COVID-19 Vaccination in Patients With Cancer and Recipients of Cellular Therapy
Fareed Khawaja, MBBS, and colleagues provide a comprehensive overview of COVID-19 vaccine efficacy and safety among patients with cancer in the United States.
ABSTRACT
COVID-19 continues to disproportionately affect patients with cancer because of their underlying immunocompromised state. Strategies to mitigate the impact of COVID-19 on patients with cancer include vaccination, which has demonstrated some level of protection, at least against serious complications such as respiratory failure and death, with limited safety concerns. In this narrative review, we discuss the current COVID-19 vaccines that are available in the United States, the published data regarding vaccine efficacy and safety in patients with cancer, current vaccination guidelines, and future directions.
Oncology (Williston Park). 2023;37(2):69-77.
DOI: 10.46883/2023.25920985
Introduction
Many millions of people have been infected with SARS-CoV-2, the causative pathogen for COVID-19, since the beginning of the pandemic, and more than 6 million people have died as a result of this infection, according to the World Health Organization.1 SARS-CoV-2 may cause severe disease in older and immunocompromised patients, including patients with cancer.2-5 Mortality rates for COVID-19 in patients with cancer are reported to be as high as 36%,3,6 higher than those among the general public.4 Risk factors associated with poor outcomes among patients with cancer who have COVID-19 include advanced age, poor functional status, use of cytotoxic chemotherapy, and having a hematologic cancer.7-9 Recipients of hematopoietic cell transplants (HCT) and of chimeric antigen receptor (CAR) T cells are also at increased risk for COVID-19–related complications.10 Among the multiple strategies devised to protect this vulnerable population are mass vaccinations, prompt therapy, enhanced infection control, early testing, public health protocols, and, when available, monoclonal antibodies, both pre- and post-exposure.
The rapid development of the COVID-19 pandemic prompted the use of novel vaccine platforms. At present, 3 different types of COVID-19 vaccines are available: mRNA vaccines, adenoviral vector–based vaccines, and protein subunit vaccines. The FDA has approved only 2 mRNA-based vaccines (BNT162b2, Pfizer/BioNTech; and mRNA-1273, Moderna), 1 adenoviral vector–based vaccine (Ad26.COV2.S, Janssen), and 1 protein subunit–based vaccine (NVX-CoV2373, Novavax), all under formal authorization or emergency use authorization (EUA) (Table 1). The ChAdOx1 nCoV-19 vaccine (adenoviral vector–based platform; Oxford University-AstraZeneca) has yet to be approved in the United States but is available in the European Union and United Kingdom.
TABLE 1. The Current Status of COVID-19 Vaccines in the United States
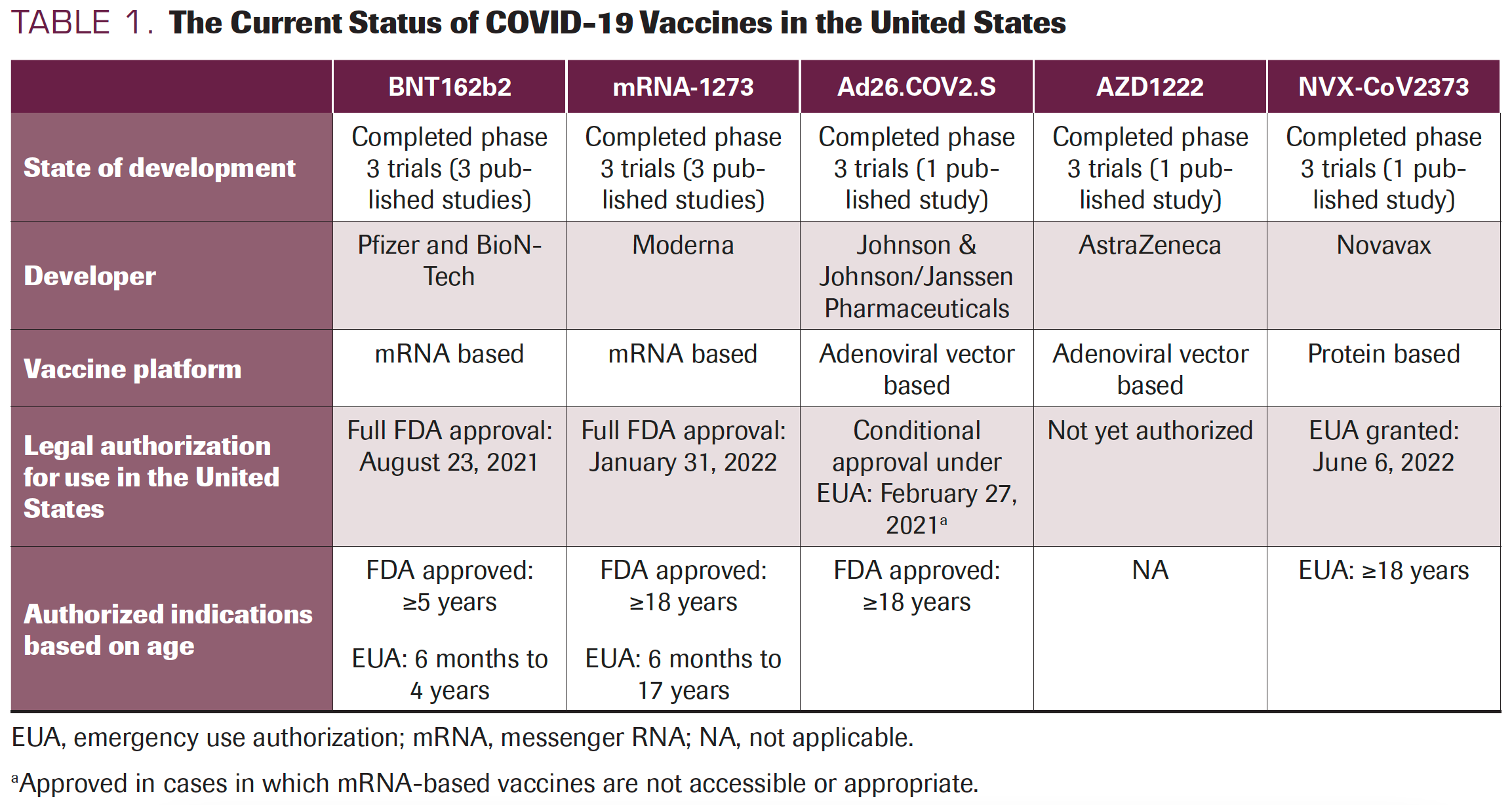
The BNT162b2 and mRNA-1273 vaccines are lipid nanoparticle–formulated mRNA vaccines encoding the SARS-CoV-2 spike protein, which mediates attachment of the virus to the host cell11 as illustrated in Figure 1. Both vaccines underwent rigorous phase 3 testing in the general population and demonstrated high rates of protection against symptomatic COVID-19 (BNT162b2, 95%; mRNA-1273, 94%), with no patients experiencing severe COVID-19 after 2 doses.12,13 The FDA granted EUAs for BNT162b2 and mRNA-1273 on December 11, 2020, and December 18, 2020, respectively, making them the first available COVID-19 vaccines in the United States. Ad26.COV2.S is based on an adenoviral vector expressing the SARS-CoV-2 spike glycoprotein11 as illustrated in Figure 2. The efficacy rate for this vaccine has been lower than those for both mRNA-based vaccines, with a rate of 81.7% against severe to critical COVID-19 at 28 days using a 1-dose schedule.14 All phase 3 trials of these 3 vaccines excluded patients who were immunocompromised, including patients with cancer receiving active therapy and transplant recipients. These studies did not account for the emergent new variants such as Delta, Omicron, and the Omicron subvariants, and the resultant reduction in vaccine efficacy.15
Because large clinical trials of COVID-19 vaccination in patients with cancer are lacking, this review focuses on pertinent data regarding vaccine efficacy and safety in this population and in cellular therapy recipients, and it discusses current vaccination guidance in the United States.
