Study Shows Big Increase in Young Adult Melanoma Incidence Since 1970
Researchers at the Mayo Clinic in Rochester, Minnesota, found an eight-fold increase in melanoma incidence among young women between 1970 and 2009 in an epidemiological study. The increase was not as striking among young men, but there was still a four-fold jump in melanoma cases over those four decades.
Researchers at the Mayo Clinic in Rochester, Minnesota, found an eight-fold increase in melanoma incidence among young women between 1970 and 2009 in an epidemiological study. The increase was not as striking among young men, but there was still a four-fold jump in melanoma cases over those four decades.
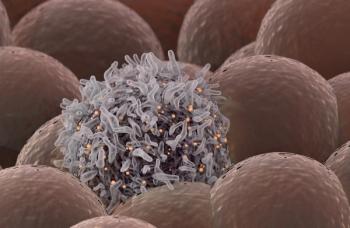
Human melanoma cell line growing in tissue culture
“Melanoma does not respect age,” said study author Jerry Brewer, MD. Brewer and colleagues used data from the Rochester Epidemiology Project, which began in 1966 and follows residents of Olmsted County, Minnesota. The study was
There were a total of 256 cases of melanoma identified in adults aged 18 to 39 years between 1970 and 2009; the average age at diagnosis was 29.9, and 179 of the patients (70%) were female.
The number of cases diagnosed increased in each decade of the study. Only 16 patients were diagnosed between 1970 and 1979 (6%); between 1980 and 1989 there were 44 cases (17%), between 1990 and 1999 there were 67 (26%), and 129 between 2000 and 2009 (50%).
These totals yielded increasing incidence rates: from 4.8 cases per 100,000 person-years in the 1970s up to 30.8 per 100,000 person-years in the last decade of the study. The difference was larger among women only, going from a rate of 5.4 cases per 100,000 person-years in the first decade to 43.5 per 100,000 person-years in the final decade of the study. The incidence of melanoma increased significantly by calendar year of diagnosis (P < .001) for both women and men.
In spite of the clearly increasing melanoma incidence, later stages of the disease became less likely over time, and the risk of death decreased. Each one-year increase in calendar year of diagnosis was significantly associated with a decreased risk of death due to metastatic melanoma, as well as with a decreased risk of death from any cause.
Brewer said in an e-mail that several factors come into play to explain the increase in melanoma, but that the most likely explanation among women is the increased use of tanning beds. “Of the million Americans going to tanning beds every day, over 70% are women [younger] than 30,” he said. “That in conjunction to a recent article that was able to show the chances of melanoma are 74% more likely in frequent tanning bed users makes this the most likely explanation in young women.”
In men, it may be as simple as trends toward wearing less clothing outdoors over the last few decades, Brewer said.
The study was limited largely by its population: the included participants were largely white, highly educated, and with good access to medical care. Populations elsewhere in the United States that do not have such good health care access may present with more advanced disease, among other differences.
“Our results emphasize the importance of active interventions to decrease risk factors associated with melanoma in young individuals,” the authors wrote, and Brewer added that there are good methods of prevention available to all. “Being aware of your skin, performing self skin exams at home monthly, avoiding tanning beds, and seeing a dermatologist could save your life,” he said.