Leukemia
Latest News

FDA Approves Abbreviated NDA for Dasatinib Tablets in Leukemia Indications
Latest Videos

CME Content
More News

Over the past 4 years, the FDA has accepted a number of NDA submissions for dasatinib, but it has yet to receive approval in CML/ALL.

Results from the phase 1/2 AUGMENT-101 trial support the FDA’s decision for approving revumenib in this NPM1-mutated, relapsed/refractory AML population.
The FDA has set a Prescription Drug User Fee Act date of June 18, 2026, for approving this formulation of nilotinib in chronic myeloid leukemia.

Based on the Good Manufacturing Practice observations, the FDA has given a complete response letter for dasatinib for patients with CML/ALL.

Yale’s COPPER Center aims to address disparities and out-of-pocket costs for patients, thereby improving the delivery of complex cancer treatment.

Jorge Cortes, MD, outlines the impact of imatinib in chronic myeloid leukemia and highlights future initiatives in the field.

Non-Hodgkin lymphoma and other indolent forms of disease may require sequencing new treatments for years or decades, said Scott Huntington, MD, MPH, MSc.

Fixed-duration therapy may be more suitable for younger patients, while continuous therapy may benefit those who are older with more comorbidities.

Determining the molecular characteristics of one’s disease may influence the therapy employed in the first line as well as subsequent settings.
A phase 1 trial is evaluating UB-VV111 with and without rapamycin as treatment for patients with CLL and LBCL who received at least 2 prior therapies.
An indirect comparison supports continuous therapy with zanubrutinib as a valuable treatment option in treatment-naïve CLL or SLL.

Data from KOMET-001 support ziftomenib as a new potential option for patients with relapsed/refractory NPM1-mutated acute myeloid leukemia.

A 2-way communication between providers and patients may help facilitate dose modifications to help better manage adverse effects.

Treatment with AML depends on a variety of factors, including stage of treatment, transplant eligibility, and mutational status.

Several ongoing trials are evaluating the efficacy of ziftomenib treatment combinations in this acute myeloid leukemia population.

Single-agent ziftomenib achieved an ORR of 35% in patients with relapsed/refractory acute myeloid leukemia harboring an NPM1 mutation.

New targeted therapies are needed to improve outcomes for patients with NPM1-mutant relapsed/refractory acute myeloid leukemia.

Ziftomenib yielded a median overall survival of 16.4 months in responders with NPM1-mutant AML who received ziftomenib in the phase 1b/2 KOMET-001 trial.
Results from the phase 3 BRUIN CLL-313 trial show that OS trended favorably for pirtobrutinib vs chemoimmunotherapy in this CLL and SLL population.

Jorge Cortes, MD, believes that, despite the rapid improvements made in CML treatment, there is always more to be done to help patients.

Both experimental models significantly improved upon historical clinical risk trial groups for patients with acute myeloid leukemia.
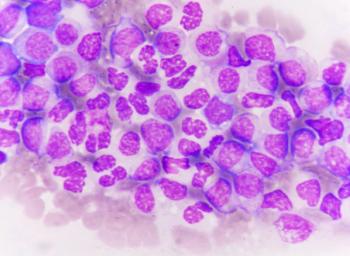
No minimal residual disease-negativity was observed with tuspetinib in patients with AML, including in a patient with more than 7 months of follow-up data.
Leading experts gathered in Orlando, Florida, to discuss the current and future state of cellular therapy in oncology at the 2025 ICE-T Symposium.

Researchers have identified the transcription factor CEBPA as a crucial regulator of immune recognition in acute myeloid leukemia.
Data from the phase 3 BRUIN CLL-314 trial show a progression-free survival trend favoring pirtobrutinib compared with ibrutinib in patients with CLL/SLL.





![We have the current CAR [T-cell therapies], which target CD19; however, we need others.](https://cdn.sanity.io/images/0vv8moc6/cancernetwork/6d5ddb2c2098f525a65b378ece6ca55a114f95fc-2974x1660.png?w=320&fit=crop&auto=format)