In a recent study, researchers found that certain amino acids in the blood were associated with a twofold increased risk of a pancreatic cancer diagnosis.

In a recent study, researchers found that certain amino acids in the blood were associated with a twofold increased risk of a pancreatic cancer diagnosis.
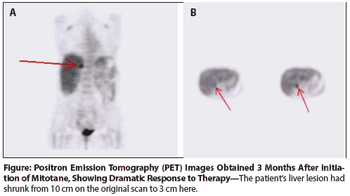
Adrenocortical carcinoma is a rare disease, with an annual incidence rate ranging from 0.5 to 2.0 cases per million individuals.

A new study provides evidence that a daily aspirin may reduce the risk of developing pancreatic cancer.
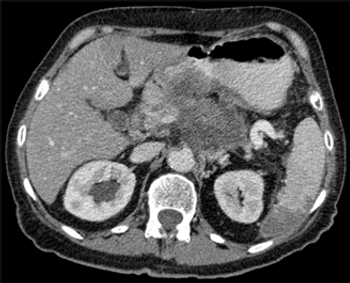
The JAK inhibitor ruxolitinib may improve overall survival in patients with metastatic pancreatic cancer characterized by an elevated CRP, a well-established marker of inflammation.
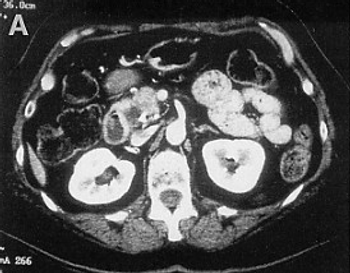
A blood-based test of four biomarkers including CA 19-9 may help clinicians diagnose pancreatic cancer at an earlier stage.
A phase III trial found that MM-398 in combination with other drugs increases overall survival in pre-treated patients with metastatic pancreatic cancer.

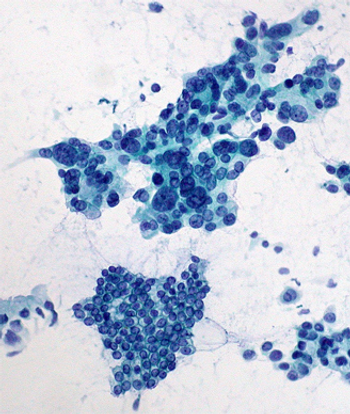
Proteomic cyst fluid mucin profiling may serve as an accurate diagnostic tool for the identification of pancreatic cancer precursor lesions, according to the results of a recently published study.

Using two new diagnostic panels based on microRNA in whole blood, researchers were able to distinguish patients with pancreatic cancer from healthy control patients.

In this interview, we discuss the current state of pancreatic cancer management, and look toward trials to further define the best course of treatment for this deadly disease.
The combination of two anticancer vaccines demonstrated improved survival compared to a single vaccine in patients with advanced pancreatic cancer, a particularly difficult to treat tumor type with few therapy options.
Completion of 6 cycles of adjuvant chemotherapy, rather than time of initiation, was an independent prognostic factor after resection of pancreatic adenocarcinoma, according to results taken from the phase III European Study Group for Pancreatic Cancer-3.

After 2 decades of disappointing phase III trials and years of single-agent gemcitabine therapy, the pancreatic cancer community is relieved to expand the front-line armamentarium in patients with mPAC. Here we evaluate the current landscape and ask some provocative questions about response rate, dosing, and predictive markers.

All improvements in outcomes for patients with metastatic pancreatic adenocarcinoma have occurred with the use of cytotoxic agents, which will probably remain the mainstay of treatment for advanced pancreatic adenocarcinoma.

Gemcitabine monotherapy has been the standard of care for patients with metastatic pancreatic cancer for several decades. Despite recent advances in various chemotherapeutic regimens and in the development of targeted therapies, metastatic pancreatic cancer remains highly resistant to chemotherapy.

In light of two recent positive clinical trials for advanced pancreatic cancer, we are currently facing an interesting situation that those of us who treat this disease have not had to deal with previously: what to do with this expanding array of choices?