FIGURE 1. Schematic of a COVID-19 mRNA Vaccine
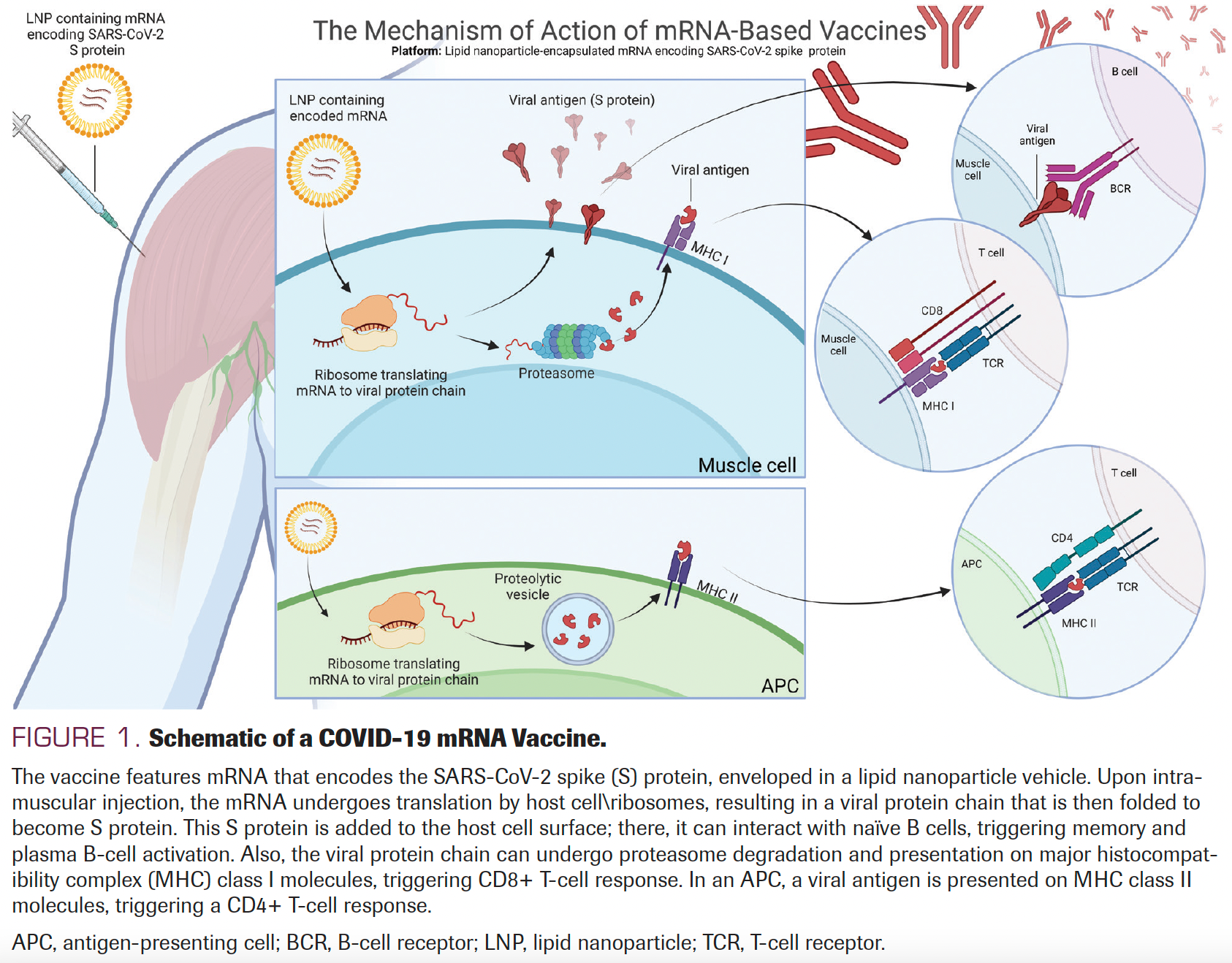
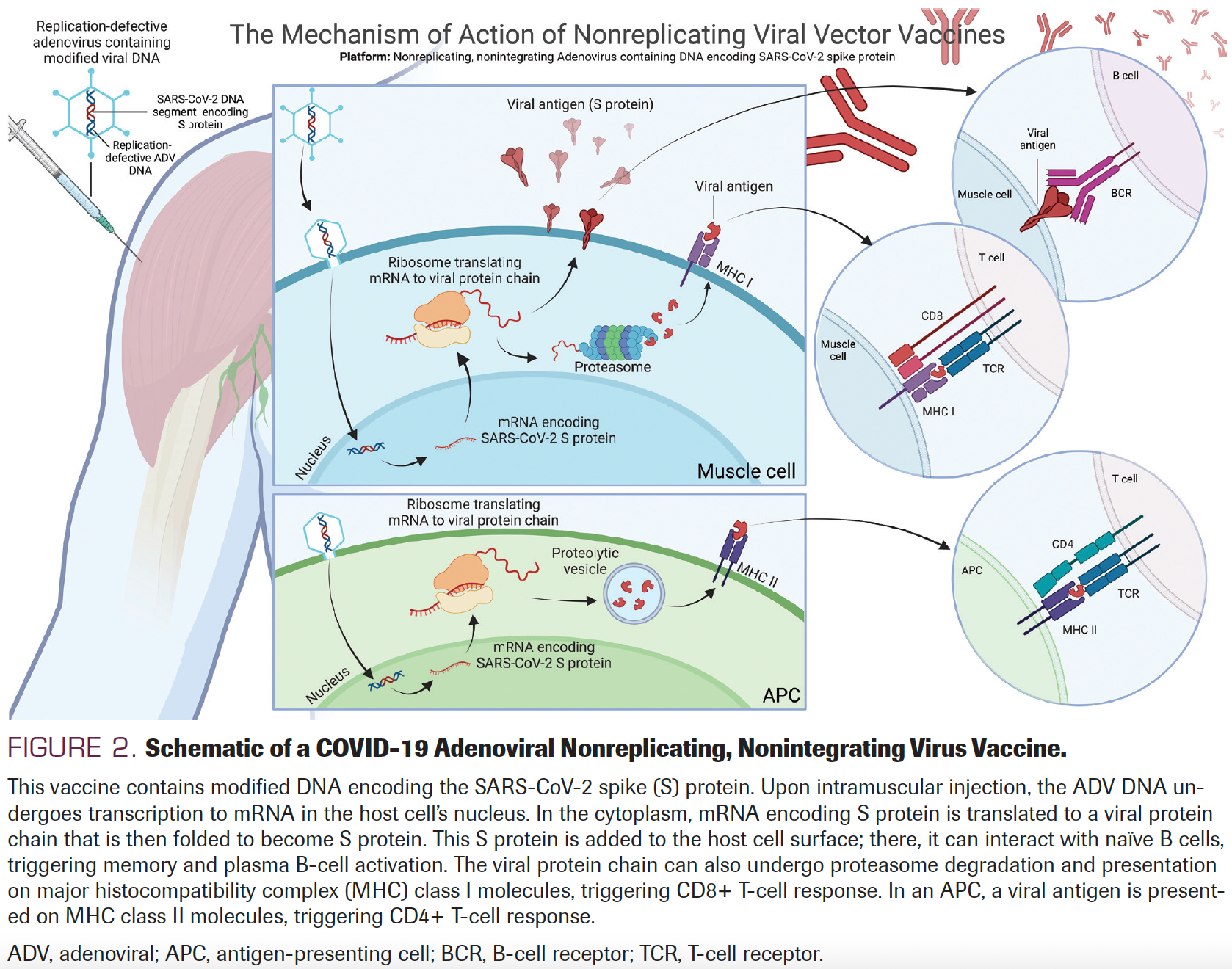
FIGURE 2. Schematic of a COVID-19 Adenoviral Nonreplicating, Nonintegrating Virus Vaccine
Efficacy of Vaccines by Underlying Cancer and Therapy
Various studies have assessed the efficacy of COVID-19 vaccinations in patients with different solid tumors; most focused on seroconversion as the primary outcome. Also, most highlighted the poor immunogenicity of a single dose of either the BNT162b2 or mRNA-1273 vaccine in these patients.16-18 After a single dose of the BNT162b2 vaccine in patients with solid tumors undergoing active therapy in 2 studies in France, the seropositivity rates were 47.5% and 55%, respectively, compared with 100% in patients without cancer.16,17 In other studies, the seropositivity rate increased significantly and was greater than 90% after the second dose of either mRNA-based vaccine in patients with solid tumors.16,18-21 Postvaccination antibody titers in patients with solid tumors differed among studies, as some showed lower median antibody titers in patients with solid tumors than in patients without cancer,16 whereas others showed similar titers.19,22 These differences are likely due to differences in therapy, cancer stage, and vaccination timing in relation to cancer therapy.
