
To find a new cure for a disease, or at least to significantly prolong patient survival, requires a bit of insight and a lot of luck.

To find a new cure for a disease, or at least to significantly prolong patient survival, requires a bit of insight and a lot of luck.

The current dogma considers cytomegalovirus (CMV) seropositivity being associated with inferior outcomes post hematopoietic stem cell transplant (HSCT). However, there has been a notion of “virus-versus-leukemia” effect since the 1980s; and recently, there have been some interesting reports which may turn this to a hot topic.

A rarely noted aspect of the era of novel agents and explosive new knowledge in the clonal plasma cell diseases is how short the half-life of relevant information has become, and how this churning has challenged clinical thinking.

In this issue of ONCOLOGY, Dr. Robert Kyle and colleagues provide their clinical and epidemiological perspective on monoclonal gammopathy of undetermined significance (MGUS) and smoldering myeloma (SMM)-a perspective that is based on more than three decades of experience.

In his plenary address as outgoing president of ASCO, Dr. George Sledge proposed that we are on the brink of a new era in cancer therapy – an era of genome-based treatment. He stressed that this new “genomic era” holds great promise for patients, citing as evidence a recent paper in JAMA that described a case in which the results of deep sequencing of a patient’s leukemic cells led to successful individualized therapy.
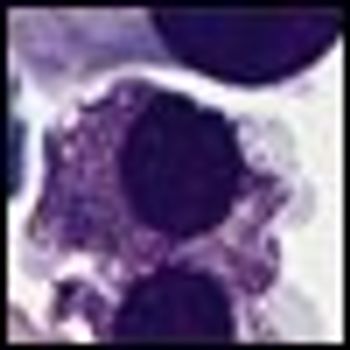
A growing understanding of the biology behind myelodysplastic syndromes (MDS) is leading the way to improved treatment options, according to two presentations at the American Society of Clinical Oncology (ASCO) Annual Meeting in Chicago.
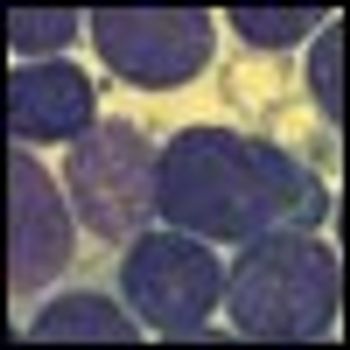
Despite dramatic improvements in survival for children and young adults with acute lymphoblastic leukemia (ALL), treatment failure in the central nervous system remains a constant foe.

ONCOLOGY talks with Dr. Susan O’Brien, professor in the department of leukemia at the MD Anderson Cancer Center. Dr. O’Brien will be one of the presenters at the upcoming ASCO session on therapies for chronic lymphocytic leukemia, and she gives us a preview of what some of the highlights of the session are likely to be, as well as some insights into her own work.
In an article published online on May 9, 2011 in the Journal of Clinical Oncology, a large-scale prospective study found that acetaminophen use was associated with an almost two-fold increase risk of hematological malignancies other than chronic lymphocytic leukemia/small lymphocytic lymphoma.

Myelodysplastic syndromes, also referred to collectively as MDS, have significant biological and clinical heterogeneity, a highly variable natural history, and a complex pathobiology that is not clearly understood.

The myelodysplastic syndromes (MDS) are a heterogeneous spectrum of clonal hematopoietic diseases characterized by bone marrow hypercellularity, dysplasia of cellular elements, and consequent inadequate hematopoiesis, with resultant peripheral blood cytopenias.

The review by Dr. Akhtari outlines the diagnosis, prognosis, and treatment options for patients with myelodysplastic syndromes (MDS), and touches on the current challenges in treating patients suffering from MDS.

This review will cover the key elements of modern acute lymphoblastic leukemia treatment regimens, focusing primarily on front-line treatment and concluding with a brief discussion of the management of relapsed disease.

We have witnessed remarkable gains in the biological understanding and treatment of acute lymphoblastic leukemia (ALL) over the past decade.

About 35 years ago, I encountered several children and adolescents with acute lymphoblastic leukemia or widespread non-Hodgkin lymphoma who presented with or who developed, upon initiation of therapy, severe renal and metabolic derangements.

Dr. Sonali Smith discusses the newest developments in the treatment of CML.

Dr. Jorge Cortes discusses new data on bosutinib, a new tyrosine kinase inhibitor for CML.

The accurate and in-depth documentation of learning gaps is a fundamental aspect of developing continuing education activities. To obtain a better understanding of community-based medical oncology practice patterns, 43 oncologists within the United States were recruited to complete a traditional clinical case–based questionnaire and to contribute specific anonymous demographic and treatment information derived from their actual patients. This information was used to create a cross-sectional case database on two types of cancer in which major clinical advances have been reported in recent years - multiple myeloma and follicular lymphoma. These diseases also are similar in that most patients experience clinically meaningful benefits from systemic treatment but are unlikely to be cured by therapy. As further described in this and the subsequent two articles, this case-based series documents that (a) clinical research advances are being quickly implemented in daily patient care and that (b) although therapeutic strategies vary based on patient age, the short-term outcomes in terms of response to and tolerance of treatment are similar in younger and older patients.

At a median follow-up of 36 months, multiple survival rates were nearly perfect at 99%. The leader of the Italian study called the low number of treatment failures reassuring news as to the durability of nilotinib response at three years post-therapy

The median reductions in Bcr-Abl transcripts at one year were greater with dasatinib (Sprycel) than with imatinib (Gleevec), according to the results of an intergroup phase II trial. A better molecular response should eventually correlate with better outcomes, making dasatinib a serious contender for upfront therapy in CML.

The likelihood of patients achieving complete cytogenetic response at any time was 1.5 times higher with dasatinib (Sprycel) than with imatinib (Gleevec), according to an investigator with the DASISION trial.

Nplate sustains platelet counts in patients with adult chronic immune (idiopathic) thrombocytopenic purpura (ITP) while single-dose Zevalin offers survival advantage in non-Hodgkin’s lymphoma.

The 24-month follow-up data from the ENESTnd trial showed that patients treated with nilotinib (Tasigna) had significantly better response rates and significantly lower rates of progression to accelerated phase or blast crisis when on treatment

Patients with early-stage Hodgkin’s lymphoma and a favorable prognosis can be treated with less intensive chemotherapy and radiotherapy regimens without affecting outcomes. This is the first study to show that less intensive therapy can be used without sacrificing benefits, according to lead author Andreas Engert, MD, and colleagues.
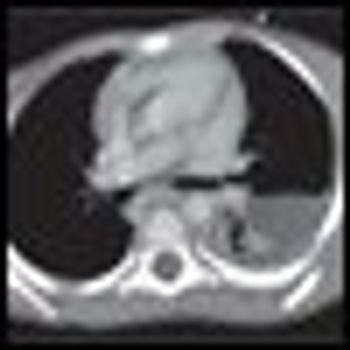
Here we present the case of a 3-year-old girl with generalized lymphadenopathy and fever, in whom the cause of the symptoms was initially thought to be infectious. Ultimately, however, anaplastic large cell lymphoma (ALCL) was diagnosed. Using this case as a backdrop, we discuss the wide range of systemic illnesses that the differential diagnosis of generalized lymphadenopathy encompasses.