The safety profile of amivantamab was consistent with previous reports in this HNSCC population, with no new signals reported.

The safety profile of amivantamab was consistent with previous reports in this HNSCC population, with no new signals reported.

Further research will investigate rates of adverse effects among patients treated with liso-cel in the real world vs a clinical trial setting.

The differences in treatment setting are associational and are likely influenced by confounding by indication and not treatment effects.

A 5-year OS rate of 97.1% was observed among patients who received PSMA PET/CT restaging at first biochemical recurrence following prostatectomy.

Confirmed antilymphoma responses occurred in 75% of patients with lymphoma, including 2 with a complete response and 2 with a partial response.

CAR T-cell therapies displayed strong efficacy and manageable safety across lymphoma populations at the 2026 Tandem Meetings.

Based on the prevalence of GLP-1 agonists employed in standard medical practice, Li’s team will assess their impact on radiotherapy for prostate cancer.

No serious adverse effects were observed with TRX103 in patients with hematologic malignancies undergoing HLA-mismatched HCT.

Of 78 patients with NMIBC in the phase 2 clinical trial, 64.4% experienced a complete response with TLD-1433.

No differences in complication rate were observed between the MIXREAL and control groups among those treated for kidney cancer in the REALITATEM trial.

CancerNetwork spoke with Arturo Loaiza-Bonilla, MD, MSEd, FACP, regarding his insights about recent advancements for AI in oncology.

Real-world data presented at the 36th Annual IPCU build upon findings from the phase 3 TITAN trial evaluating apalutamide in this CSPC population.

The median progression-free survival was significantly higher with donor vs placebo fecal microbiota transplantation in this RCC population.

PSMA-PET could be considered in selective cases, given its modest sensitivity and prognostic value in intermediate-risk prostate cancers.

Any-grade treatment-emergent immune-mediated AEs occurred in 22% of patients with early-stage lymphoma treated with the ADC-based regimen.

Findings from the phase 1b/2 TENACITY-01 trial, which is assessing CTD402 monotherapy in these hematologic malignancies, supported the agency’s decision.
Findings from the phase 1/2 BRUIN trial support the Notice of Compliance with conditions for pirtobrutinib in this relapsed/refractory disease population.
A correlation between miR-93-5p and basal-like tumor features was observed among urinary samples of patients with bladder cancer.

Data from the phase 2/3 AHEAD-MERIT trial support the FDA decision for this head and neck cancer population.

The requested information does not pertain to the design or initiation of any new trials, and the developers plan to provide it in the next 30 days.
Toxicities with streptozotocin/5-fluorouracil and everolimus were comparable with other orally available chemotherapeutic schemes in this NET population.

Epcoritamab did not demonstrate a significant improvement in OS, but improvements were observed in PFS, ORR, and DOR in this DLBCL group.

According to investigators, the lack of anti-tumor activity and immunogenicity results do not support the agent’s further development in metastatic CRPC.

A disease control rate of 100% was attained among 4 patients with Waldenström lymphoma treated with the CAR-NK cell therapy.
Federal cuts to insurance and cancer research could reduce access to therapies and stifle progress when incidence is rising across many common cancers.
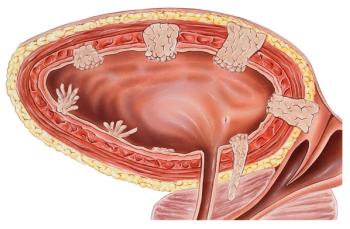
Data from the QUILT-3.032 trial supported the Saudi approval of nogapendekin alfa plus BCG in adults with BCG-unresponsive NMIBC with carcinoma in situ.
Patients with BPDCN who did not achieve a complete or clinical complete response during treatment experienced a restoration of hematopoiesis.

No grade 3 or greater treatment-related adverse effects or long-term safety signals emerged with gemogenovatucel-T in this ovarian cancer group.
Any-grade AEs were comparable between cadonilimab and a PD-1 monoclonal antibody regimen in this population, and no difference in grade 3/4 AEs emerged.

Ash Tewari, MBBS, hopes that with institutional partner aid, in 10 years, 1 million men will undergo prostate cancer screening through mobile units.