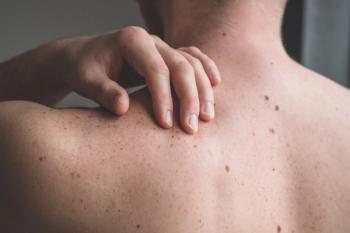
Nivolumab New Standard for Advanced, High-Risk Resected Melanoma
Nivolumab significantly improved recurrence-free survival compared with ipilimumab in patients with stage III/IV melanoma at high risk for recurrence, according to results of the CheckMate 238 study.
Nivolumab significantly improved recurrence-free survival compared with ipilimumab in patients with stage III/IV melanoma at high risk for recurrence, according to results of the CheckMate 238 study (
“The results clearly show that relapse-free survival is more favorable with nivolumab,” investigator Jeffrey Weber, MD, deputy director, Perlmutter Cancer Center, NYU Langone Health, said in a press release. “The majority of patients had higher risk disease than in most prior adjuvant melanoma trials, which makes the findings even more encouraging.”
The study included 906 patients aged 15 or older with complete resection of stage IIIb (34%), stage IIIc (47%), or stage IV (19%) melanoma. They were randomly assigned to nivolumab 3 mg/kg every 2 weeks or ipilimumab 10 mg/kg every 3 weeks for 4 doses, then every 12 weeks for up to 1 year.
The trial was stopped early after clear evidence of a benefit with nivolumab. At a follow-up of 18.5 months, treatment with nivolumab resulted in a 35% lower risk for recurrence compared with ipilimumab (hazard ratio, 0.65; 95% CI, 0.51–0.83). The 18-month recurrence-free survival was 66.4% compared with 52.7% for ipilimumab (P < .0001).
There were similar results across prespecified subgroups of patients including analyses of PD-L1 expression, which showed hazard ratios in favor of nivolumab.
“A previous trial found that ipilimumab had a significant relapse-free and overall survival advantage compared to placebo,” Weber said. “CheckMate 238 shows that nivolumab is superior to ipilimumab, so extrapolating these results, nivolumab is far better than no adjuvant treatment for high-risk melanoma. It is also much less toxic than ipilimumab.
Indeed, patients assigned to nivolumab had improved safety. Treatment-related grade 3/4 adverse events occurred in 14% of patients treated with nivolumab compared with 46% of patients assigned ipilimumab. Only 10% of patients assigned nivolumab stopped treatment due to adverse events compared with 43% of those assigned ipilimumab.
“The results of CheckMate 238 are very exciting,” said professor John Haanen, MD, PhD, of the Netherlands Cancer Institute in Amsterdam, commenting on the results of the study. “They show for the first time that an anti–PD-1 drug is superior in the adjuvant setting and because of its lower toxicity nivolumab is much easier to give than ipilimumab.”
The results of the study were
Newsletter
Stay up to date on recent advances in the multidisciplinary approach to cancer.