
In this interview we discuss acute myeloid leukemia therapy approaches and new molecular targets based on genetic analyses of the disease with a leukemia expert.

In this interview we discuss acute myeloid leukemia therapy approaches and new molecular targets based on genetic analyses of the disease with a leukemia expert.
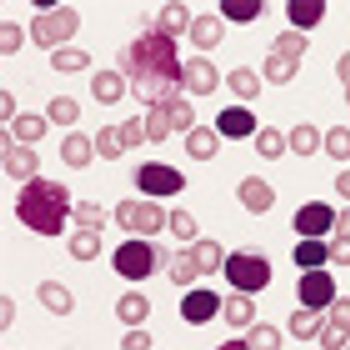
Monotherapy with the investigational oral Bruton's tyrosine kinase inhibitor ibrutinib was well tolerated and produced durable responses in a phase Ib/II, open-label, multicenter study of 85 patients with relapsed/refractory chronic lymphocytic leukemia or small lymphocytic lymphoma.
Use of the bisphosphonate pamidronate (Aredia) may be “more efficient” than standard regimens as palliative treatment for symptoms of acute symptomatic osteonecrosis in pediatric patients with acute lymphoblastic leukemia.
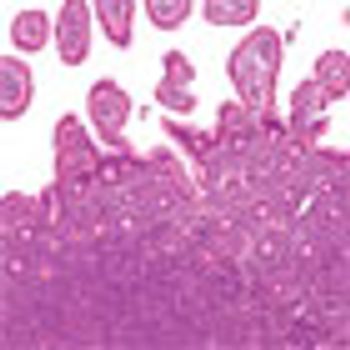
Phase II trial results of the targeted agent ibrutinib in relapsed or refractory mantle-cell lymphoma show that the drug led to promising and durable responses.
Almost half of patients with chronic-phase chronic myeloid leukemia (CML) who discontinued imatinib treatment did not relapse, according to results of a prospective study. Those who did relapse showed continued sensitivity to imatinib when treatment started again.
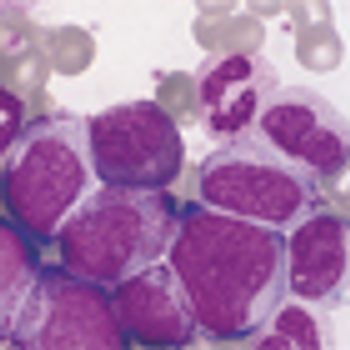
A phase II study found that an alternative imatinib treatment schedule for elderly patients with chronic myeloid leukemia (CML) could be an effective way to reduce dosing requirements of the drug.
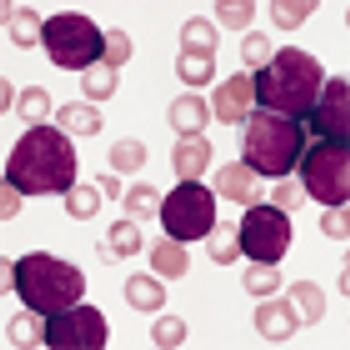
Findings suggesting that obesity substantially impairs the ability of L-asparaginase to kill leukemia cells were reported last month by investigators from The Saban Research Institute, Children’s Hospital Los Angeles.

DLBCL of any stage remains a systemic disease with early hematogenous spread. Thus, arguments advocating the role of IFRT do not truly address disease biology, and all future efforts to cure patients will require improved systemic therapy.
Two studies found higher rates of peripheral artery occlusive disease in nilotinib-treated chronic myeloid leukemia patients than in imatinib-treated patients.

Researchers have characterized acute myeloid leukemia, providing new genetic driver leads to help classify the disease and even stratify AML patients by risk.
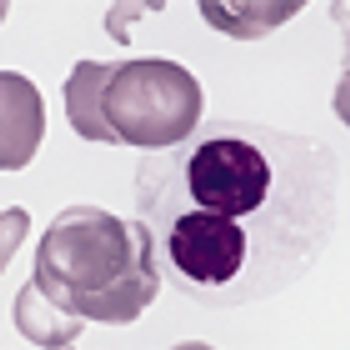
Multiple myeloma patients are at increased risk of developing myelodysplastic syndrome or acute leukemia after maintenance lenalidomide or thalidomide treatment, according to a new study.
A group of experts say that cancer drug prices, especially those for chronic myeloid leukemia, have skyrocketed, making patient treatment extremely difficult.
Targeting the bone marrow–specific extracellular matrix osteopontin may be an effective strategy to increase the efficacy of chemotherapy in patients with acute lymphocytic leukemia, according to the authors of a recent study.
A dose-adjusted regimen of etoposide, doxorubicin, and cyclophosphamide with vincristine, prednisone, and rituximab (DA-EPOCH-R) obviated the need for radiotherapy in patients with primary mediastinal B-cell lymphoma in a single-group, phase II, prospective study.
A study of patients with chronic myeloid leukemia treated with imatinib found that chronic fatigue is the major factor that limits health-related quality of life.
A majority of patients on imatinib for treatment of GIST or CML had low or absent levels of osteocalcin, a bone marker secreted by osteoblasts, and about 50% of patients had a decrease in bone mineral density, signaling that long-term treatment may affect bone health in these patients.
CML patients treated with nilotinib had fewer treatment-emergent BCR-ABL mutations than those treated with imatinib, and among patients who did have a mutation, those treated with nilotinib had reduced rates of progression to accelerated phase and blast phase of the disease.
Researchers have identified a novel monoclonal antibody directly targeted against a receptor found in abundance on chronic lymphocytic leukemia (CLL) cells, but not normal B cells. The humanized antibody can directly kill CLL cells.

Researchers have discovered a fully human “T-cell receptor–like” monoclonal antibody specific for the Wilms tumor 1 oncoprotein-an intracellular oncogenic transcription factor that is overexpressed in a wide range of leukemias, as well as solid cancers.
Combination chemotherapy with sequential administration of methotrexate and asparaginase was found to be effective salvage therapy in a small retrospective study of pediatric patients with relapsed or refractory acute myeloid leukemia (AML).
Contrary to previous laboratory findings, a new study has shown for the first time the effect of stem cell burden on treatment outcome, discovering that tyrosine kinase inhibitors, including imatinib and dasatinib, can rapidly eradicate most chronic myeloid leukemia stem cells.
The European Medicines Agency adopted a “positive opinion” earlier this year regarding conditional marketing approval for bosutinib for the treatment of Philadelphia chromosome-positive chronic myeloid leukemia.
Findings of a newly published study by an international team of researchers suggest that targeting growth factor independence 1 (GFI1) may improve the prognosis of patients with T-cell acute lymphoblastic leukemia or other lymphoid leukemias.
Researchers from the University of Rochester have identified BCL2 inhibitors as potential leukemia stem cell-targeting agents, demonstrating that two such inhibitors killed inactive and metabolically slower leukemia stem cells.
New research suggests that a novel, investigative drug could help alleviate some of the resistance to tyrosine kinase inhibitor treatment seen in chronic myeloid leukemia (CML). The drug, a pan-BCL2 inhibitor called sabutoclax, could sensitize malignant leukemic stem cells in the bone marrow niche to TKI treatment.