Leukemia
Latest News
Latest Videos

CME Content
More News
Patients with chronic lymphocytic leukemia or small lymphocytic leukemia treated with zanubrutinib, obinutuzumab, and venetoclax experienced increased rates of undetectable minimal residual disease in peripheral blood and bone marrow.
DNA Sequencing of Bone Marrow Is Predictive of ALL Relapse Following Treatment With Tisagenlecleucel
DNA sequencing to detect minimal residual disease and eventual relapse was more accurate than flow cytometry for adult and pediatric patients with acute lymphoblastic leukemia who have been treated with tisagenlecleucel.
Pediatric patients with KMT2A-rearranged acute myeloid leukemia who were treated with gemtuzumab ozogamicin plus standard chemotherapy experienced improved event-free survival and a reduced relapsed risk.

Patients with relapsed chronic lymphocytic leukemia who were treated with either limited or continuous venetoclax and rituximab experienced improved responses during a 5-year follow-up.
Investigators announced positive topline results for the phase 3 QuANTUM-First trial, assessing the use of quizartinib plus chemotherapy for adult patients with newly diagnosed FLT3-ITD–positive acute myeloid leukemia.

Patients with relapsed/refractory adult B-cell acute lymphoblastic leukemia who were treated with AUTO1 experienced durable responses.

“I’ve done a lot of work [not only with] clinical trials, but also understanding the disease, the prognostic factors, and the management of adverse effects.”
Patients with mutant-IDH2 acute myeloid leukemia experienced a better overall response rate when treated with enasidenib plus azacitidine compared with azacitidine alone.
A phase 1b/2 trial found that the combination of enasidenib plus azacytidine improved overall responses and was well tolerated compared with azacytidine monotherapy for patients with newly diagnosed, mutant-IDH2 acute myeloid leukemia.

A phase 2 study found that acalabrutinib monotherapy followed by treatment with venetoclax and obinutuzumab in the frontline setting was highly active and tolerable for patients with previously untreated chronic lymphocytic leukemia despite not meeting the primary end point.

The FDA granted accelerated approval to asciminib for the treatment of patients with Philadelphia chromosome–positive chronic myeloid leukemia for 2 indications.

ASTCT recently published an article in their journal Nucleus detailing CAR T therapy in patients with acute lymphoblastic leukemia.
In a debate, experts discuss the importance of IGHV and TP53 mutational status in predicting response to novel therapies in chronic lymphocytic leukemia.
Ibrutinib for treating patients with chronic lymphocytic leukemia increased the risk of atrial fibrillation, bleeding, and heart failure in results of a cohort study.

Patients with chemotherapy-refractory, high-risk acute myeloid leukemia achieved promising benefit from treatment with ficlatuzumab and cytarabine.
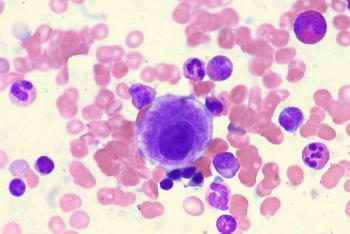
Adding venetoclax to cladribine, high-dose cytarabine, and idarubicin appears to yield high rates of minimal residual disease negativity and promising survival in patients with newly diagnosed acute myeloid leukemia and high-risk myelodysplastic syndrome.

The FDA has approved the use of CD19-directed CAR T-cell therapy brexucabtagene autoleucel for adult patients with relapsed/refractory precursor acute lymphoblastic leukemia.

A recently published article on CAR T cells in patients with acute myeloid leukemia is featured by CancerNetwork's Strategic Alliance Partner ASTCT.
As more novel therapeutic targets are discovered in patients with chronic lymphocytic leukemia, the more possibilities are presented in terms of treatment with targeted agents, small molecules, and cellular therapies.
Patients with previously treated chronic lymphocytic leukemia and small lymphocytic lymphoma appeared to benefit from treatment with pirtobrutinib.

The latest episode of the ASTCT Talks episode features John DiPersio, MD, PhD, on emerging therapies in the treatment of acute myeloid leukemia.
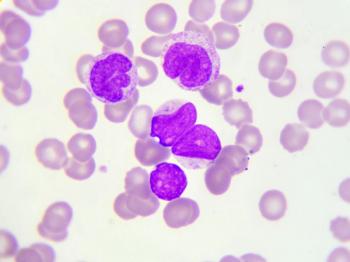
Strong response rates were observed with pirtobrutinib across dose levels to treat patients with chronic lymphocytic leukemia and small lymphocytic lymphoma ion a phase 1/2 study.

The introduction of targeted therapies and immunotherapeutics may work to improve survival for patients with T-cell acute lymphoblastic leukemia.

Clinical decision-making based on minimal residual disease may be associated with improved therapy satisfaction and optimized post-remission treatment for patients with intermediate-risk acute myeloid leukemia.

A recent study provides evidence showing that focal 22q11.22 deletions may be correlated with poor outcomes in patients with pediatric B-cell acute lymphoblastic leukemia with alterations in IKZF1.