
The phase II portion of the GAUGUIN study found promising activity with the anti-CD20 antibody obinutuzumab in patients with relapsed or refractory indolent NHL.

The phase II portion of the GAUGUIN study found promising activity with the anti-CD20 antibody obinutuzumab in patients with relapsed or refractory indolent NHL.

Older multiple myeloma patients exposed to novel agents prior to autologous peripheral blood stem cell transplantation were at increased risk for engraftment syndrome.

A phase I/II study found that radioimmunotherapy with 177Lu and the anti-CD20 antibody rituximab along with the chelator DOTA is safe and feasible for treatment of relapsed follicular, mantle cell, or other indolent lymphomas.

Palliation is a laudable concept and an important goal in the therapy of all patients with malignant disease. Unfortunately, in the current day and age, the adjective “palliative” is being used in a derogatory manner that suggests palliation of suffering somehow lessens the importance or impact that such a therapy has upon individuals with the disease.

By inhibiting inflammatory cytokines and controlling the signs and symptoms of myelofibrosis, the patient’s body condition improves as the disease is kept under good control. Ultimately, prolonged exposure of a patient with myelofibrosis to ruxolitinib at a clinically effective dose results in prolongation of the his or her life.
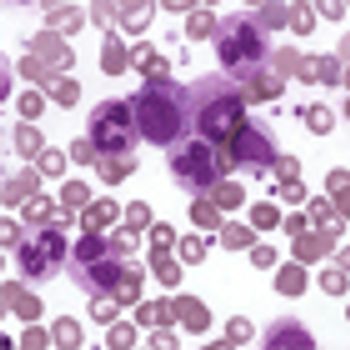
A new study validates a simple prognostic score, the EUTOS score, as a useful tool in predicting the therapeutic effects of TKIs for chronic myeloid leukemia.
ARIAD has received marketing authorization from the European Commission for ponatinib (Iclusig) in chronic myeloid leukemia and acute lymphoblastic leukemia.

In this interview we discuss acute myeloid leukemia therapy approaches and new molecular targets based on genetic analyses of the disease with a leukemia expert.

The International Myeloma Working Group recently released new recommendations to aid physicians in the treatment of bone disease related to multiple myeloma.
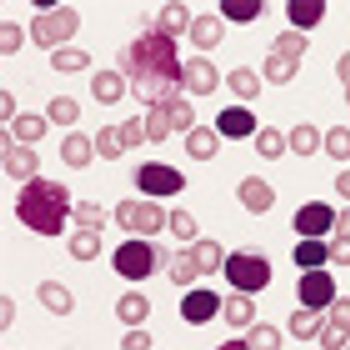
Monotherapy with the investigational oral Bruton's tyrosine kinase inhibitor ibrutinib was well tolerated and produced durable responses in a phase Ib/II, open-label, multicenter study of 85 patients with relapsed/refractory chronic lymphocytic leukemia or small lymphocytic lymphoma.
Use of the bisphosphonate pamidronate (Aredia) may be “more efficient” than standard regimens as palliative treatment for symptoms of acute symptomatic osteonecrosis in pediatric patients with acute lymphoblastic leukemia.
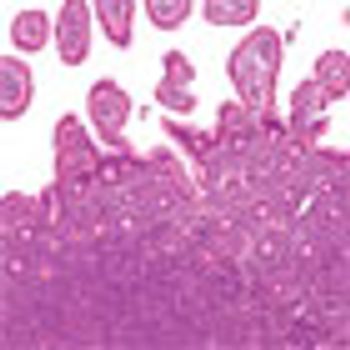
Phase II trial results of the targeted agent ibrutinib in relapsed or refractory mantle-cell lymphoma show that the drug led to promising and durable responses.
Results from a first-in-human trial of daratumumab indicate that the investigational drug reduced paraprotein and bone marrow plasma cells at doses greater than 4 mg/kg in patients with advanced multiple myeloma.
Almost half of patients with chronic-phase chronic myeloid leukemia (CML) who discontinued imatinib treatment did not relapse, according to results of a prospective study. Those who did relapse showed continued sensitivity to imatinib when treatment started again.
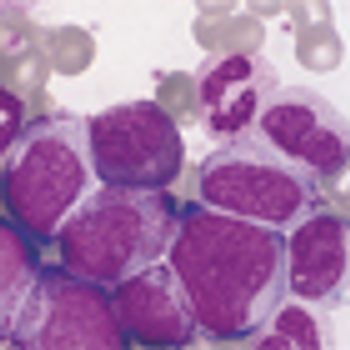
A phase II study found that an alternative imatinib treatment schedule for elderly patients with chronic myeloid leukemia (CML) could be an effective way to reduce dosing requirements of the drug.

Pomalidomide in combination with low-dose dexamethasone had a highly significant benefit on progression-free survival and overall survival compared with single-agent high-dose dexamethasone in patients with relapsed or refractory multiple myeloma, according to updated results of the MM-03 trial presented at the ASCO 2013 Annual Meeting.

Multiparameter flow cytometry and deep sequencing were both able to accurately identify patients with multiple myeloma who were negative for minimal residual disease, a factor that was found to better predict prolonged survival compared with complete response as measured by traditional response criteria.
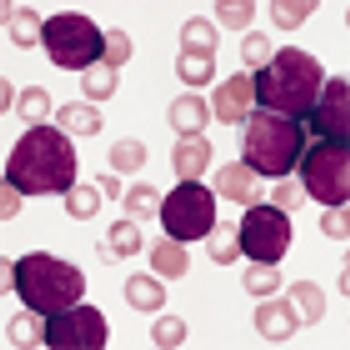
Findings suggesting that obesity substantially impairs the ability of L-asparaginase to kill leukemia cells were reported last month by investigators from The Saban Research Institute, Children’s Hospital Los Angeles.

If systemic treatment is effective enough to reliably control not only microscopic but also bulky disease, there will be little role for radiotherapy. And if systemic treatment cannot even reliably control microscopic disease, let alone macroscopic disease, there will be little role for radiotherapy, either. However, there are patients who fall into neither of these categories, and in them radiotherapy may well have a role.

DLBCL of any stage remains a systemic disease with early hematogenous spread. Thus, arguments advocating the role of IFRT do not truly address disease biology, and all future efforts to cure patients will require improved systemic therapy.
Two studies found higher rates of peripheral artery occlusive disease in nilotinib-treated chronic myeloid leukemia patients than in imatinib-treated patients.

Researchers have characterized acute myeloid leukemia, providing new genetic driver leads to help classify the disease and even stratify AML patients by risk.
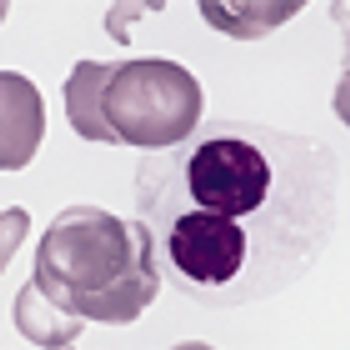
Multiple myeloma patients are at increased risk of developing myelodysplastic syndrome or acute leukemia after maintenance lenalidomide or thalidomide treatment, according to a new study.
A majority of patients with multiple myeloma are being treated with novel agents such as thalidomide, bortezomib, and lenalidomide within a year of diagnosis instead of the chemotherapeutic regimens that were more prevalent a decade ago, according to a new study.
A group of experts say that cancer drug prices, especially those for chronic myeloid leukemia, have skyrocketed, making patient treatment extremely difficult.