Patients With Hematologic Cancer
Compared with solid tumors, hematologic cancers have been associated with worse COVID-19–related outcomes.2,23-25 Patients with hematologic cancers were not included in large vaccine trials; however, smaller trials investigated COVID-19 vaccine efficacy in these patients.18,19,25 Monin et al reported an increase in the seropositivity rate from 18% after the first dose of BNT162b2 to 60% after the second dose.18 Importantly, most studies including patients with hematologic cancers showed that they had lower seropositivity rates compared with patients with solid tumors or healthy controls.19,26,27 For example, Thakkar et al reported a seropositivity rate of 85% in patients with hematologic cancers, which was markedly lower than the rate of 98% in patients with solid tumors after 2 doses of either mRNA vaccine or 1 dose of the Ad26.COV2.S vaccine.19 Also, in an age- and sex-matched analysis, patients with chronic lymphocytic leukemia or small lymphocytic lymphoma had a considerably lower seropositivity rate than did patients without cancer.27
Patients Undergoing Cytotoxic Therapy
Recent and/or active cytotoxic chemotherapy has been associated with suboptimal serologic responses to COVID-19 vaccines in most studies.21 Addeo et al reported that, after both the first and second mRNA vaccine doses, patients with either hematologic or solid-tumor cancer who were receiving cytotoxic therapy had lower seropositivity rates than did patients with cancer who were undergoing active surveillance (69% vs 86% and 93% vs 98%, respectively); patients with hematologic cancers had lower seroconversion rates and antibody titers than did patients with solid tumors.21 Similarly, Thakkar et al reported that patients with solid tumors or hematologic cancer undergoing cytotoxic chemotherapy had a lower seropositivity rate after a complete series of the BNT162b2 (2 doses), mRNA-1273 (2 doses), or Ad26.COV2.S (1 dose) vaccine than did patients with cancer receiving other types of cancer therapy (eg, hormone therapy, immunotherapy; 92% vs 99%; P = .04).19 Some study results have suggested that chemotherapy does not impact vaccine effectiveness,19,20 but these studies had small sample size and made no clear distinction between cytotoxic therapy and other types of cancer therapy, which may explain the reported inconsistencies in response rates.
Patients Undergoing Immunotherapy
Data regarding the effects of immunotherapy on COVID-19 vaccine responses in patients with cancer have been mixed.20 Massarweh et al evaluated the immediate humoral response to 2 doses of the BNT162b2 vaccine in 102 patients with solid tumors and in 78 healthy controls.20 The median level of SARS-CoV-2 spike antibodies was lower in the patients than in the controls (1931 AU/mL [IQR, 509-4386 AU/mL] vs 7160 AU/mL [IQR, 3129-11,241 AU/ mL]; P < .001). Also, the combination of chemotherapy and immunotherapy was the only variable associated with low antibody titers upon multivariate analysis.27 In a follow-up study to assess the durability of antibody responses over 4 months, patients with cancer undergoing immunotherapy + chemotherapy, or immunotherapy + biologic therapy, had the lowest titers (median, 94.4 AU/ mL [IQR, 49.4-191.0 AU/mL] and median, 147.0 AU/mL [IQR, 62.8-339.0 AU/mL], respectively), compared with other patients with cancer.28 Exploratory multivariate analysis identified chemotherapy plus immunotherapy and immunotherapy plus biologic therapy as risk factors for low titers 4 months after completing a COVID-19 vaccination series. In contrast, larger, more robust studies,29-31 such as the VOICE trial, assessed the efficacy of the mRNA-1273 vaccine in patients with cancer who were actively undergoing therapy.29 In those studies, response rates based on serum titers were highest in the immunotherapy group (n = 130; 93%) followed by the chemotherapy/ immunotherapy group (n = 143; 89%) and the chemotherapy group (n = 223; 84%). Notably, the humoral response rates of all 3 groups were not inferior to that of a group of healthy participants.29 The discrepancies in response rates between these studies and previous ones may have resulted from smaller numbers of patients in earlier cohorts as well as the additional immunosuppression related to co-administration of agents such as cytotoxic chemotherapeutics.
Recipients of Anti-CD20 Therapy or Cellular Therapy
The results of a few studies have indicated that the use of anti-CD20 agents, such as rituximab, may be associated with reduced immunogenic responses to COVID-19 vaccines.32,33 In the United Kingdom–based CAPTURE study of patients with cancer who received 2 doses of either the BNT162b2 or AstraZeneca AZD1222 vaccine, receipt of anti-CD20 therapy within 12 months after vaccination was associated with reduced titers among patients with hematologic cancers undergoing different treatment types.33 In another study including 87 individuals with hematologic cancers who received anti-CD20 therapy within 12 months of 2 doses of the BNT162b2 vaccine, the patients had negligible median serologic titers, and some experienced severe breakthrough COVID-19.34
HCT recipients have had mixed responses to the COVID-19 vaccines. In the CAPTURE study, HCT recipients and other patients with hematologic cancers had similar antibody titers within 6 months of vaccination.33 The timing of HCT may affect vaccine efficacy, with study data demonstrating poorer immunologic responses in patients with recent transplants and better responses in patients vaccinated at least 12 months after HCT.34,35 The type of transplant impacts vaccine efficacy as well, with better humoral responses after autologous HCT than after allogeneic HCT.35,36
Although some studies found that CAR T-cell recipients had serologic responses to COVID-19 vaccination similar to those of patients with hematologic cancer undergoing chemotherapy,33 most found lower seropositivity rates among the patients who received CAR T-cell therapy.19,35,37 The results of one study showed that 79% of CAR T-cell recipients had no appreciable immune responses after completing a primary vaccination series with 2 doses of either of the mRNA vaccines.35
Strategies to Improve COVID-19 Vaccine Efficacy in Patients With Cancer
Because of the reduced efficacy of COVID-19 vaccines in patients with cancer, new strategies are needed to increase vaccine immune responses. Additionally, the evolution of SARS CoV-2 into different variants has reduced vaccine efficacy and protection in previously vaccinated patients, resulting in part from immune evasion.38 Breakthrough infections in patients with cancer are associated with higher mortality rates and more severe complications than in immunocompetent patients.6,39 Optimizing the timing of vaccination, the use of additional and/ or booster doses, and heterologous vaccinations are strategies that may improve vaccine immune responses.
Optimal timing of vaccination after cytotoxic therapy, anti-CD20 therapy, or cellular therapy may improve vaccine efficacy.22,40 In a subanalysis of the phase 3 BNT162b2 vaccine trial, 3813 patients with a history of solid tumors (predominantly breast or prostate cancer) who were no longer undergoing active therapy had a vaccine efficacy rate of 94.4% at 6 months of follow-up.22 In patients with cancer undergoing active therapy, however, timing of vaccination may prove to be more complicated, as many patients may end up getting vaccinated while receiving therapy. Vaccination at least 6 months after anti-CD20 therapy may provide better immune responses.21 Vaccination at least 3 months after HCT or CAR T-cell therapy may provide superior immune responses,35 especially for autologous HCT recipients.36
