, and improved approaches to handle treatment-related toxicity.

Heather Moore, CPP, PharmD, shares expert insights on managing T-DXd-related adverse effects, including prophylactic measures for nausea and strategies for monitoring and management of ILD.

Rani Bansal, MD explores recent findings suggesting a risk of radiation necrosis in patients undergoing treatment with ADCs and concurrent radiotherapy for brain metastases and discusses the potential implications for future treatment approaches.

Rani Bansal, MD, discusses progressive developments in treating brain metastases in HER2-positive breast cancer, highlighting insights from the TUXEDO and DEBORAH trials, and examines the potential role of T-DXd in managing leptomeningeal disease.

Rani Bansal, MD, discusses the case of a 54-year-old post-menopausal patient who develops liver and brain metastases after undergoing prior therapy with trastuzumab/pertuzumab and T-DM1.

Heather Moore, CPP, PharmD examines the role of topical diclofenac gel in the management of hand and foot syndrome associated with capecitabine, highlighting key insights from the D-TORCH trial.

Heather Moore, CPP, PharmD, shares expert insights on the effective management of adverse effects related to tucatinib and other HER2 tyrosine kinase inhibitors (TKIs).

Carey Anders, MD, offers insights into the BRIDGET trial, a study investigating the role of tucatinib in the prevention of secondary brain metastases in patients with advanced HER2-positive breast cancer.

Carey Anders, MD, examines strategies for treating stable and active brain metastases in individuals with advanced HER2-positive breast cancer, highlighting key data from the HER2CLIMB trial.

Carey Anders, MD, discusses the scenario of a 34-year-old patient diagnosed with HER2-positive breast cancer, who develops brain metastases after undergoing initial therapy with dual HER2 blockade.

Heather Moore, CPP, PharmD, presents a comprehensive summary of targeted therapies for HER2-positive breast cancer and provides expert insights into the management of adverse effects associated with these treatments.

Susan Dent, MD, delves into treatment approaches for triple-positive breast cancer in the second-line and beyond, highlighting findings from the DESTINY-Breast03 trial.

Carey Anders, MD, and Susan Dent, MD, discuss the role of radiotherapy in patients with HER2-positive breast cancer and brain metastases.

Susan Dent, MD, delves into the exploration of front-line treatment options for triple-positive breast cancer and examines strategies for restaging in the event of disease progression after first-line therapy.

In this Cancer Network Around the Practice program, Susan Dent, MD discusses the case of a 66-year-old patient with grade 3 triple-positive breast cancer who presents with multiple liver and bone metastases after front-line treatment with trastuzumab and letrozole.
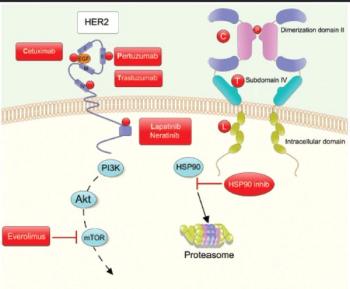
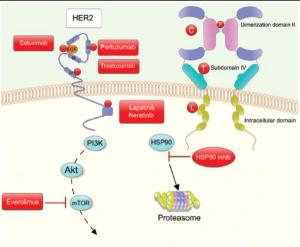
This article discusses the advances in HER2-targeted therapy, in both the metastatic and adjuvant settings, with a focus on those with early-stage breast cancer.
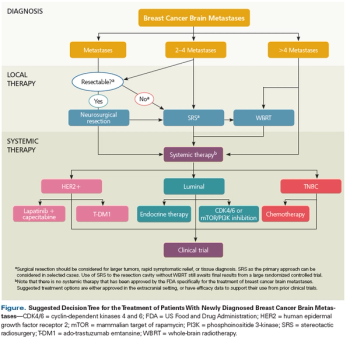
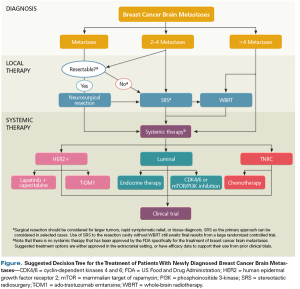
This review summarizes the most up-to-date approach to the multidisciplinary management of patients with breast cancer brain metastases.

Brain metastases arising from breast cancer constitute a clinically unmet need and a situation that portends a poor prognosis with few therapeutic options.

With regard to potential research strategies relevant to the treatment of triple-negative breast cancer/basal-like breast cancer, potential targets include PTEN, INPP4B, PIK3CA, KRAS, BRAF, EGFR, FGFR1, FGFR2, IGFR1, KIT, MET, PDGFRA, and the HIF1-α/ARNT pathway. Many of these will be discussed further in this review article.

In 2008, it is estimated that over 1 million women worldwide will be diagnosed with breast cancer, of which 172,695 will be classified as “triple-negative.”[1] The triple-negative phenotype encompasses a breast tumor subtype that is clinically negative for expression of the estrogen and progesterone receptors (ER and PR) and lacks overexpression of the HER2 protein, with unique prognostic and therapeutic implications.

As half of all breast cancers occur in patients beyond the age of 65 and a quarter beyond the age of 75, a significant number of patients with metastatic breast cancer are elderly. New hormonal therapies, such as aromatase inhibitors, appear to have favorably improved the survival of these patients. Side effects such as osteoporosis or cognitive issues appear manageable. Information specific to elderly patients has recently emerged in the field of chemotherapy for metastatic breast cancer. This article reviews data on anthracyclines, taxanes, capecitabine (Xeloda), gemcitabine (Gemzar), trastuzumab (Herceptin), and bevacizumab (Avastin). For most patients in this setting, sequential single-agent chemotherapy appears at this time to be the preferred course of treatment.

Published: October 1st 2006 | Updated:

Published: September 15th 2013 | Updated:

Published: July 15th 2014 | Updated:

Published: October 1st 2008 | Updated:
Published: October 15th 2016 | Updated:
Published: October 17th 2018 | Updated: