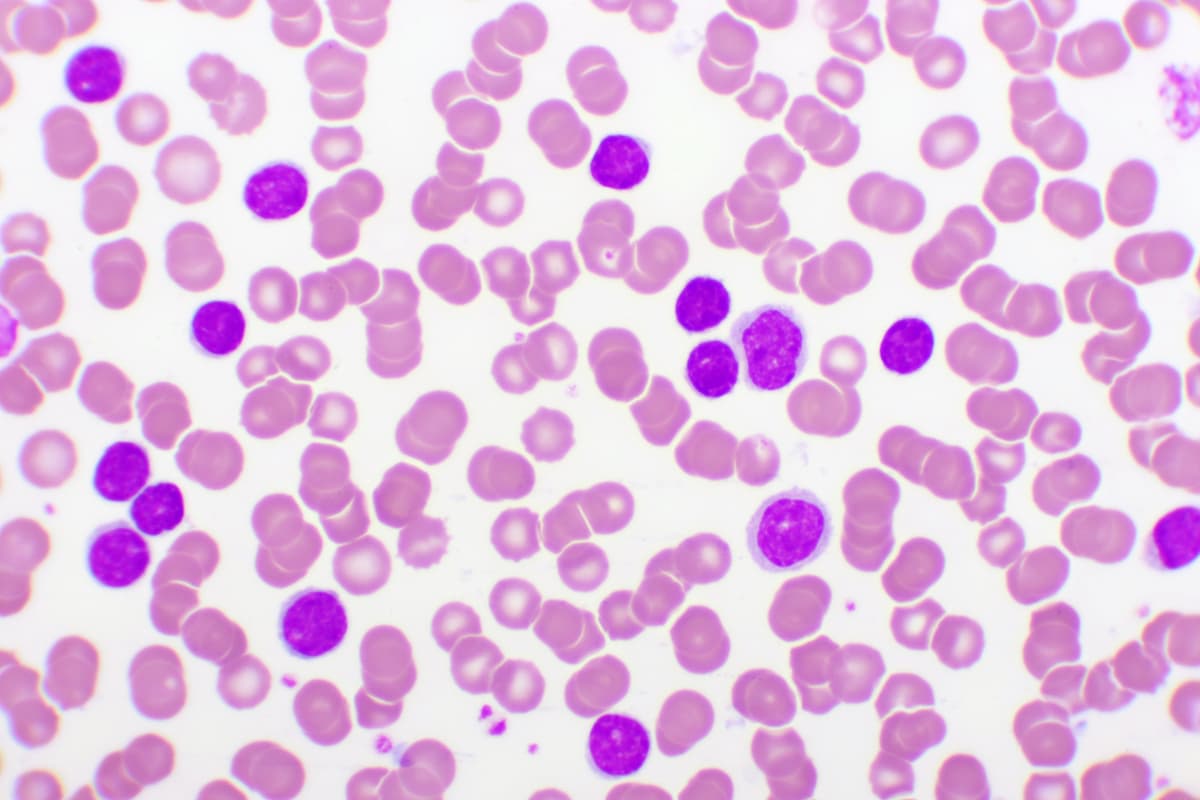
Leukemia
Latest News
Latest Videos

CME Content
More News
Among patients with Philadelphia chromosome–positive acute lymphoblastic leukemia, ponatinib plus chemotherapy yielded higher rates of minimal residual disease–negative complete remission compared with imatinib.

Two teams from leading institutions go head-to-head to debate the latest datasets and advances in chronic myeloid leukemia (CML).

Findings from a secondary analysis highlighted an association between improved quality of life outcomes and longitudinal use of approach-oriented coping strategies in patients with acute myeloid leukemia.

A conditioning regimen consisting of of Iomab-B prior to a bone marrow transplant met the phase 3 SIERRA trial’s primary end point of durable complete remission compared with conventional care in elderly patients with relapsed or refractory acute myeloid leukemia.
Quizartinib has received priority review from the FDA for the treatment of patients with newly diagnosed acute myeloid leukemia that is FLT3-ITD positive.
Michael Mauro, MD, presents data on a phase 2 ponatinib dose-ranging study in chronic-phase CML.

Steven Frommeyer introduces the two teams of competing physicians participating in Cancer Network® Face-off.
A panel of experts convened at the 2022 NCCN: Hematologic Malignancies Conference to discuss the classification, treatment options, and supportive care strategies available for patients with acute myeloid leukemia.

Topline results from the phase 3 ALPINE trial’s final progression-free survival analysis highlighted that zanubrutinib yielded higher progression-free survival compared with ibrutinib in patients with chronic lymphocytic leukemia.

Findings from a study examining the prognostic value of Nutritional Risk Index prior to hematopoietic stem cell transplant in patients with acute myeloid leukemia highlighted a need to consider other tools for assessing nutritional status among those undergoing transplant.

A real-world study found that time to discontinuation and time to next treatment outcomes associated with ibrutinib were not impacted by a baseline high risk of atrial fibrillation or stroke in patients with chronic lymphocytic leukemia or small cell lymphocytic lymphoma.

An 8-to-4 vote was cast by the FDA’s Oncologic Drugs Advisory Committee against the use of duvelisib in previously treated chronic lymphocytic leukemia and small lymphocytic leukemia.
Frequent targetable mutations in patients with extramedullary acute myeloid leukemia lends credence to the use of next-generation sequencing to determine the optimal targeted therapy approach.
In patients with acute myeloid leukemia receiving venetoclax, tumor lysis syndrome was uncommon; patients at high risk should be admitted for venetoclax dosing ramp-up.
Results from the phase 3 ASCEMBL trial led to the approval of asciminib by the European Commission for patients with Philadelphia chromosome–positive chronic myeloid leukemia in chronic phase.

The FDA has placed a full clinical hold on a phase 1 trial assessing FHD-286 as a potential treatment for patients with relapsed/refractory acute myelogenous leukemia and myelodysplastic syndrome due to concerns around suspected cases of fatal differentiation syndrome that may be associated with the agent.

Michael R. Bishop, MD, and Bruce B. Bank, MD, review results from the ELEVATE-RR noninferiority trial on acalabrutinib versus ibrutinib in CLL, and discuss the clinical implications of the findings.

Adult patients with acute myeloid leukemia who are not eligible for treatment with standard induction chemotherapy may benefit from treatment with decitabine and cedazuridine, the marketing authorization application for which was accepted by the European Medicines Agency.

Patients with newly diagnosed acute myeloid leukemia had longer overall survival with a modified dosing schedule of venetoclax plus a hypomethylating agent.
Although European Leukemia Net 2017 Risk Stratification was ineffective for predicting outcomes following allogeneic hematopoietic stem cell transplantation in intermediate-risk acute myeloid leukemia, pre-transplant Wilms tumor gene 1 expression and FLT3-ITD mutation demonstrated promising predictive ability.

WU-CART-007 was granted fast track and rare pediatric disease designation by the FDA for the treatment of patients with relapsed/refractory T-cell acute lymphoblastic leukemia and lymphoblastic lymphoma.
The regulatory organization indicated that duvelisib induces increased risk of death or serious adverse effects in patients with chronic lymphocytic leukemia and small lymphocytic leukemia.

Black adolescent young adult patients with acute myeloid leukemia appeared to have inferior outcomes compared with White patients.

In a new series from CancerNetwork®, 2 teams of fellows from leading institutions go head-to-head to debate the latest datasets and advances in acute lymphoblastic leukemia.
Patients with previously untreated chronic lymphocytic leukemia experienced minimal residual disease negativity following treatment with venetoclax and ibrutinib.