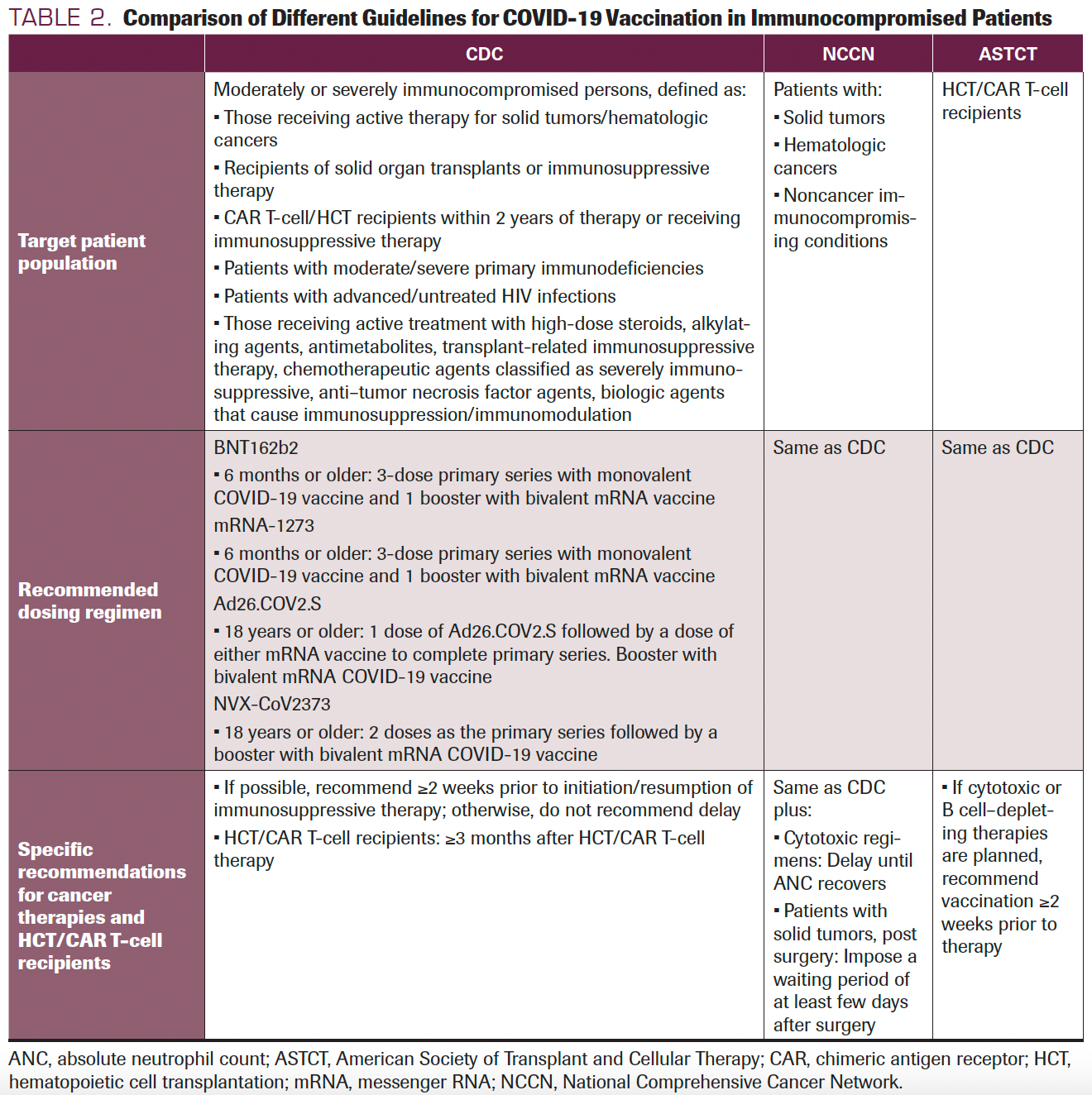
Additional or booster doses of COVID-19 vaccines have optimized serologic responses and may reduce the rate of breakthrough infections in previously vaccinated healthy adults.41 Boosters of mRNA vaccines were also effective in preventing COVID-19 complications with the emergence of recent SARS CoV-2 variants, such as the Omicron variant.42 Among patients with cancer, data on the efficacy of boosters are limited to the BNT162b2 vaccine.43-46 Of 20 patients with solid tumors who received a third dose of the BNT162b2 vaccine as a booster,16 had increased humoral but not cellular responses.43 Other studies noted a poor seroconversion rate in patients with hematologic cancer (29.7%) after a third dose of BNT162b2.44 Clinical studies translating the benefits of 1 or more booster doses in patients with cancer are still lacking. Additionally, due to the increased prevalence of the Omicron subvariants such as BA.4/BA.5 and subsequent immune escape to the available vaccines, 2 new bivalent vaccines that carry modified RNA from both the original Wuhan-Hu-1 strain and the Omicron BA.4/BA.5 strains were tested in clinical trials and granted FDA approval under EUA on August 29, 2022, based on preliminary data.47 The process to produce these mRNA vaccines is the same as for the monovalent mRNA vaccines, and no new safety concerns are expected. The CDC and many professional societies, such as the American Society for Transplantation and Cellular Therapy (ASTCT) and the National Comprehensive Cancer Network (NCCN), have recommended additional and booster doses for patients with cancer after primary vaccination (Table 2).
TABLE 2. Comparison of Different Guidelines for COVID-19 Vaccination in Immunocompromised Patients
Mixing COVID-19 vaccines or heterologous vaccine boosters has been considered as a potential strategy to boost immune responses to the vaccines.48 In a recent study, vaccine response was increased in immunocompetent individuals who received heterologous booster vaccination, with an increase in titers by a factor of 6 to 73, and they had prolonged cellular responses.48 On the other hand, among 32 patients with hematologic cancer who did not have responses to the original series of mRNA COVID-19 vaccines and had a booster dose of the Ad26.COV2.S COVID-19 vaccine,49 31% had serologic responses.50 The improvement in humoral response in cancer patients is promising, but more data are needed before adopting heterologous COVID-19 vaccine boosters as a preferred strategy, as the impact of this on clinical outcomes and protection against infection with SARS-CoV-2 variants remains unclear. On the other hand, mixing booster mRNA vaccines in patients with cancer is indicated when access to specific vaccines is constrained.
Safety of COVID-19 Vaccines in Patients With Cancer
The safety of COVID-19 vaccines has been well studied. The most common adverse effects (AEs) reported in the general population include pain at the injection site, fever, and headaches.12-14,51,52 Hypersensitivity related to vaccine administration is uncommon, with rates as low as 2.5 to 4.5 cases per 1 million injections.53 Authors have reported notable AEs in few patients, including Bell palsy, idiopathic thrombocytopenia, acute disseminated encephalomyelitis, myocarditis, pericarditis, Guillain-Barré syndrome, transverse myelitis, and acute myocardial infarction.54 Safety data for patients with cancer are limited because of their exclusion from the initial COVID-19 vaccine trials, but post marketing data are becoming available.55-63
Waissengrin et al compared the AEs of check point inhibitors (CPIs) in 137 patients with solid tumors and a control group of healthy participants after they received the first and second doses of the BNT162b2 vaccine. The rate of myalgia was higher in patients with cancer, but the researchers identified no CPI-mediated toxic effects during short-term follow-up.55 On the other hand, 1 patient in a different study who underwent treatment of colorectal cancer with CPIs had cytokine release syndrome after BNT162b2 vaccination that responded to steroid-based therapy.56 It was unclear whether CPI use contributed to this event or if it was driven by COVID-19 vaccination. Long-term safety follow-up after COVID-19 vaccination in patients receiving CPIs or other active therapy for solid tumors is necessary to better understand the associations among COVID-19 vaccination, vaccine AEs, and patient outcomes; so far, however, the COVID-19 vaccines appear to be safe in these patients.
Many patients with cancer have been administered the mRNA and adenovirus-based COVID-19 vaccines since their initial release.57-59 In a large survey of 1094 patients with solid tumors, the reported AEs for COVID-19 vaccines were similar to those in patients without cancer.59 Investigators noted similar findings in prospective trials that included patients with breast cancer.58 Similarly, multiple studies have demonstrated the safety of COVID-19 vaccines in patients with hematologic malignancies,50,60-63 with the rate of serious AEs ranging from 0% to 7.5%.50,61 The most common AEs have included pain at the injection site, fatigue, joint pain, and fever.60-63 Episodes of thrombocytopenia or thrombosis have yet to be reported.61 Immunologic responses based on antibody titers and the rate of safety events have no significant relationship, suggesting that the degree of immunologic response to the vaccines does not correlate with safety.61,63 In addition, authors have documented the safety of heterologous COVID-19 vaccine boosters in immunocompetent recipients.49 However, vaccine safety data for patients with hematologic cancers are currently limited to 4 to 6 weeks after vaccination, with a lack of long-term follow-up data.
Recipients of CAR T-cell therapy or of autologous or allogeneic HCT may experience toxic effects related to their specific therapies. Different transplant centers have reported limited AEs related to COVID-19 vaccinations.64-70 Early data for HCT recipients who received 2 doses of the mRNA COVID-19 vaccines demonstrated only mild AEs, similar to those in the general population.64,65,67 The most common AEs included pain at the injection site, headaches, fatigue, joint pain, and fever.65,67 Among allogeneic HCT recipients, development of graft-vs-host disease (GVHD) or exacerbation of GVHD can complicate post transplantation care. Whether chronic GVHD is related to COVID-19 vaccination is unclear. No data have established a direct link; reports from some centers noted that about 6% to 12% of vaccine recipients had chronic GVHD after vaccination,69-71 although the investigators did not study comparator groups.68,69 Authors of one study reported graft failure in HCT recipients that was potentially related to COVID-19 vaccination, with some reports of neutropenia or lymphopenia occurring after COVID-19 vaccination.69,70 No thrombotic AEs after vaccination have been reported.
