Oncology NEWS International
- Oncology NEWS International Vol 11 No 9
- Volume 11
- Issue 9
Database of Congenital Nevi Shows Malignant Potential
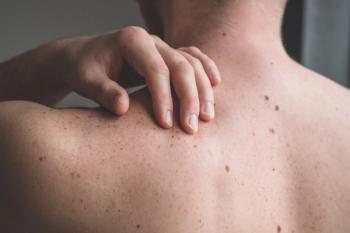
NEW ORLEANS-Because of their malignant potential and their cosmetic appearance, congenital nevi elicit much concern from parents. Ashfaq A. Marghoob, MD, assistant professor of dermatology and director of the Pigmented Lesion Group, Memorial Sloan-Kettering Cancer Center, presented new insights into this disorder at a symposium on melanoma held during the American Academy of Dermatology annual meeting.
NEW ORLEANSBecause of their malignant potential and their cosmetic appearance, congenital nevi elicit much concern from parents. Ashfaq A. Marghoob, MD, assistant professor of dermatology and director of the Pigmented Lesion Group, Memorial Sloan-Kettering Cancer Center, presented new insights into this disorder at a symposium on melanoma held during the American Academy of Dermatology annual meeting.
First 3 Years of Life
While moles that are present from birth are obviously "congenital nevi," Dr. Marghoob extends this definition also to lesions that develop within the first 3 years of life, appear clinically to be congenital, and have a history and histology that are consistent with this assessment.
One of Dr. Marghoob’s patients, for example, had only satellite nevi present at birth, but at 18 months of age developed a 20- to 30-cm mole on her back. "This was the first clinical evidence of a mole that was clinically a congenital nevus but was not evident when I first saw her," he said.
Congenital nevi begin with the melanocytic stem cell in the neural crest. These cells migrate to the leptomeninges and to the embryonic dermis, where they begin to differentiate into melanocytes. After this process, Dr. Marghoob said, the cells migrate up into the epidermis, where they begin forming pigment. The timing of this process is variable; therefore, not all congenital nevi are clinically obvious at birth.
Nevus Outreach Registry
Observations from two large data-basesthe New York University Registry and the worldwide Nevus Outreach Registry (
Dr. Marghoob based much of his presentation on the characteristics of the first 334 patients (out of a current 400) in the Nevus Outreach Registry, who are being followed prospectively to reveal information about the natural history of this condition.
Through these longitudinal observations, it has become clear that congenital nevi often change over time. Most become darker and thicker, although some occasionally become lighter and thinner, and some contain components of very fragile skin, he said.
The risk of melanoma is the real concern with congenital nevi, and this varies according to several factors. In large congenital nevi, melanomas usually develop before puberty, most often within the nevus and not the periphery, and frequently below the dermal-epidermal junction. Melanoma can also arise in small congenital nevi, but these usually occur after puberty, at the periphery of the nevus, and right at the dermal-epidermal junction, he said.
Lesions 50 cm or Greater
The lifetime risk of melanoma in congenital nevi is related to their size. Lesions over 20 cm have a 4.5% to 9% risk, while those under 20 cm have a 0% to 4.9% risk.
Lesions over 50 cm have the highest risk, though the actual risk is currently unknown. The excessive risk in this size subset is based on the finding that all but one melanoma in the Nevus Outreach Registry developed in children with nevi 50 cm or greater, he said.
But beyond size, risk has not been well correlated with various features. "Is the risk greater for the lesion that has a fairly flat, light brown, homogenous surface but covers a very large portion of the body, or the lesion that is rugose, with a mammilated and thickened surface? We don’t know the answer to this yet," Dr. Marghoob said.
What we do know, he continued, is that patients with large congenital nevi appearing in the paraspinal area (the head, neck, and posterior midline) and patients who have multiple satellite nevi are at high risk for developing melanoma. "And it is these same individuals who are at high risk for developing neurocutaneous melanosis (NCM)," he said.
Neurocutaneous Melanosis
Neurocutaneous melanosis occurs when the same nevus cells that develop in the skin also form in the central nervous system. It causes neurological problems and is potentially fatal.
The 5-year risk of melanoma for patients with NCM is similar to that of patients with congenital nevi, about 2% to 3%. In the Nevus Outreach Registry, 24 patients currently have NCM, and there has been one death from complications of this disease, not from melanoma, he reported.
"So patients with large congenital nevi on the posterior axis and patients with multiple congenital nevi are both at risk for developing neurocutaneous melanosis. The link between the conditions may be the satellite nevi," he said.
In the Nevus Outreach Registry, 60% of patients with NCM had at least 50 satellite nevi, compared with about 20% of persons without NCM. In patients with NCM, the average number of satellites was almost 70, whereas it was only 15 for patients without NCM.
Among the 334 patients currently analyzed in the Nevus Outreach Registry, 50% of their parents reported that they had the nevi removed out of fear of melanoma, and 30% said they had them removed primarily for cosmetic reasons. About 20% of patients also had satellite nevi removed to prevent melanoma, "even though not a single melanoma has ever been reported to have developed within a satellite nevus," Dr. Marghoob commented.
Articles in this issue
over 23 years ago
Tumor-Specific Idiotype Vaccines Promising in B-Cell Lymphomasover 23 years ago
Childhood Survivors May Not Know Their Past Rxover 23 years ago
Pemetrexed/Gemcitabine Promising in Advanced Pancreatic Cancerover 23 years ago
Physician Experience Predicts HIV-Related Mortalityover 23 years ago
Eloxatin With 5-FU/LV Approved for Recurrent Colon Cancerover 23 years ago
Comprehensive Geriatric Evaluations Improve Careover 23 years ago
Nordion’s Monte Carlo Dose Calculation Software Approvedover 23 years ago
No Strong Link Between Breast Cancer Risk and Pollutantsover 23 years ago
Imatinib Inactive in Sarcomas That Lack C-KIT/PDGFNewsletter
Stay up to date on recent advances in the multidisciplinary approach to cancer.