
ONCOLOGY Vol 34 Issue 8

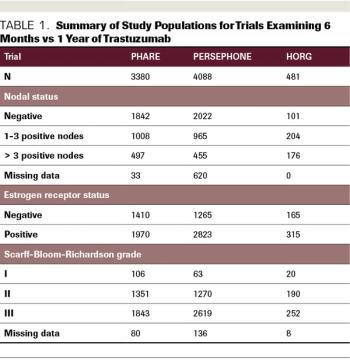
ABSTRACT Prior to the introduction of trastuzumab, the first targeted anti-HER2 agent, in 1998, patients diagnosed with HER2-positive breast cancer felt like they were being handed a death sentence. Despite treatment with aggressive chemotherapy, their tumors recurred faster, more often spread to brain and liver, and were associated with higher rates of death than HER2-negative tumors. However, in the 1980s, cancer researchers and oncologists recognized that HER2 could be targeted by a small molecule that binds to the receptor on the cell surface and blocks the signal telling the cell to divide. This small molecule was called trastuzumab, and it eventually completely changed how HER2-positive breast cancer was treated. The drug was first approved in the metastatic setting, and then the results of 2 pivotal randomized control trials demonstrated that the administration of trastuzumab in the adjuvant setting decreased the risk of breast cancer recurrence by 50%. These trials showed trastuzumab to be unequivocally effective in the adjuvant setting and the HERA trial results led to the adoption of 1 year of adjuvant trastuzumab as the standard of care. Since that time, the field of anti–HER2-targeted therapy has exploded, with the development of multiple targeted agents for use in the advanced and up-front settings. Although trastuzumab significantly improves outcomes for women diagnosed with HER2-positive breast cancer and has few adverse effects (AEs), the disadvantages are that it requires intravenous administration every 3 weeks and can be associated with cardiac AEs. It is also expensive. Given all of these factors, the question of whether a duration of trastuzumab that is shorter than 1 year may be acceptable for some patients with early-stage HER2-positive breast cancer is an important and very relevant one. Here, we will review the studies that have examined this question and evaluate their results.


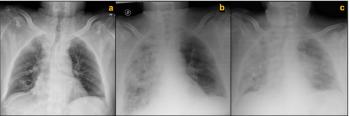
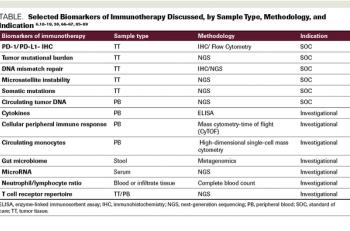
ABSTRACT Advances in immuno-oncology over the last several years have led to FDA approvals of novel agents. As our understanding of immune response and its checkpoints has evolved, further advances have been made in treatment for several cancer types. To predict a response to immunotherapy, the initial biomarkers used were expression of the PD-1 receptor and PD-L1, as assessed by immunohistochemistry. More recently, predictive biomarkers have included microsatellite instability, DNA mismatch repair, and tumor mutational burden. Although these markers may be clinically relevant in predicting an immunotherapy response, cancer immunotherapy fails some patients. Improved understanding of the human immune system is necessary, as is a careful evaluation of the methods used to predict and assess response to Immuno-oncology treatments. With the application of therapeutic immune-modulating agents, more comprehensive assays, and associated bioinformatics tools to accurately assess the tumor microenvironment, we may better predict responses to immuno-oncology agents and the ever-increasing complexity of their clinical use.
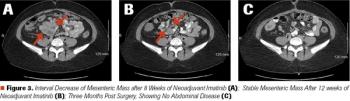
ABSTRACT Gastrointestinal stromal tumors (GISTs) are rare neoplasms of the gastrointestinal tract. They commonly present with nonspecific symptoms and thus are often discovered incidentally. They are best identified by CT scan and most stain positive for CD117 (C-Kit), CD34, and/or DOG-1. Several risk stratification classification systems have been developed based on tumor size, mitotic rate, location, and perforation. Traditional chemotherapy and radiation therapy have been very ineffective, making surgery the mainstay of treatment. The discovery of mutations associated with these tumors has revolutionized the treatment approach. Imatinib mesylate, a selective tyrosine kinase receptor inhibitor, used as adjuvant or neoadjuvant therapy, has greatly improved the morbidity and mortality associated with GISTs. As the survival of patients has increased with the long-term use of targeted therapies, quality-of-life issues now have become much more relevant and have come to the forefront of care. We present a young woman who was successfully treated for GIST but now faces associated long-term adverse effects of imatinib, including the challenge of preserving fertility and the potential for childbearing.