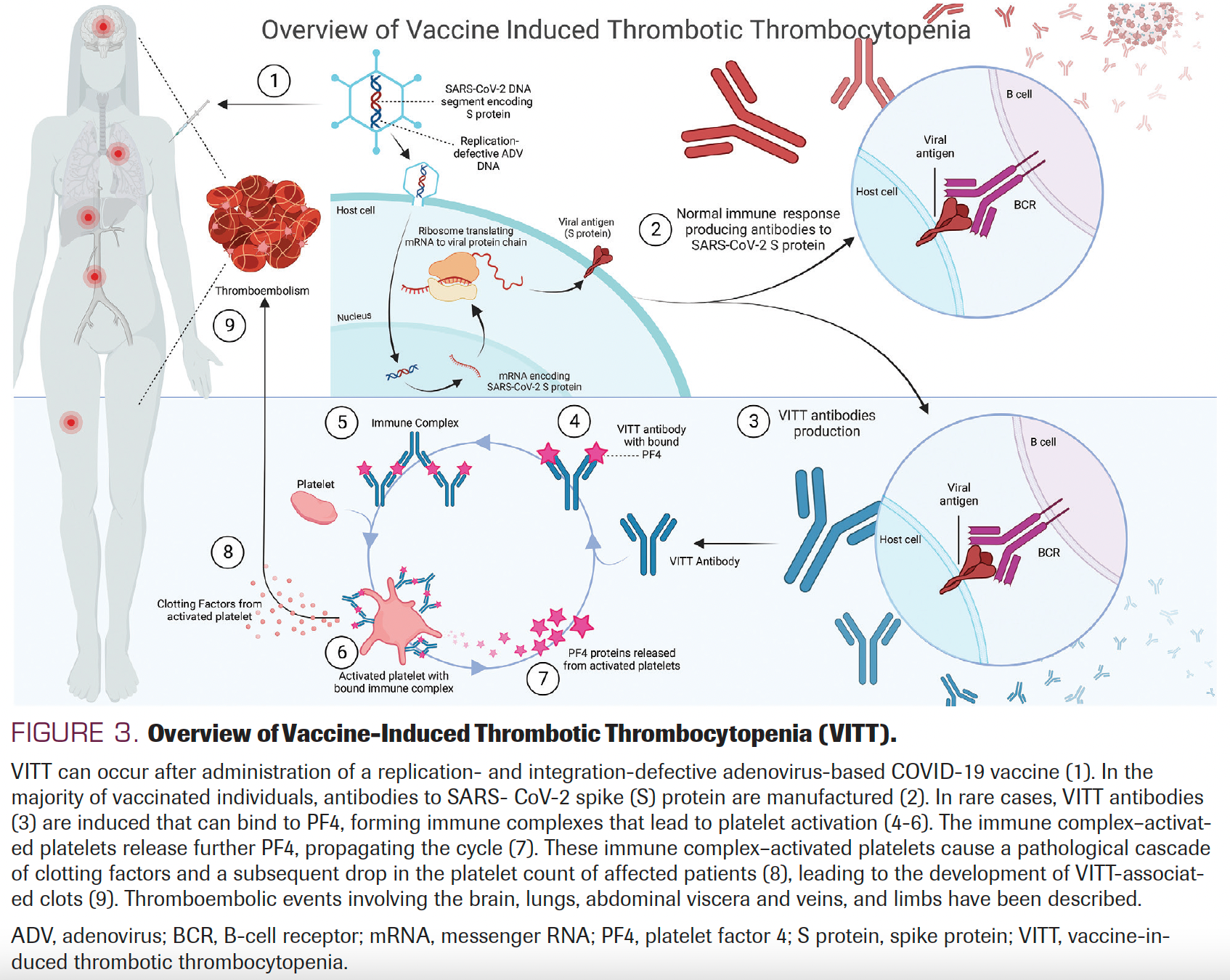
Vaccine-induced immune thrombotic thrombocytopenia (VITT) is a dreaded major AE described with the use of adenoviral vector– based COVID-19 vaccines, such as Ad26.COV2.S and ChAdOx1 nCov-19.72,73 Figure 3 illustrates the possible pathway of VITT based on platelet factor 4 formation. VITT events are very rare in patients with cancer after vaccination.72,73 The few reported cases of VITT in patients with cancer occurred in those with solid tumors.73 COVID-19–related thrombosis is more common than VITT but is still a rare AE.74,75 The mortality rate in patients who develop sinus thrombosis as a result of COVID-19 vaccination is about 50%.72 Because of the low risk-to-benefit ratio COVID-19 vaccines, preferably the mRNA ones, are highly recommended for patients with cancer to at least prevent severe infections and mortality.
FIGURE 3. Overview of Vaccine-Induced Thrombotic Thrombocytopenia (VITT)
Current Recommendations for COVID-19 Vaccination in Patients With Cancer
The CDC and NCCN have made recommendations for COVID-19 vaccination in patients with cancer.76,77 In addition, the ASTCT has provided guidance regarding COVID-19 vaccination in HCT and CAR T-cell recipients. All these organizations agree that COVID-19 vaccination is beneficial to patients with cancer and encourage all such patients to undergo vaccination. Their guidelines are often aligned, but they do provide unique guidance for different groups. Table 2 compares the different guidelines for COVID-19 vaccination in immunocompromised patients.
As of September 2, 2022, the CDC recommends that patients with cancer and recipients of cellular therapy receive a monovalent primary series (consisting of 3 mRNA vaccine doses or 1 adenoviral vector–based and 1 mRNA vaccine dose), with an updated recommendation to include a bivalent BNT162b2 or mRNA-1273 booster dose for those 12 years or older at least 2 months after the last dose of the primary vaccine series. According to these latest guidelines, the bivalent booster dose may obviate the need for multiple booster doses. This new vaccination regimen including the bivalent booster does not have a clear clinical benefit yet, but based on prior serologic studies, it may provide better protection against COVID-19 compared with the regimen that included monovalent boosters. The CDC does not provide specific guidance for different types of cancer.
Among patients with cancer who undergo surgery, vaccination is recommended within a few days after surgery because of the patient’s lack of immunosuppression. Patients with hematologic cancer are advised to undergo vaccination when their absolute neutrophil counts recover. All vaccination guidelines recommend boosters for patients with cancer, with a preference for the mRNA vaccines regardless of the primary vaccine series.77 Specifically, the ASTCT recommends that recipients of cellular therapy receive vaccination against COVID-19 3 months after conditioning therapy. Revaccination is also recommended for patients who were vaccinated prior to cellular therapy.78
Future Directions
Prevention of COVID-19 using safe, effective vaccines continues to be paramount in patients with cancer. The introduction of the new bivalent mRNA COVID-19 vaccines may lead to better protection at the time when BA.4/BA.5 subvariants are dominant,47,79 although little is known about whether their timing in relation to cancer treatment and cellular therapy will affect humoral responses, as was described with the monovalent mRNA COVID-19 vaccines.21 Indeed, the FDA, in their fact sheets on bivalent mRNA vaccines, provided a disclaimer that immunocompromised patients may not have effective responses to the new boosters.47 In addition, safety data for patients with cancer have not been well investigated, and patients therefore should be observed closely post vaccination for short- and long-term adverse effects.
Other options for COVID-19 prevention in patients with cancer are monoclonal antibodies that provide passive immunity. At this time, only tixagevimab-cilgavimab (Evusheld) is approved under EUA for pre-exposure prophylaxis based on data for patients at high risk for inadequate response to COVID-19 vaccination. Very few patients with cancer were included in the original phase 3 trial of Evusheld, yet it is recommended for these patients.80 Studies demonstrated that the effectiveness of Evusheld was retained against the SARS-CoV-2 Omicron variants with adjustments in dosing, but those studies were limited to mouse models.81 Experience with Evusheld in immunocompromised patients has demonstrated reductions in severe COVID-19 and in hospitalization.82,83 Because of a lack of clinical efficacy data regarding protection against the Omicron subvariants, there is some doubt regarding future use of Evusheld.84,85 New Omicron subvariants such as BQ.1 and BQ.1.1 have demonstrated neutralizing antibody escape, imperiling the future use of Evusheld and probably bebtelovimab.85 Monoclonal antibodies under development should provide a wider range of neutralizing capabilities for the circulating and future variants and subvariants.86
Stimulating the immune system to protect patients with cancer from severe COVID-19 is also a suggested prophylactic measure.87,88 Theoretically, the use of live vaccines such as Bacille Calmette-Guérin could enhance response to COVID-19 vaccines and defend against severe COVID-19, and data from early randomized controlled trials did demonstrate some benefits of Bacille Calmette-Guérin in terms of COVID-19 protection.88 However, live vaccines are contraindicated in patients with cancer undergoing active therapy, so a Canadian trial is investigating the use of the immunotherapeutic drug IMM-101 to stimulate the immune system of such patients.89 So far, firm evidence supporting the use of any of these methods to enhance COVID-19 vaccination is lacking.
Conclusions
Patients with cancer and recipients of cellular therapy are at increased risk for COVID-19–related complications. Many strategies to protect these patients against COVID-19 are available, and the currently available COVID-19 vaccines provide hope. Despite reports of suboptimal serologic responses to COVID-19 vaccines, serious COVID-19–related complications may be prevented. Beyond the basic vaccine series, various strategies—such as the use of multiple boosters (homozygous or heterozygous), optimal timing of vaccination, and repeating the original vaccine series after transplantation—may provide further protection. Other strategies for protection against severe COVID-19 disease in vaccine nonresponders are needed, such as the use of pre-exposure monoclonal anti-COVID-19 antibodies.