Researchers have identified a potential new method for treating pancreatic cancer, using calcium to overload pancreatic cancer cells and, thus, induce cell death in cancerous cells while sparing healthy cells.

Trends in pancreatic mortality have gone in opposite directions for blacks and whites during the last few decades, a pattern which cannot be explained by known risk factors, according to researchers from the American Cancer Society.
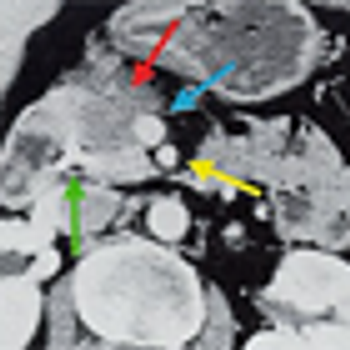
Researchers at Kaiser Permanente were able to achieve complete histopathologic response in more than 40% of initially unresectable patients with pancreatic adenocarcinoma who underwent prolonged preoperative chemotherapy and were subsequently able to undergo surgical resection.

Patients with a high body mass index prior to being diagnosed with pancreatic cancer had reduced survival from the disease and were more likely to present with late-stage cancer, according to the results of a recently published study.
The combination of two chemotherapy agents-nab-paclitaxel and gemcitabine-improves survival for patients with metastatic pancreatic cancer, according to the results of a phase III trial.
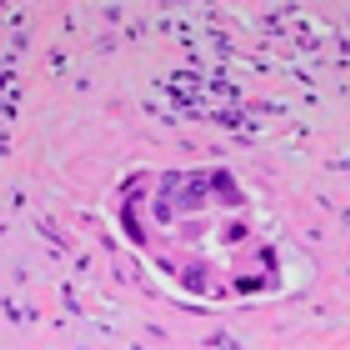
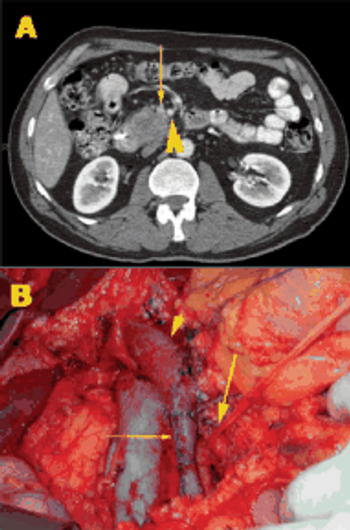
The patient is an otherwise healthy 45-year-old female who presented to her primary care physician with 6 weeks of increasing left upper quadrant abdominal pain with radiation to the back. She underwent an abdominal ultrasound, which revealed a large cystic abdominal mass.
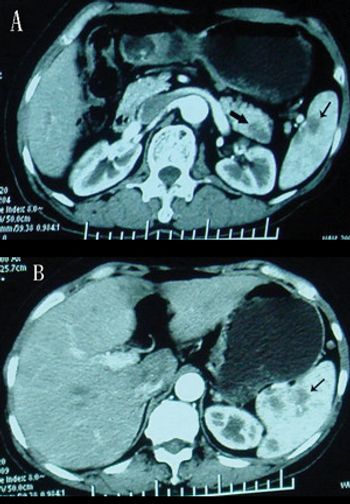
Using blood samples of pancreatic cancer and chronic pancreatitis patients, researchers in Japan have developed a metabolomics-based test that may be an easy and noninvasive way to detect pancreatic cancer.

Advanced urothelial cancer remains, along with pancreatic cancer, one of the last solid tumors for which essentially no progress has been made for 25 years. It’s time to think out of the box, and to develop novel and creative ways of overcoming the real, but not insurmountable, logistical challenges to carrying out the needed clinical trials.

This review covers symptoms and complications in patients with late-stage pancreatic cancer, including venous thromboembolism, anorexia-cachexia, pain, and depression.

Optimal supportive care for patients with pancreatic cancer is essential. Putting these interventions into practice requires that oncologists and oncology teams incorporate innovations at both the individual and the system level.