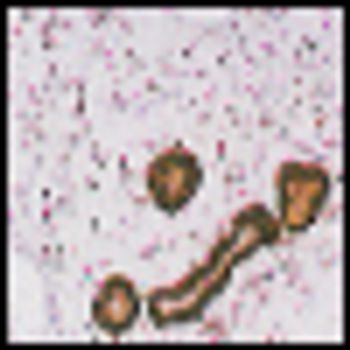
Thromboembolism affects many patients with solid tumors and clonalhematologic malignancies. Pathogenetic mechanisms include inflammatory-and tissue factor-mediated coagulation, natural anticoagulantdeficiencies, fibrinolytic alterations, hyperviscosity, and activationof platelets, endothelial cells, and leukocytes. High rates of venousthromboembolism (VTE) occur with advanced pancreatic, breast, ovarian,germ cell, lung, prostate, and central nervous system cancers.Hodgkin disease, non-Hodgkin's lymphoma, myeloma, paroxysmalnocturnal hemoglobinuria, and certain leukemias also predispose tovenous thromboembolism. Arterial and venous events occur with polycythemiavera and essential thrombocythemia. Central venous cathetersand prothrombotic antitumor regimens augment the risk in somepatients. Part 1 of this two-part article addresses pathophysiology, clinicalpresentations, and risk of malignancy-associated thrombosis. Part 2,which will appear in next month's issue, covers prophylaxis and treatmentof these thromboembolic complications.