AUTHOR AFFILIATIONS:
Fareed Khawaja, MBBS1; Marilyne Daher, MD2; Amy Spallone, MD1; and Roy F. Chemaly MD, MPH1
1Department of Infectious Diseases, Infection Control, and Employee Health, The University of Texas MD Anderson Cancer Center, Houston, TX.
2Department of Internal Medicine, Baylor College of Medicine, Houston, TX.
CORRESPONDING AUTHOR:
Fareed Khawaja, MBBS
Department of Infectious Diseases, Infection Control, and Employee Health Unit 1460
The University of Texas MD Anderson Cancer Center
1515 Holcombe Blvd
Houston, TX 77030
Tel: 281-610-023
Email: fkhawaja@mdanderson.org
DISCLOSURES:
FK has received honoraria from Medscape and research funding from Merck. MD and AS have nothing to disclose. RFC has served as a consultant, speaker, or advisor for Adagio Therapeutics, ADMA Biologics, Ansun Pharmaceuticals, Astellas, Genentech, Janssen, Karius, MSD, Oxford Immunotec, Partner Therapeutics, Pulmotect, Shionogi, and Takeda, and has received research grants paid to his institution from AiCuris, Ansun Pharmaceuticals, Eurofins Viracor, Genentech, Karius, MSD, Oxford Immunotec, and Takeda.
REFERENCES
- WHO coronavirus (COVID-19) dashboard. World Health Organization (WHO). Accessed on December 14, 2022. https://covid19.who.int/
- Wang Q, Berger NA, Xu R. Analyses of risk, racial disparity, and outcomes among US patients with cancer and COVID-19 infection. JAMA Oncol. 2021;7(2):220-227. doi:10.1001/jamaoncol.2020.6178
- Saini KS, Tagliamento M, Lambertini M, et al. Mortality in patients with cancer and coronavirus disease 2019: a systematic review and pooled analysis of 52 studies. Eur J Cancer. 2020;139:43-50. doi:10.1016/j.ejca.2020.08.011
- Rugge M, Zorzi M, Guzzinati S. SARS-CoV-2 infection in the Italian Veneto region: adverse outcomes in patients with cancer. Nat Cancer. 2020;1(8):784-788. doi:10.1038/s43018-020-0104-9
- Kodde C, Bonsignore M, Schöndube D, et al. Mortality in cancer patients with SARS-CoV-2 or seasonal influenza: an observational cohort study from a German-wide hospital network. Infection. Published online June 3, 2022. doi:10.1007/s15010-022-01852-5
- Wang W, Kaelber DC, Xu R, Berger NA. Breakthrough SARS-CoV-2 infections, hospitalizations, and mortality in vaccinated patients with cancer in the US between December 2020 and November 2021. JAMA Oncol. 2022;8(7):1027-1034. doi:10.1001/jamaoncol.2022.1096
- Grivas P, Khaki AR, Wise-Draper TM, et al. Association of clinical factors and recent anticancer therapy with COVID-19 severity among patients with cancer: a report from the COVID-19 and Cancer Consortium. Ann Oncol. 2021;32(6):787-800. doi:10.1016/j.annonc.2021.02.024
- Robilotti EV, Babady NE, Mead PA, et al. Determinants of COVID-19 disease severity in patients with cancer. Nat Med. 2020;26(8):1218-1223. doi:10.1038/s41591-020-0979-0
- Mehta V, Goel S, Kabarriti R, et al. Case fatality rate of cancer patients with COVID-19 in a New York hospital system. Cancer Discov. 2020;10(7):935-941. doi:10.1158/2159-8290.CD-20-0516
- Shah GL, DeWolf S, Lee YJ, et al. Favorable outcomes of COVID-19 in recipients of hematopoietic cell transplantation. J Clin Invest. 2020;130(12):6656-6667. doi:10.1172/JCI141777
- Hwang JK, Zhang T, Wang AZ, Li Z. COVID-19 vaccines for patients with cancer: benefits likely outweigh risks. J Hematol Oncol. 2021;14(1):38. doi:10.1186/s13045-021-01046-w
- Baden LR, El Sahly HM, Essink B, et al; COVE Study Group. Efficacy and safety of the mRNA-1273 SARS-CoV-2 vaccine. N Engl J Med. 2021;384(5):403-416. doi:10.1056/NEJMoa2035389
- Polack FP, Thomas SJ, Kitchin N, et al; C4591001 Clinical Trial Group. Safety and efficacy of the BNT162b2 mRNA Covid-19 vaccine. N Engl J Med. 2020;383(27):2603-2615. doi:10.1056/NEJMoa2034577
- Sadoff J, Gray G, Vandebosch A, et al; ENSEMBLE Study Group. Safety and efficacy of single-dose Ad26.COV2.S vaccine against Covid-19. N Engl J Med. 2021;384(23):2187-2201. doi:10.1056/NEJMoa2101544
- Accorsi EK, Britton A, Fleming-Dutra KE, et al. Association between 3 doses of mRNA COVID-19 vaccine and symptomatic infection caused by the SARS-CoV-2 Omicron and Delta variants. JAMA. 2022;327(7):639-651. doi:10.1001/jama.2022.0470
- Barrière J, Chamorey E, Adjtoutah Z, et al. Impaired immunogenicity of BNT162b2 anti-SARS-CoV-2 vaccine in patients treated for solid tumors. Ann Oncol. 2021;32(8):1053-1055. doi:10.1016/j.annonc.2021.04.019
- Palich R, Veyri M, Marot S, et al. Weak immunogenicity after a single dose of SARS-CoV-2 mRNA vaccine in treated cancer patients. Ann Oncol. 2021;32(8):1051-1053. doi:10.1016/j.annonc.2021.04.020
- Monin L, Laing AG, Muñoz-Ruiz M, et al. Safety and immunogenicity of one versus two doses of the COVID-19 vaccine BNT162b2 for patients with cancer: interim analysis of a prospective observational study. Lancet Oncol. 2021;22(6):765-778. doi:10.1016/S1470-2045(21)00213-8
- Thakkar A, Gonzalez-Lugo JD, Goradia N, et al. Seroconversion rates following COVID-19 vaccination among patients with cancer. Cancer Cell. 2021;39(8):1081-1090.e2. doi:10.1016/j.ccell.2021.06.002
- Massarweh A, Eliakim-Raz N, Stemmer A, et al. Evaluation of seropositivity following BNT162b2 messenger RNA vaccination for SARS-CoV-2 in patients undergoing treatment for cancer. JAMA Oncol. 2021;7(8):1133-1140. doi:10.1001/jamaoncol.2021.2155
- Addeo A, Shah PK, Bordry N, et al. Immunogenicity of SARS-CoV-2 messenger RNA vaccines in patients with cancer. Cancer Cell. 2021;39(8):1091-1098.e2. doi:10.1016/j.ccell.2021.06.009
- Thomas SJ, Perez JL, Lockhart SP, et al. Efficacy and safety of the BNT162b2 mRNA COVID-19 vaccine in participants with a history of cancer: subgroup analysis of a global phase 3 randomized clinical trial. Vaccine. 2022;40(10):1483-1492. doi:10.1016/j.vaccine.2021.12.046
- Pinato DJ, Zambelli A, Aguilar-Company J, et al. Clinical portrait of the SARS-CoV-2 epidemic in European cancer patients. Cancer Discov. 2020;10(10):1465-1474. doi:10.1158/2159-8290.CD-20-0773
- Dai M, Liu D, Liu M, et al. Patients with cancer appear more vulnerable to SARS-CoV-2: a multicenter study during the COVID-19 outbreak. Cancer Discov. 2020;10(6):783-791. doi:10.1158/2159-8290.CD-20-0422
- He W, Chen L, Chen L, et al. COVID-19 in persons with haematological cancers. Leukemia. 2020;34(6):1637-1645. doi:10.1038/s41375-020-0836-7
- Wu JT, La J, Branch-Elliman W, et al. Association of COVID-19 vaccination with SARS-CoV-2 infection in patients with cancer: a US nationwide veterans affairs study. JAMA Oncol. 2022;8(2):281-286. doi:10.1001/jamaoncol.2021.5771
- Herishanu Y, Avivi I, Aharon A, et al. Efficacy of the BNT162b2 mRNA COVID-19 vaccine in patients with chronic lymphocytic leukemia. Blood. 2021;137(23):3165-3173. doi:10.1182/blood.2021011568
- Eliakim-Raz N, Massarweh A, Stemmer A, Stemmer SM. Durability of response to SARS-CoV-2 BNT162b2 vaccination in patients on active anticancer treatment. JAMA Oncol. 2021;7(11):1716-1718. doi:10.1001/jamaoncol.2021.4390
- Oosting SF, van der Veldt AAM, GeurtsvanKessel CH, et al. mRNA-1273 COVID-19 vaccination in patients receiving chemotherapy, immunotherapy, or chemoimmunotherapy for solid tumours: a prospective, multicentre, non-inferiority trial. Lancet Oncol. 2021;22(12):1681-1691. doi:10.1016/S1470-2045(21)00574-X
