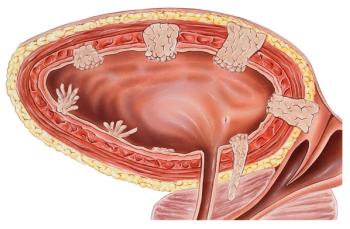
ODAC Votes in Favor of Pembrolizumab for Treatment of Certain Patients with NMIBC
The anti-PD-1 therapy was recommended as a treatment for certain patients with high-risk, non-muscle invasive bladder cancer.
The Oncologic Drugs Advisory Committee (ODAC) voted 9 to 4 in favor of recommending the FDA’s approval of pembrolizumab (KEYTRUDA), an anti-PD-1 therapy, for the treatment of certain patients with high-risk, non-muscle invasive bladder cancer (NMIBC), according to Merck, the agent’s developer.1
The recommendation was based on the
The FDA set a Prescription Drug User Fee Act (PDUFA) for January 2020.
“The positive vote from today’s ODAC meeting supports the potential for Keytruda in certain patients with high-risk, non-muscle invasive bladder cancer, who currently have limited non-surgical treatment options approved by the FDA,” Roy Baynes, MD, PhD, senior vice president and head of global clinical development, chief medical officer, Merck Research Laboratories, said in a press release. “We are encouraged by today’s productive discussion and look forward to working with the FDA as they continue their review of our supplemental application for KEYTRUDA in this patient population.”
Data from the phase II KEYNOTE-057 trial were first presented at the European Society for Medical Oncology (ESMO) 2018 Congress. In the trial, pembrolizumab had encouraging activity in patients with high-risk BCG-unresponsive CIS with or without papillary tumors and a safety profile consistent with those previously seen.2-3
Participants were given 200 mg of pembrolizumab every 3 weeks for 24 months or until recurrence, progression, or unacceptable toxicity. Patients with high-risk NMIBC or progressive disease during treatment were required to discontinue. Assessment of tumor status was performed every 12 weeks.
The major efficacy outcome measures were complete response (CR) as defined by negative results for cystoscopy with transurethral resection of bladder tumor/biopsies as applicable, urine cytology, and computed tomography urography imaging, and duration of response.
The 3-month CR rate was 38.8% (95% CI; 29.4-28.9) by central assessment. Among 40 patients who experienced a CR at 3 months, 72.5% maintained CR at last follow-up (median, 14.0 months; range 4.0-26.3) and median CR duration had not been reached (range, 0-14.1 months). Overall, 80.2% of patients had a CR duration of ≥6 months.
Treatment-related adverse events (AEs) occurred in 63.1% of participants, with the most frequent being pruritus (10.7%), fatigue (9.7%), diarrhea (8.7%), hypothyroidism (5.8%), and maculopapular rash (5.8%). Grade 3/4 AEs occurred in 12.6% of patients, and 1 death was considered treatment related. Immune-mediated AEs occurred in 18.4%.
References:
1. FDA Oncologic Drugs Advisory Committee (ODAC) Recommends KEYTRUDA® (pembrolizumab) for the Treatment of Certain Patients with High-Risk, Non-Muscle Invasive Bladder Cancer (NMIBC) [news release]. Kenilworth, New Jersey. Published December 17, 2019. mrknewsroom.com/news-release/oncology/fda-oncologic-drugs-advisory-committee-odac-recommends-keytruda-pembrolizumab-. Accessed December 18, 2019.
2. FDA Grants Priority Review to Merck’s Supplemental Biologics License Application (sBLA) for KEYTRUDA® (pembrolizumab) in Certain Patients with High-Risk, Non-Muscle Invasive Bladder Cancer (NMIBC) [news release]. Kenilworth, NJ. Published December 2, 2019. mrknewsroom.com/news-release/oncology/fda-grants-priority-review-mercks-supplemental-biologics-license-application-s. Accessed December 2, 2019.
3. Balar AV, Kulkarni GS, Uchio EM, et al. Keynote 057: Phase II trial of Pembrolizumab (pembro) for patients (pts) with high-risk (HR) nonmuscle invasive bladder cancer (NMIBC) unresponsive to bacillus calmette-guérin (BCG). Journal of Clinical Oncology. doi:10.1200/JCO.2019.27.7_suppl.350