
In this article, we review the data surrounding the use of chemotherapy (CT) and chemoradiotherapy (CRT) in patients with resectable pancreatic cancer.

In this article, we review the data surrounding the use of chemotherapy (CT) and chemoradiotherapy (CRT) in patients with resectable pancreatic cancer.

The treatment of cancer of the anal canal has changed significantly over the past several decades. Although the abdominoperineal resection (APR) was the historical standard of care, a therapeutic paradigm shift occurred with the seminal work of Nigro, who reported that anal canal cancer could be treated with definitive chemoradiation, with APR reserved for salvage therapy only. This remains an attractive approach for patients and physicians alike and the standard of care in this disease. Now, nearly four decades later, a similar approach continues to be utilized, albeit with higher radiation doses; however, this strategy remains fraught with considerable treatment-related morbidities. With the advent of intensity-modulated radiation therapy (IMRT), many oncologists are beginning to utilize this technology in the treatment of anal cancer in order to decrease these toxicities while maintaining similar treatment efficacy. This article reviews the relevant literature leading up to the modern treatment of anal canal cancer, and discusses IMRT-related toxicity and disease-related outcomes in the context of outcomes of conventionally treated anal cancer.
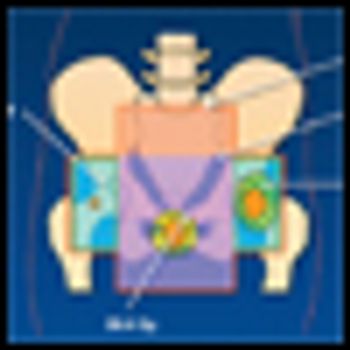
Historically, the treatment of squamous cell carcinoma of the anal canal has been an abdominoperineal resection (APR), resulting in loss of the anus and rectum with need for a permanent colostomy.

Prior to the mid-1980s, patients with rectal cancer usually underwent surgery alone, resulting in high rates of pelvic failure with subsequent morbidity and death.

Epidermal growth factor receptor (EGFR) and vascular endothelial growth factor (VEGF) are often overexpressed in colorectal cancer and are associated with inferior outcomes. Based on successful randomized phase III trials, anti-EGFR and anti-VEGF therapeutics have entered clinical practice. Cetuximab (Erbitux), an EGFR-specific antibody, is currently approved in the United States in combination with irinotecan (Camptosar) for patients with metastatic colorectal cancer refractory to irinotecan or as a single agent for patients unable to tolerate irinotecan-based therapy. In retrospective analyses, patients with EGFR-expressing rectal cancer undergoing neoadjuvant radiation therapy had a significantly inferior disease-free survival and lower rates of achieving pathologic complete response. Based on the positive data in metastatic colorectal cancer and synergy with radiation therapy seen in preclinical models, there is a strong rationale to combine cetuximab with neoadjuvant radiation therapy and chemotherapy in rectal cancer. Bevacizumab (Avastin), a VEGF-specific antibody, was the first antiangiogenic agent to be approved in the United States for use in combination with standard chemotherapy in the first- and second-line of treatment in metastatic colorectal cancer. VEGF-targeted therapy may lead to indirect killing of cancer cells by damaging tumor blood vessels, and may increase the radiosensitivity of tumor-associated endothelial cells. VEGF blockade can also "normalize" tumor vasculature, thereby leading to greater tumor oxygenation and drug penetration. This review will address completed and ongoing trials that have established and continue to clarify the effects of these agents in rectal cancer.

Preliminary results of studies employing hepatic transplantation with radiation therapy are encouraging. Although these new approaches hold promise, the prognosis in patients with biliary cancers remains poor, and the integration of novel therapeutic strategies is indicated.

Colon cancer is a major public health problem. The primary treatment is resection. For patients with early-stage disease, surgery results in excellent survival rates. In contrast, patients with locally advanced tumors arising in "anatomically immobile" segments of large bowel have a less satisfactory outcome, in part secondary to compromised surgical clearance. Patterns-of-failure analyses suggest that for tumors that invade adjacent organs, exhibit perforation or fistula, or are subtotally resected, local failure rates exceed 30%. Multiple single-institution retrospective studies have shown improved local control and possibly survival with the addition of external irradiation and/or intraoperative radiation. In contrast, a recent Intergroup trial failed to show any benefit by the addition of adjuvant radiation therapy combined with chemotherapy. Interpretation of this trial's results is handicapped by low patient accrual. With the advent of novel and more effective systemic therapies for metastatic colon cancer, current and future clinical research will address the efficacy of these agents in the adjuvant setting. Adjuvant radiation therapy should be considered in patients with colon cancer at high risk for local failure.

Drs. Chadha, Kuvshinoff, andJavle have provided a wellwrittenreview of the rationaleand literature supporting neoadjuvanttherapy and gastric cancer.Although the incidence of gastric canceris declining in the United States,approximately 1 million new caseswill be diagnosed worldwide this yearwith over 700,000 deaths, resulting ina disease-related mortality of nearly75%.[1] These figures emphasize theneed for new and improved treatmentstrategies in this disease. In contrastto other gastrointestinal malignancies,there has been little systematic evaluationof neoadjuvant multimodalityapproaches for patients with gastriccancer. Given its natural history andbiology, this approach is logical andmay yield therapeutic benefit.

Drs. Pisters, Wolff, Crane, andEvans have provided an excellentoverview of contemporaryapproaches to staging, surgicalmanagement, and treatment ofpatients with potentially resectablepancreatic cancer. Given the impressiveadvances in our understandingof the biology and genetics of pancreaticcancer, we would agree thatcurrent opportunities for progressagainst this malignancy are encouraging.The reality, however, is thatmortality rates still exceed 95%.While the article addresses the clinicalmanagement of patients with operablepancreatic cancer, this subsetof patients constitutes only 10% to15% of all patients with the disease.This group as well as patients withlocally advanced and metastatic diseaseare in need of new and innovativetreatment strategies. In thisreview, we will highlight several ofthe points made by the authors.

This year, approximately 40% of the 28,300 patients diagnosed with pancreatic carcinoma in the United States will present with locally advanced disease. Radiotherapeutic approaches are often employed, as these patients

November 1st 2000

November 2nd 2008
November 13th 2009

August 1st 2007