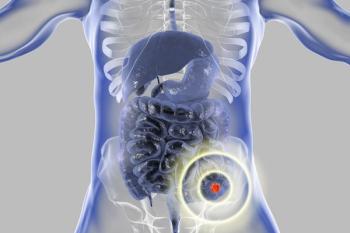
Molecular Testing in Metastatic CRC
Opening their discussion on metastatic colorectal cancer management, expert panelists reflect on the molecular testing paradigm in the setting of diagnosis and workup.
Episodes in this series

Transcript:
Cathy Eng, MD: Welcome to this Cancer Network® Patient Journey program titled "Diagnosis and Treatment of Metastatic Colorectal Cancer with a Focus on HER2-Positive Disease: Year in Review 2022". I am your host, Dr Cathy Eng, Professor of Medicine and Co-Leader and Co-Director of the GI [Gastrointestinal] Oncology Cancer Research program here at Vanderbilt-Ingram Cancer Center. I have a wonderful panel consisting of experts that have joined me today in this virtual discussion. I would like to invite my fellow panelists to introduce themselves. Dr Tanios Bekaii-Saab?
Tanios S. Bekaii-Saab, MD: Dr Eng, Cathy, thank you. Tanios Bekaii-Saab, Mayo Clinic, GI Medical Oncology.
Cathy Eng, MD: Dr Ciombor?
Kristen K. Ciombor, MD: Hi, I'm Kristen Ciombor. I'm also at the Vanderbilt-Ingram Cancer Center where I specialize in GI Medical Oncology.
Cathy Eng, MD: And Dr Hechtman?
Jaclyn F. Hechtman, MD: Hi, I'm Jackie Hechtman. I'm a GI Molecular Pathologist. I'm at Baptist Hospital, I'm the Precision Diagnostics Instructor at Miami Cancer Institute, and I also have a role at NeoGenomics.
Cathy Eng, MD: Thank you everyone for joining us today. We're going to discuss key updates that were presented at recent meetings regarding the testing and treatment of metastatic colorectal cancer. We will discuss these updates in the context of the treatment landscape and how they may impact clinical practice. Let's begin our discussion. Currently, regarding colorectal cancer it's remains a common malignancy as we all know and unfortunately, we're seeing an increase incidence in our young adult patient population on top of it all. Historically though, our patients are still the median age of 67 years of age. Most patients do not have an inherited form of colorectal carcinoma and most patients still are not being screened appropriately even though the screening age has now been reduced to the age of 45. We need to continue to highlight that patient population that needs to be screened sooner than the standard age previously at 50 years of age. And we know that for our metastatic colorectal cancer patient population unless they're surgically resectable. Unfortunately, the 5 year survival of these patients is approximately 14% and that has not changed dramatically over the past 20 years. I'd like to get the conversation started with Dr Hechtman and just focusing on how we can provide optimal care for our patients and really try to get your opinion about what do you view as molecular testing being appropriate for a metastatic colorectal cancer patients.
Jaclyn F. Hechtman, MD: It's a very limited number of markers that the NCCN [National Comprehensive Cancer Network] does recommend testing for. For all patients with colorectal carcinoma, it's recommended to do mismatch repair, expression testing by IHC [Immunohistochemistry screening] or a micro satellite testing by PCR and next-generation sequencing or both. For patients with distant metastases, either at diagnosis or at some time after diagnosis extended sequencing, so not just exon two, but 3, 4 of KRAS and NRAS as recommended, as well as BRAF V600E and then HER2 either by IHC reflex FISH or looking by NGS for copy variations as well as for patients with distant metastases NTRK 1 through 3 patient detection.
Cathy Eng, MD: Some of those molecular markers you mentioned are rare. How do we encourage our community providers as well as our patients to be aware of the actual – the current actionable mutations that exist that they can optimize their overall treatment? It took a long time as you know for BRAF to be a common approach for all of our newly-diagnosed patients in regards to testing. What can we do as providers and as well as your colleagues in molecular pathology, to help get the word out?
Jaclyn F. Hechtman, MD: There are some ways – it goes back to the methods we use. The methods we use are IHC, next-generation sequencing, FISH and CWGS sequencing. When we do it by next-generation sequencing, we pick up a lot of things, if we use a large panel MSI, TMB, all the mutation status, NTRK fusions. Sometimes there are barriers to that and we're not able to do NGS [Next generation sequencing] on every single case but that does provide a more comprehensive look and include that rare scale of actionable biomarkers that we're only going to see in a couple patients, but we pick it up, and we give them a long time of symptom-free life. So that's one way. Other ways are reflex testing so when a patient gets a diagnosis instead of waiting for the clinician to test, we're helping the patients not fall through the cracks by having a disease management team that say, this is what we're going to do. When we get this diagnosis, we run X, Y, and Z. Whether it's PD-L1, CPS, we send it through this panel. Other ways, there are molecular reference labs that have panels for a specific disease type so that can help, and they're supposed to be inclusive of different types of markers, so that's some ways we can get it out. When we can't do a large panel of next-generation sequencing tests, it's usually because of either low tumor content or in general not much tissue on the slide, we're not extracting enough DNA. Or the tumor purity isn't good enough so usually we need 20% tumor, if we don't have that, IHC is pretty much agnostic of tumor purity, so you can do MMRHC to qualify for MSI status. MMRHC generally performs well. You can screen for NTRAK fusions by pan-TRK IHC and for colon cancer the specificity of that is high, and you can do HER2 IHC also by that. And even if your tumor purity is let's say even if it's like 10%, by large panel NGS often KRAS and BRAF are hot spots. For the areas that do have that, you should be able to get a result for those.
Transcript edited for clarity.