Jason M. Hafron, MD, CMO, and Oliver Sartor, MD, share their approach for the optimal management of mCRPC through genetic testing.

Jason M. Hafron, MD, CMO, and Oliver Sartor, MD, share their approach for the optimal management of mCRPC through genetic testing.
Daniel P. Petrylak, MD, leads the discussion on sequencing treatment for a patient with mCRPC, such as in case 2, who progresses on docetaxel therapy.
Prostate cancer experts review the use of PSMA PET/CT imaging and Axumin imaging for patients with metastatic castration-resistant prostate cancer.
Raoul S. Concepcion, MD, presents the case of a 64-year-old-man with mCRPC, and Jason M. Hafron, MD, CMO, leads the discussion on the optimal treatment approach for the given case.

Daniel P. Petrylak, MD, leads the discussion on approaching treatment of high-volume metastatic castration-naïve prostate cancer.

A panel of experts in prostate cancer examine the use of conventional imaging and PSMA PET/CT and the impact on their approach to the management of mCNPC.
Dr Raoul S. Concepcion presents the case of a 69-year-old man with metastatic castration-naïve prostate cancer (mCNPC), and the panel shares their personal approaches to treatment.

Raoul S. Concepcion, MD, FACS, poses polling questions for the audience’s medical specialty and the percent of patients they receive with prostate cancer.
A 24-year-old otherwise healthy man with a history of retractile right testicle managed with right orchidopexy at age 9 presented with a several weeks’ history of discomfort in the left testicle. He has no family history of testicular cancer.

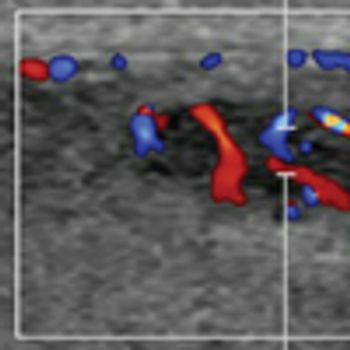
Prostate cancer management issurrounded by controversy.From the screening debatethrough choosing the best treatmentoption for localized disease, there islittle consensus on the approach to themost common solid tumor in men. Avariety of predictive models are beingdeveloped to assist in clinical decisionmaking.[1,2] Although transrectal ultrasound(TRUS)-directed prostatebiopsies represent the “gold standard”in the diagnosis of the disease, limitationsof this approach have been recognized.[3] To compensate for theselimitations, the absolute number of needlecores taken has increased from 6 to10–12 or more. TRUS enhancementssuch as color Doppler and the use ofcontrast agents hold promise, but theyhave not yet replaced the TRUS grayscaleapproach.[4]

Various treatment options are available for adenocarcinoma of the prostate-the most common malignant neoplasm among men in the United States. To select an optimum management strategy, we must be able to identify an organ-confined disease (in which local therapy such as surgery or radiation may be beneficial) vs prostate cancer beyond the confines of the gland (for which other treatment approaches may be more appropriate). At present, no standard imaging modality can by itself reliably diagnose and/or stage adenocarcinoma of the prostate. Standard transrectal ultrasound, magnetic resonance imaging (MRI), computed tomography, bone scans, and plain x-ray are not sufficiently reliable when used alone. Fortunately, advances in imaging technology have led to the development of several promising modalities. These modalities include color and power Doppler ultrasonography, ultrasound contrast agents, intermittent and harmonic ultrasound imaging, MR contrast imaging, MRI with fat suppression, MRI spectroscopy, three-dimensional MRI spectroscopy, elastography, and radioimmunoscintigraphy. These newer imaging techniques appear to improve the yield of prostate cancer detection and staging, but are limited in availability and thus require further validation. This article reviews the status of current imaging modalities for prostate cancer and identifies emerging imaging technologies that may improve the diagnosis and staging of this disease. [ONCOLOGY 15(3):325-342, 2001]

Dr. de la Taille and colleagues from Columbia University provide an overview of the concept of molecular staging” of prostate cancer using reverse transcriptase–polymerase chain reaction (RT-PCR). They do an admirable job of summarizing all of the currently available data on the results of this assay in the clinical staging of prostate cancer. As they note, only their group and one other have been able to demonstrate that a positive assay correlates with final pathologic stage. A limited number of other studies have suggested that the RT-PCR assay can predict prostate-specific antigen (PSA) recurrence.
December 9th 2021
December 9th 2021
December 2nd 2021

November 24th 2021

February 1st 1999