- Fenioux C, Teixeira L, Fourati S, et al. SARS-CoV-2 antibody response to 2 or 3 doses of the BNT162b2 vaccine in patients treated with anticancer agents. JAMA Oncol. 2022;8(4):612-617. doi:10.1001/jamaoncol.2021.7777
- Sharafeldin N, Bates B, Song Q, et al. Outcomes of COVID-19 in patients with cancer: report from the National COVID Cohort Collaborative (N3C). J Clin Oncol. 2021;39(20):2232-2246. doi:10.1200/JCO.21.01074
- Ghione P, Gu JJ, Attwood K, et al. Impaired humoral responses to COVID-19 vaccination in patients with lymphoma receiving B-cell-directed therapies. Blood. 2021;138(9):811-814. doi:10.1182/blood.2021012443
- Fendler A, Shepherd STC, Au L, et al. Adaptive immunity and neutralizing antibodies against SARS-CoV-2 variants of concern following vaccination in patients with cancer: the CAPTURE study. Nat Cancer. 2021;2:1321-1337. doi:10.1038/s43018-021-00274-w
- Maneikis K, Šablauskas K, Ringelevičiūtė U, et al. Immunogenicity of the BNT162b2 COVID-19 mRNA vaccine and early clinical outcomes in patients with haematological malignancies in Lithuania: a national prospective cohort study. Lancet Haematol. 2021;8(8):e583-e592. doi:10.1016/S2352-3026(21)00169-1
- Dhakal B, Abedin S, Fenske T, et al. Response to SARS-CoV-2 vaccination in patients after hematopoietic cell transplantation and CAR T-cell therapy. Blood. 2021;138(14):1278-1281. doi:10.1182/blood.2021012769
- Salvini M, Maggi F, Damonte C, et al. Immunogenicity of anti-SARS-CoV-2 Comirnaty vaccine in patients with lymphomas and myeloma who underwent autologous stem cell transplantation. Bone Marrow Transplant. 2022;57(1):137-139. doi:10.1038/s41409-021-01487-4
- Greenberger LM, Saltzman LA, Senefeld JW, Johnson PW, DeGennaro LJ, Nichols GL. Antibody response to SARS-CoV-2 vaccines in patients with hematologic malignancies. Cancer Cell. 2021;39(8):1031-1033. doi:10.1016/j.ccell.2021.07.012
- Lopez Bernal J, Andrews N, Gower C, et al. Effectiveness of Covid-19 vaccines against the B.1.617.2 (Delta) variant. N Engl J Med. 2021;385(7):585-594. doi:10.1056/NEJMoa2108891
- Song Q, Bates B, Shao YR, et al. Risk and outcome of breakthrough COVID-19 infections in vaccinated patients with cancer: real-world evidence from the National COVID Cohort Collaborative. J Clin Oncol. 2022;40(13):1414-1427. doi:10.1200/JCO.21.02419
- Desai A, Gainor JF, Hegde A, et al; COVID19 and Cancer Clinical Trials Working Group. COVID-19 vaccine guidance for patients with cancer participating in oncology clinical trials. Nat Rev Clin Oncol. 2021;18(5):313-319. doi:10.1038/s41571-021-00487-z
- Bar-On YM, Goldberg Y, Mandel M, et al. Protection against Covid-19 by BNT162b2 booster across age groups. N Engl J Med. 2021;385(26):2421-2430. doi:10.1056/NEJMoa2115926
- Garcia-Beltran WF, St Denis KJ, Hoelzemer A, et al. mRNA-based COVID-19 vaccine boosters induce neutralizing immunity against SARS-CoV-2 Omicron variant. Cell. 2022;185(3):457-466.e4. doi:10.1016/j.cell.2021.12.033
- Shroff RT, Chalasani P, Wei R, et al. Immune responses to two and three doses of the BNT162b2 mRNA vaccine in adults with solid tumors. Nat Med. 2021;27(11):2002-2011. doi:10.1038/s41591-021-01542-z
- Saiag E, Grupper A, Avivi I, et al. The effect of a third-dose BNT162b2 vaccine on anti-SARS-CoV-2 antibody levels in immunosuppressed patients. Clin Microbiol Infect. 2022;28(5):735.e5-735.e8. doi:10.1016/j.cmi.2022.02.002
- Shapiro LC, Thakkar A, Campbell ST, et al. Efficacy of booster doses in augmenting waning immune responses to COVID-19 vaccine in patients with cancer. Cancer Cell. 2022;40(1):3-5. doi:10.1016/j.ccell.2021.11.006
- Zeng C, Evans JP, Chakravarthy K, et al. COVID-19 mRNA booster vaccines elicit strong protection against SARS-CoV-2 Omicron variant in patients with cancer. Cancer Cell. 2022;40(2):117-119. doi:10.1016/j.ccell.2021.12.014
- Coronavirus (COVID-19) update: FDA authorizes Moderna, Pfizer-BioNTech bivalent COVID-19 vaccines for use as a booster dose. News release. FDA; August 31, 2022. Accessed January 5, 2023. https://bit.ly/3BkZXre
- Atmar RL, Lyke KE, Deming ME, et al; DMID 21-0012 Study Group. Homologous and heterologous Covid-19 booster vaccinations. N Engl J Med. 2022;386(11):1046-1057. doi:10.1056/NEJMoa2116414
- Reimann P, Ulmer H, Mutschlechner B, et al. Efficacy and safety of heterologous booster vaccination with Ad26.COV2.S after BNT162b2 mRNA COVID-19 vaccine in haemato-oncological patients with no antibody response. Br J Haematol. 2022;196(3):577-584. doi:10.1111/bjh.17982
- Piechotta V, Mellinghoff SC, Hirsch C, et al. Effectiveness, immunogenicity, and safety of COVID-19 vaccines for individuals with hematological malignancies: a systematic review. Blood Cancer J. 2022;12(5):86. doi:10.1038/s41408-022-00684-8
- Sharif N, Alzahrani KJ, Ahmed SN, Dey SK. Efficacy, immunogenicity and safety of COVID-19 vaccines: a systematic review and meta-analysis. Front Immunol. 2021;12:714170. doi:10.3389/fimmu.2021.714170
- Kian W, Zemel M, Kestenbaum EH, et al. Safety of the BNT162b2 mRNA COVID-19 vaccine in oncologic patients undergoing numerous cancer treatment options: a retrospective single-center study. Medicine (Baltimore). 2022;101(2):e28561. doi:10.1097/MD.0000000000028561
- Shimabukuro TT, Cole M, Su JR. Reports of anaphylaxis after receipt of mRNA COVID-19 vaccines in the US - December 14, 2020-January 18, 2021. JAMA. 2021;325(11):1101-1102. doi:10.1001/jama.2021.1967
- Nasreen S, Calzavara A, Buchan SA, et al; Canadian Immunization Research Network (CIRN) Provincial Collaborative Network (PCN) Ontario investigators. Background incidence rates of adverse events of special interest related to COVID-19 vaccines in Ontario, Canada, 2015 to 2020, to inform COVID-19 vaccine safety surveillance. Vaccine. 2022;40(24):3305-3312. doi:10.1016/j.vaccine.2022.04.065
- Waissengrin B, Agbarya A, Safadi E, Padova H, Wolf I. Short-term safety of the BNT162b2 mRNA COVID-19 vaccine in patients with cancer treated with immune checkpoint inhibitors. Lancet Oncol. 2021;22(5):581-583. doi:10.1016/S1470-2045(21)00155-8
- Au L, Fendler A, Shepherd STC, et al; CAPTURE Consortium. Cytokine release syndrome in a patient with colorectal cancer after vaccination with BNT162b2. Nat Med. 2021;27(8):1362-1366. doi:10.1038/s41591-021-01387-6
- Aznab M, Chalehchaleh M, Dokoshkani S, Rezaei M. Evaluation of safety and side effects COVID-19 vaccine in cancer patients being treated. Asian Pac J Cancer Prev. 2022;23(4):1263-1270. doi:10.31557/APJCP.2022.23.4.1263
- Forster M, Wuerstlein R, Koenig A, et al. COVID-19 vaccination in patients with breast cancer and gynecological malignancies: a German perspective. Breast. 2021;60:214-222. doi:10.1016/j.breast.2021.10.012
- Shulman RM, Weinberg DS, Ross EA, et al. Adverse events reported by patients with cancer after administration of a 2-dose mRNA COVID-19 vaccine. J Natl Compr Canc Netw. 2022;20(2):160-166. doi:10.6004/jnccn.2021.7113
