Data from the ELEVATE trial may support elacestrant as an endocrine therapy backbone in ER-positive, HER2-negative metastatic breast cancer.

Data from the ELEVATE trial may support elacestrant as an endocrine therapy backbone in ER-positive, HER2-negative metastatic breast cancer.
“Higher pretreatment HER2 amplicon mRNA signature and HER2 protein expression predicted improved outcomes with T-DXd for [metastatic breast cancer],” Paolo Tarantino, MD, PhD, said.
Data from DESTINY-Breast09 may support trastuzumab deruxtecan plus pertuzumab as a frontline standard of care in HER2-positive advanced breast cancer.

Data from the phase 3 NATALEE trial confirms ribociclib plus NSAI consistently improves survival outcomes in stage II/III HR+/HER2– early breast cancer patients, regardless of age or menopausal status.

Data from the NeoSTAR trial showed no new safety signals with sacituzumab govitecan plus pembrolizumab for early-stage triple-negative breast cancer.

The use of chemotherapy trended toward improved recurrence-free intervals in older patients with high-risk tumors as determined via the MammaPrint assay.

Camizestrant and continued CDK4/6 inhibition delayed time to QOL deterioration vs SOC therapy in ER+/HER2– advanced breast cancer.

Patients who received ipatasertib/fulvestrant in the intention-to-treat population achieved a median PFS of 5.32 months compared with 1.94 months in the placebo arm.
In the phase 3 DESTINY-Breast06 trial, the overall biomarker-evaluable population’s confirmed ORR was 59.4% with T-DXd vs 33.9% with chemotherapy.
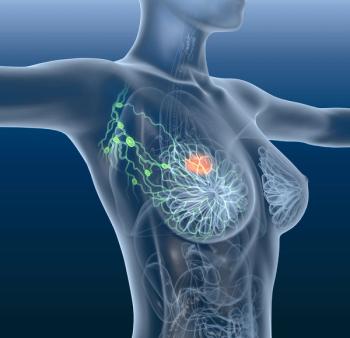
Across all 3 treatment arms, global health status/quality of life and functional domains were maintained in the phase 3 EMBER-3 trial.

Use of a pharmacist-directed resource appears to improve provider confidence and adverse effect monitoring for patients undergoing infusion therapy.

PFS was improved with first-line sacituzumab govitecan plus pembrolizumab for patients with PD-L1–positive metastatic TNBC.
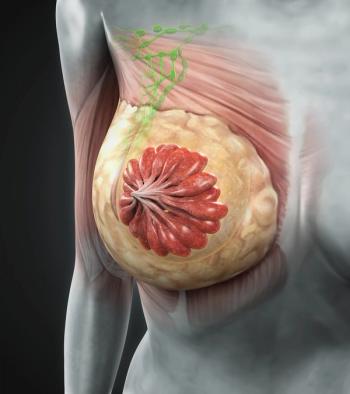
Vepdegestrant shows significant clinical activity and a favorable safety profile in ESR1-mutant HER2-negative, ER-positive metastatic breast cancer vs fulvestrant.

Reshma L. Mahtani, DO, describes how updates from the DESTINY-Breast09, ASCENT-04, and VERITAC-2 trials may shift practices in the breast cancer field.

Daniel G. Stover, MD, describes how findings from the phase 3 NATALEE trial may support expanding the portion of patients who receive CDK 4/6 inhibitors as a treatment for hormone receptor–positive, HER2-negative breast cancer.

Daniel G. Stover, MD, suggests that stromal tumor infiltrating lymphocytes may serve as a biomarker of immune activation and can potentially help optimize therapy with microtubule-targeting agents for patients with metastatic breast cancer.

Hope Rugo, MD, speaks to the importance of identifying patients with aromatase inhibitor–resistant, hormone receptor–positive, HER2-negative advanced breast cancer who are undergoing treatment with capivasertib/fulvestrant who may be at a high risk of developing diabetes or hyperglycemia.

The anti-tumor activity of lasofoxifene plus abemaciclib does not appear to be compromised by co-occurring alterations that confer resistance among patients with estrogen receptor–positive HER2-negative breast cancer.
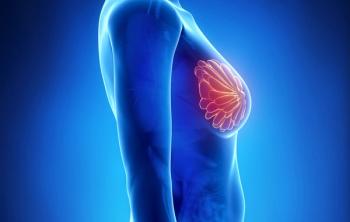
Additionally, treatment with sacituzumab govitecan-hziy may result in a prolonged overall response rate and clinical benefit rate vs treatment of physician’s choice in pretreated, endocrine-resistant, hormone receptor–positive, HER2-negative metastatic breast cancer.

Treatment with patritumab deruxtecan appears to yield improved responses in patients who have been heavily pretreated for metastatic breast cancer.

Sara M. Tolaney, MD, MPH, describes the benefit of sacituzumab govitecan for patients with HER2-low metastatic breast cancer seen in the final overall survival analysis of the phase 3 TROPiCS-02 study.
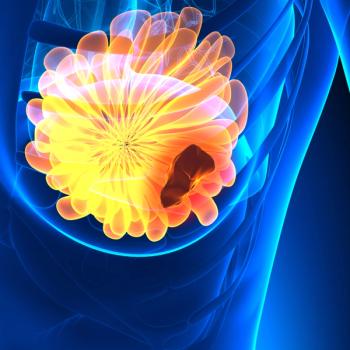
Zotaifin plus abemaciclib and fulvestrant appears to produce no dose-limiting toxicities among patients with estrogen receptor–positive metastatic breast cancer in a phase 1/2 study.

Elacestrant also appears to produce a manageable safety profile in the treatment of patients with estrogen receptor–positive HER2-negative advanced breast cancer in the phase 3 EMERALD trial.
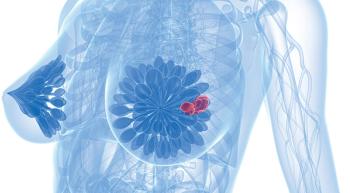
Older patients with hormone receptor–positive, HER2-negative, high-risk early breast cancer maintain a clinically meaningful absolute reduction in risk of distant relapse and invasive disease following treatment with abemaciclib and endocrine therapy.
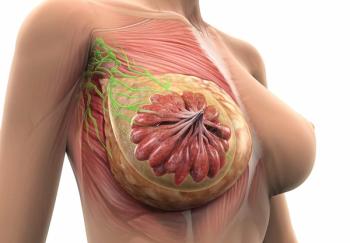
Results from the phase 3 NATALEE trial investigating ribociclib plus endocrine therapy may change practice for the treatment of hormone receptor–positive or HER2-negative early breast cancer, according to an expert from the University of Chicago Medicine.

Data from a phase 3 study indicate that weight loss intervention with a telephone-based program appears to be effective across all subgroups of breast cancer survivors.

According to Hurvitz, the findings of trials such as DESTINY-Breast04 and TROPiCS-02 shed light on potential new therapies for breast cancer, though more research is needed to address new agents and other unmet needs.

Patients with locally advanced or metastatic ESR1-mutant, estrogen receptor–positive, HER2-negative breast cancer who have progressed on a CDK4/6 inhibitor may benefit from treatment with lasofoxifene and abemaciclib.

Valentina Boni, MD, PhD, spoke about numerous trials in the breast cancer space presented at 2022 ASCO.

Mark Pegram, MD, spoke the most important data from the IDEAL trial he believes his colleagues should take away.