
Shift work is positively associated with higher levels of prostate-specific antigen (PSA) levels in men between the ages of 40 and 65, according to results of a new study.

Shift work is positively associated with higher levels of prostate-specific antigen (PSA) levels in men between the ages of 40 and 65, according to results of a new study.

Prostate tumors may not readily evolve from low to high grade, according to a new study. The results have important clinical implications for patients and clinicians when choosing active surveillance or treatment.

The long-term follow-up of the Prostate Cancer Prevention Trial confirms that finasteride reduces the risk of low-grade prostate cancer by one-third, but there were no significant survival differences between the two study arms.

Both Internet and print-based decision aids equally helped men make important decisions related to prostate cancer screening, but did not affect actual screening rates.

The ALSYMPCA phase III clinical trial, recently published, demonstrated that radium-223 dichloride was well-tolerated and resulted in an improvement in overall survival by 3.6 months compared with placebo.

Researchers have identified pathways that are important for prostate cancer growth after the tumor becomes resistant to androgen therapies.

A large and prospective study shows that a high concentration of omega-3 fatty acids is linked to a higher risk of aggressive prostate cancer.

We need to understand each patient’s cancer and its microenvironment well enough to develop targeted treatments that will kill the tumor the first time-for if we let it escape, 70 years of prostate cancer research teaches us that our job will only get harder.

Although high-level evidence is lacking, the existing literature indicates that select men with lymph node–positive prostate cancer benefit from local therapy.

Unfortunately, although agents in the pipeline each extend life, none are curative. Therefore, physicians who investigate and treat mCRPC have two paths they can follow to further improve outcomes.

Node-positive prostate cancer without distant metastases (T any, N+, M0) currently is encountered rarely, primarily because of the shift to diagnosis at earlier stages, a result of widespread PSA testing.

In this review, we focus on the testosterone/androgen receptor pathway that is being targeted with potent new agents; we also discuss other important alternative biologic pathways that have given rise to new therapeutics that may attenuate prostate cancer growth, survival, and propagation.

The “experts” should maintain a stringent standard regarding what merits further development and reconsider carefully and critically the available data before committing to PARP inhibition, attacks on the PI3K pathway, and vasoactive agents in prostate cancer.

Current evidence for the management of lymph node–positive prostate cancer suggests both a disease-control and survival benefit to systemic ADT plus surgery and radiation.

From 2004 to 2009, use of advanced treatment technologies increased among prostate cancer patients with low-risk disease and high risk of noncancer mortality.
A new imaging approach, combining PET with magnetic resonance (MR), was shown to be more sensitive in detecting recurrent prostate cancer compared with PET/CT.

In a new study presented at the Endocrine Society’s annual meeting, researchers using animal models show that early BPA exposure increases prostate cancer risk.

A new study shows that men diagnosed with prostate cancer may do better by substituting carbohydrates and saturated fats with plant-based fats such as those found in nuts and olive oil.

In my experience, being treated for low-volume Gleason 6 tumors is the norm, not the exception, for men in the United States. Surveillance may be discussed as an option, but it is not taken seriously.

The concept of active surveillance is based on the observation that Gleason 6 (pattern 3) prostate cancer is an indolent condition that poses little or no threat to the patient’s life. Conservative management is thus appropriate for these patients.

Further analyses of data subsets from the ALSYMPCA study of the alpha particle-emitting isotope Ra-223 (Xofigo) were presented at ASCO, providing additional evidence of efficacy and safety of the recently FDA approved therapeutic agent.
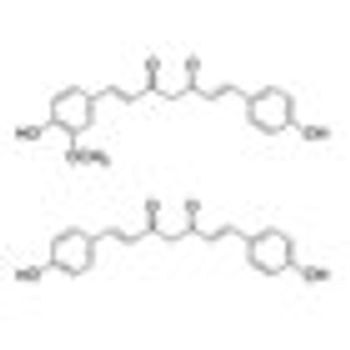
Addition of curcuminoids to treatment with docetaxel was well tolerated and showed promise in improving the response rate to docetaxel “in terms of both PSA decrease and objective response” in a phase II trial in patients with castration-resistant prostate cancer.
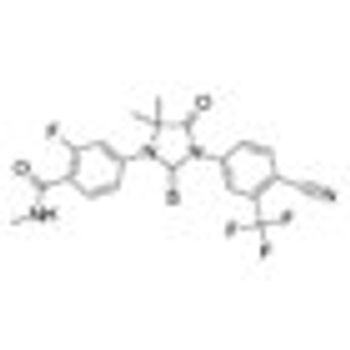
Monotherapy with enzalutamide (Xtandi) achieved a “high PSA response rate and marked PSA decline” in patients with hormone-naïve prostate cancer after 6 months in a single-arm, multicenter phase II study.
Treatment with 200 µmol per day of sulforaphane for 20 weeks was “feasible, safe,” and inhibited histone deacetylase (HDAC) function in a single-arm study of 20 patients who had non-castrate biochemical (PSA)-recurrence of prostate cancer despite surgery or radiation.

Ahead of the 2013 ASCO meeting we highlight some of this year's prostate cancer sessions, many of which focus on how best to use the new agents that have been approved recently, as well as looking into new drugs and combinations presented from early trials.