- Agrati C, Castilletti C, Sacchi A, et al. Immunogenicity and safety of BNT162b2 COVID-19 vaccine in a chronic lymphocytic leukaemia patient. J Cell Mol Med. 2021;25(13):6460-6462. doi:10.1111/jcmm.16565
- Benda M, Mutschlechner B, Ulmer H, et al. Serological SARS-CoV-2 antibody response, potential predictive markers and safety of BNT162b2 mRNA COVID-19 vaccine in haematological and oncological patients. Br J Haematol. 2021;195(4):523-531. doi:10.1111/bjh.17743
- Benjamini O, Rokach L, Itchaki G, et al. Safety and efficacy of the BNT162b mRNA COVID-19 vaccine in patients with chronic lymphocytic leukemia. Haematologica. 2022;107(3):625-634. doi:10.3324/haematol.2021.279196
- Greenberg RS, Ruddy JA, Boyarsky BJ, et al. Safety and antibody response to two-dose SARS-CoV-2 messenger RNA vaccination in patients with multiple myeloma. BMC Cancer. 2021;21(1):1354. doi:10.1186/s12885-021-09097-5
- Le Bourgeois A, Coste-Burel M, Guillaume T, et al. Safety and antibody response after 1 and 2 doses of BNT162b2 mRNA vaccine in recipients of allogeneic hematopoietic stem cell transplant. JAMA Netw Open. 2021;4(9):e2126344. doi:10.1001/jamanetworkopen.2021.26344
- Matkowska-Kocjan A, Owoc-Lempach J, Chruszcz J, et al. The COVID-19 mRNA BNT163b2 vaccine was well tolerated and highly immunogenic in young adults in long follow-up after haematopoietic stem cell transplantation. Vaccines (Basel). 2021;9(10):1209. doi:10.3390/vaccines9101209
- Bergman P, Blennow O, Hansson L, et al; COVAXID-collaborator group. Safety and efficacy of the mRNA BNT162b2 vaccine against SARS-CoV-2 in five groups of immunocompromised patients and healthy controls in a prospective open-label clinical trial. EBioMedicine. 2021;74:103705. doi:10.1016/j.ebiom.2021.103705
- Shem-Tov N, Yerushalmi R, Danylesko I, et al. Immunogenicity and safety of the BNT162b2 mRNA COVID-19 vaccine in haematopoietic stem cell transplantation recipients. Br J Haematol. 2022;196(4):884-891. doi:10.1111/bjh.17918
- Watanabe M, Yakushijin K, Funakoshi Y, et al. The safety and immunogenicity of the BNT162b2 mRNA COVID-19 vaccine in Japanese patients after allogeneic stem cell transplantation. Vaccines (Basel). 2022;10(2):158. doi:10.3390/vaccines10020158
- Ali H, Ngo D, Aribi A, et al. Safety and tolerability of SARS-CoV2 emergency-use authorized vaccines for allogeneic hematopoietic stem cell transplant recipients. Transplant Cell Ther. 2021;27(11):938.e1-938.e6. doi:10.1016/j.jtct.2021.07.008
- Ram R, Hagin D, Kikozashvilli N, et al. Safety and immunogenicity of the BNT162b2 mRNA COVID-19 vaccine in patients after allogeneic HCT or CD19-based CART therapy - a single-center prospective cohort study. Transplant Cell Ther. 2021;27(9):788-794. doi:10.1016/j.jtct.2021.06.024
- Pabst C, Benning L, Liebers N, et al. Humoral responses and chronic GVHD exacerbation after COVID-19 vaccination post allogeneic stem cell transplantation. Vaccines (Basel). 2022;10(2):330. doi:10.3390/vaccines10020330
- Sánchez van Kammen M, Aguiar de Sousa D, Poli S, et al; Cerebral Venous Sinus Thrombosis With Thrombocytopenia Syndrome Study Group. Characteristics and outcomes of patients with cerebral venous sinus thrombosis in SARS-CoV-2 vaccine-induced immune thrombotic thrombocytopenia. JAMA Neurol. 2021;78(11):1314-1323. doi:10.1001/jamaneurol.2021.3619
- Pavord S, Scully M, Hunt BJ, et al. Clinical features of vaccine-induced immune thrombocytopenia and thrombosis. N Engl J Med. 2021;385(18):1680-1689. doi:10.1056/NEJMoa2109908
- Li A, Kuderer NM, Hsu C-Y, et al; CCC19 consortium. The CoVID-TE risk assessment model for venous thromboembolism in hospitalized patients with cancer and COVID-19. J Thromb Haemost. 2021;19(10):2522-2532. doi:10.1111/jth.15463. Published correction appears in J Thromb Haemost. 2022;20(3):785-786.
- Brito-Dellan N, Tsoukalas N, Font C. Thrombosis, cancer, and COVID-19. Support Care Cancer. 2022;30(10):8491-8500. doi:10.1007/s00520-022-07098-z
- COVID-19 vaccines for people who are moderately or severely immunocompromised. CDC. Updated December 9, 2022. Accessed on December 14, 2022. https://bit.ly/3Wdzy6m
- COVID-19 resources: COVID-19 vaccination and cancer patients. National Comprehensive Cancer Network. Accessed on December 14, 2022. https://www.nccn.org/covid-19
- ASTCT resources for COVID-19. American Society for Transplantation and Cellular Therapy [ASTCT]. Updated 2022. Accessed on December 14, 2022. https://bit.ly/3Fo9gHN
- Use of COVID-19 vaccines in the United States: interim clinical considerations. CDC. Updated December 9, 2022. Accessed December 14, 2022. https://bit.ly/3Bsi5PZ
- Levin MJ, Ustianowski A, De Wit S, et al; PROVENT Study Group. Intramuscular AZD7442 (tixagevimab-cilgavimab) for prevention of Covid-19. N Engl J Med. 2022;386(23):2188-2200. doi:10.1056/NEJMoa2116620
- Case JB, Mackin S, Errico JM, et al. Resilience of S309 and AZD7442 monoclonal antibody treatments against infection by SARS-CoV-2 Omicron lineage strains. Nat Commun. 2022;13(1):3824. doi:10.1038/s41467-022-31615-7
- Kertes J, Shapiro Ben David S, Engel-Zohar N, et al. Association between AZD7442 (tixagevimab-cilgavimab) administration and severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection, hospitalization, and mortality. Clin Infect Dis. Published online July 29, 2022. doi:10.1093/cid/ciac625
- Nguyen Y, Flahault A, Chavarot N, et al; AP-HP-Centre Monoclonal Antibodies Working Group. Pre-exposure prophylaxis with tixagevimab and cilgavimab (Evusheld) for COVID-19 among 1112 severely immunocompromised patients. Clin Microbiol Infect. 2022;28(12):1654.e1-1654.e4. doi:10.1016/j.cmi.2022.07.015
- Mahase E. Covid-19: UK will not buy Evusheld owing to “insufficient data” on protection, government says. BMJ. 2022;378:o2021. doi:10.1136/bmj.o2021
- Qu P, Evans JP, Faraone J, et al. Distinct neutralizing antibody escape of SARS-CoV-2 omicron subvariants BQ.1, BQ.1.1, BA.4.6, BF.7 and BA.2.75.2. bioRxiv. Preprint posted online October 20, 2022.. doi:10.1101/2022.10.19.512891
- Dacon C, Tucker C, Peng L, et al. Broadly neutralizing antibodies target the coronavirus fusion peptide. Science. 2022;377(6607):728-735. doi:10.1126/science.abq3773
- Aaby P, Netea MG, Benn CS. Beneficial non-specific effects of live vaccines against COVID-19 and other unrelated infections. Lancet Infect Dis. Published online August 26, 2022. doi:10.1016/S1473-3099(22)00498-4
- Faustman DL, Lee A, Hostetter ER, et al. Multiple BCG vaccinations for the prevention of COVID-19 and other infectious diseases in type 1 diabetes. Cell Rep Med. 2022;3(9):100728. doi:10.1016/j.xcrm.2022.100728
- Immunization with IMM-101 vs observation for prevention of respiratory and severe COVID-19 related infections in cancer patients at increased risk of exposure (COV-IMMUNO). ClinicalTrials.gov. Updated September 13, 2022. Accessed on December 14, 2022. https://bit.ly/3YgO3Iz
Oncology Peer Review On-The-Go: COVID-19, Cancer, and the Potential of mRNA Vaccines
March 30th 2021Mehmet Sitki Copur, MD, discussed his article in the Journal ONCOLOGY® focusing on COVID-19, messenger RNA vaccines, and the excitement surrounding its integration into the future of cancer treatment.
