A new epigenetic hallmark of melanoma has been identified, which has a critical function in disease development, and may serve as a potential target for reversing melanoma progression.

Your AI-Trained Oncology Knowledge Connection!



A new epigenetic hallmark of melanoma has been identified, which has a critical function in disease development, and may serve as a potential target for reversing melanoma progression.
The oral selective MEK inhibitor trametinib improved progression-free and overall survival over chemotherapy in patients with metastatic melanoma with a BRAF mutation, according to a new phase III trial.

Sentinel lymph node biopsy is recommended for patients with newly diagnosed intermediate-thickness melanomas, while the procedure may not be indicated for patients with thinner lesions, according to a new set of guidelines.

A new target of melanoma tumors has been identified that may be promising as part of a novel combination therapy for melanoma. In a study published in Nature Medicine, researchers have identified that more than half of melanoma cases, both early and late-stage, may have higher levels of MDM4, a p53-interacting protein.
A new study finds cutaneous human papillomavirus infection can increase the risk of squamous-cell carcinoma, a nonmelanoma skin cancer.
In a phase III trial, the oral BRAF inhibitor dabrafenib, improved progression-free survival in previously untreated metastatic melanoma patients.

At the ASCO annual meeting, researchers presented persuasive evidence that a new class of targeted agents-MEK inhibitors-may warrant inclusion in the growing armamentarium for patients with advanced BRAF-mutated melanoma.

In this exclusive interview, Michael B. Atkins, MD, director of the Georgetown Lombardi Comprehensive Cancer Center, discusses some of the most important melanoma research to come out of this year’s ASCO meeting and talks about the future of melanoma therapies.
Data from the phase III BREAK-3 and the phase II BREAK-MB trials of dabrafenib establish the drug as the second BRAF inhibitor for BRAF V600E-mutated melanoma.

The class of agents that target the Programmed Death 1 (PD-1) pathway was described at ASCO as “likely the most exciting new agents recently developed in melanoma.”

The new therapies that became available for advanced melanoma over the past year-the anti-CTLA4 antibody ipilimumab (Yervoy) and the selective BRAF inhibitor vemurafenib (Zelboraf)-represent promising new options for these patients, whose prognosis was heretofore almost universally dismal. However, the advent of new treatment strategies has made treatment decisions more complex.

Researchers have shown that patients who use nonsteroidal anti-inflammatory drugs like aspirin and ibuprofen are less likely to develop three types of skin cancer.

A new analysis of four large European trials of cutaneous melanoma patients showed a substantial survival advantage for women, most likely explained by underlying biologic differences.
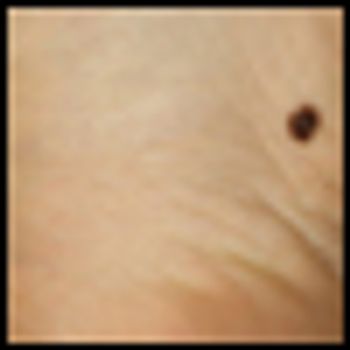
The addition of sorafenib to isolated limb infusion therapy with melphalan did not improve responses in a new phase I trial of patients with in-transit extremity melanoma.
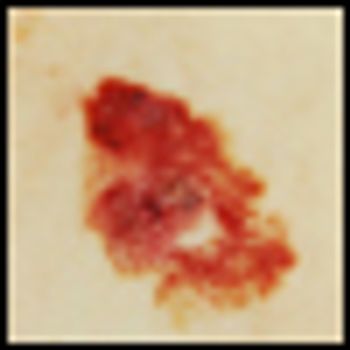
Melanoma has become the poster cancer for genomic research. The identification of a driver mutation in the BRAF gene found in approximately 40% of metastatic melanoma patients and the subsequent approval last year of the targeted BRAF inhibitor, vemurafenib, has resulted in a surge of both clinical and laboratory research.
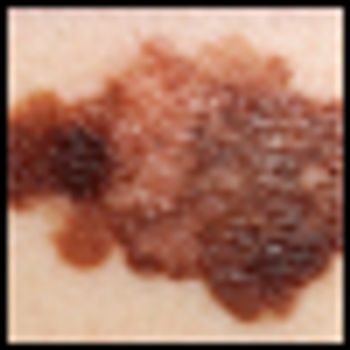
The presence of a mutation in the MEK1 gene in melanoma patients does not cause resistance to BRAF inhibitor therapy in patients that also carry a BRAF mutation, according to a new study. Previously, experts believed that resistance to the drugs in BRAF-mutated melanoma patients could likely be blamed on the concurrent mutation in MEK1.
Researchers at the Mayo Clinic in Rochester, Minnesota, found an eight-fold increase in melanoma incidence among young women between 1970 and 2009 in an epidemiological study. The increase was not as striking among young men, but there was still a four-fold jump in melanoma cases over those four decades.
Results from a phase II trial of vemurafenib for metastatic melanoma show a significant number of patients exhibiting a prolonged and durable response and a median overall survival of 16 months.
A study published last month shows that the melanoma drug ipilimumab has activity in melanoma patients whose cancer has spread to the brain. Long-term survival of melanoma patients with brain metastases was comparable to survival of metastatic melanoma patients without brain metastases.

A study published this week shows that taking retinol, a form of vitamin A, results in a decrease in the risk of developing melanoma. The effect is limited to those who took vitamin A in excess of standard multivitamin guidelines and was more pronounced in women than in men.

The US Food and Drug Administration (FDA) announced the approval of vismodegib (Erivedge), for the treatment of advanced basal cell carcinoma, the most common type of skin cancer, for patients who are not eligible for surgery or radiation, and for metastatic disease.

Metastatic melanomas that harbor the V600E mutation in the BRAF gene respond rapidly to vemurafenib (Zelboraf), the BRAF V600E inhibitor. But While vemurafenib results in a response in about 80% of melanoma patients, the clinical response among CRC patients is not greater than 5%.
In a rare case where the side effect of a cancer treatment can be explained through molecular studies, researchers have identified the reason behind the frequent skin lesion side effect among metastatic melanoma patients that take the newly approved drug vemurafenib.

A large cohort study shows that women on antiestrogen therapy have a lower risk of melanoma. In a study of 7360 women diagnosed with breast cancer between 1980 and 2005, 54% were given supplemental antiestrogen therapy. The rate of cutaneous melanoma was 60% higher for those women not taking antiestrogen supplements compared with the expected rate of melanoma incidence based on age and other factors.

The management of in-transit metastases is challenging, since the treatments and extent of disease vary greatly based on the number, depth, location, and distribution of lesions, and on their biological behavior.