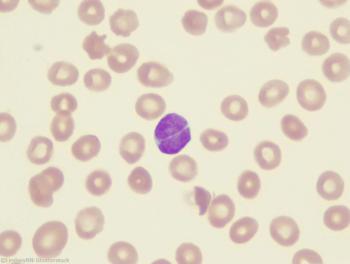
A study shows expanding access to care through insurance has the potential to improve outcomes in adults with follicular lymphoma.

A study shows expanding access to care through insurance has the potential to improve outcomes in adults with follicular lymphoma.
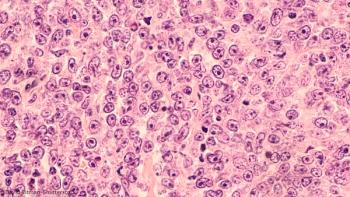
A study shows pretreatment ctDNA levels and molecular responses are independently prognostic of outcomes in lymphomas.

How much do you know about the clinical course and genomics of follicular lymphoma? Take our latest quiz to find out.
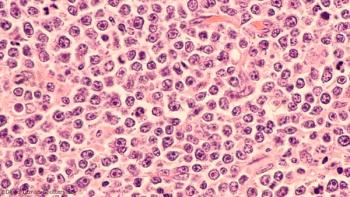
Antiretroviral therapy and rituximab show promise in aids-related diffuse large B-cell lymphoma patients.
Recent studies on CAR T-cell immunotherapy, and the recent approval of a new agent, add to evidence supporting the efficacy of these therapies.

Balancing the goal of obtaining a durable remission and that of avoiding a negative impact on quality of life argues against the routine use of chemotherapy in follicular lymphoma.

It is clear that chemoimmunotherapy has redefined the history of follicular lymphoma, producing survival rates measured in decades.

DLBCL and FL patients experience considerable economic burden during the first year after diagnosis.
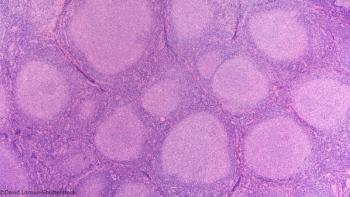
The combination of obinutuzumab and lenalidomide was found to be effective in relapsed or refractory follicular B-cell lymphoma.

New data support PFS as a surrogate endpoint for OS in future trials evaluating chemoimmunotherapy in DLBCL.
In the DBL3001 trial, the combination of ibrutinib and R-CHOP was not superior to treatment with R-CHOP alone.

In addition to significant improvements in 5-year OS and PFS with maintenance rituximab, there was a trend toward an association between maintenance and reduced transformation risk.
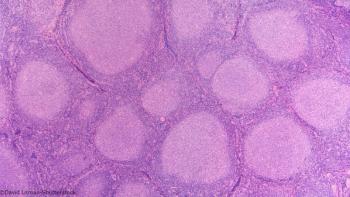
TROG 99.03 constitutes “the only high level evidence currently available to guide decision making for this group of patients,” says investigator Michael MacManus.

There may be prophylactic benefit from using lenalidomide, an orally bioavailable CNS-penetrating agent, combined with R-CHOP in the upfront setting.
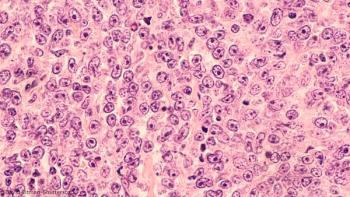
The OS benefit associated with standard treatment diminished in patients older than 80 with high comorbidity scores, but other age groups fared better.

De-escalated treatment may be possible in patients with advanced HL who reach a metabolic response after only 2 cycles of escalated BEACOPP.

Efficacy of lenalidomide plus rituximab was similar to chemotherapy induction in previously untreated symptomatic FL, with a better safety profile.

In the DAWN trial, however, investigators said, “some patients experienced prolonged remission durations and symptom relief with no new safety signals.”

AEs were more common in patients assigned to obinutuzumab compared with rituximab; however, baseline characteristics differed between treatment arms.
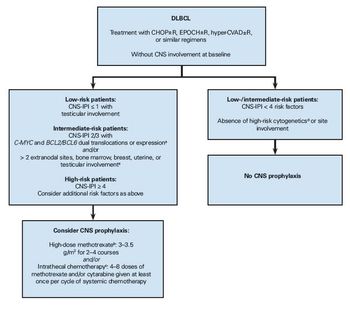
Here we review current prognostic models, risk factors, and prophylaxis methods to provide a practical approach to preventing CNS relapse in patients with DLBCL.

Polatuzumab vedotin administered with bendamustine and rituximab significantly improved PET-based CR rates, PFS, and OS in DLBCL but not FL.

In TRANSCEND NHL 001, the CD19-directed 4-1BB CAR T-cell product lisocabtagene maraleucel yielded durable responses in heavily pretreated R/R DLBCL.

While HCT is an important benefit for FL patients, the optimal approach remains up for debate.

The approval includes adults with R/R DLBCL after two or more lines of prior systemic therapy, high-grade B-cell lymphoma, and DLBCL arising from FL.

“The core message is that DLBCL can no longer be viewed as a single disease,” explained senior author Dr. Louis M. Staudt, Director of NCI’s Center for Cancer Genomics.