
The FDA granted a breakthrough therapy designation to abatacept for the prevention of moderate to severe acute graft-versus-host disease in hematopoietic stem cell transplants from unrelated donors.
Acalabrutinib Regimens Improve PFS in Treatment-Naïve Patients with CLL
Frontline Ibrutinib/Venetoclax Provides High Rates of Undetectable MRD in CLL

The FDA granted a breakthrough therapy designation to abatacept for the prevention of moderate to severe acute graft-versus-host disease in hematopoietic stem cell transplants from unrelated donors.
Additional positive interim safety and efficacy data were reported for annamycin in the treatment of patients with relapsed or refractory acute myeloid leukemia.

As part of Project Orbis, The FDA has approved acalabrutinib for the treatment of adult patients with chronic lymphocytic leukemia or small lymphocytic lymphoma.

A new study in the Journal of Clinical Oncology finds that a subset of pediatric ALL relapses may be triggered by the very chemotherapy which helped patients beat the cancer the first time.

The National Comprehensive Cancer Network recently issued new guidelines on best practices in evaluating patients for hematopoietic cell transplantation, as well as how to manage complications associated with the procedure.
Treatment with gilteritinib improved survival and increased remission rates, compared with salvage chemotherapy, among patients with relapsed or refractory FLT3-mutated acute myeloid leukemia.
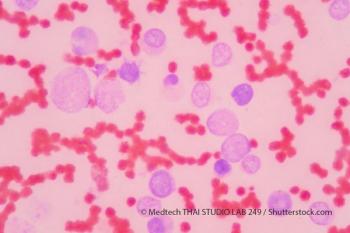
Treatment with SY-1425 in combination with azacitidine induced a 62% complete response rate with incomplete blood count recovery rate among unfit patients with RARA-positive AML.

Jennifer Crombie, MD, discusses classification of diffuse large B-cell lymphoma (DLBCL) into distinct subtypes and treatment decisions based on molecular classifications.
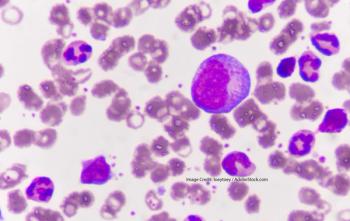
Researchers explore the predictive capability of EVI1 expression.
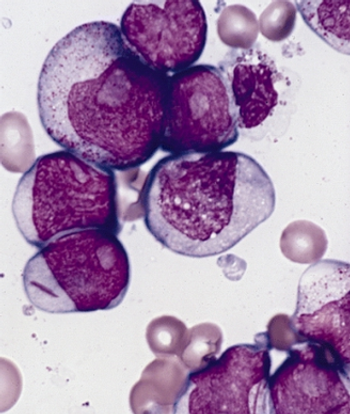
Researchers report on the BRIGHT AML 1019 Phase III trial.
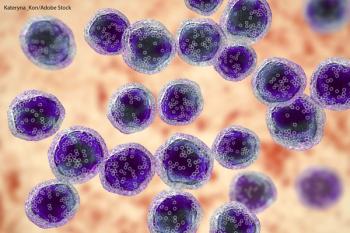
MYC-rearrangement within 2 years after diagnosis may affect the prognosis of patients with diffuse large B-cell lymphoma.
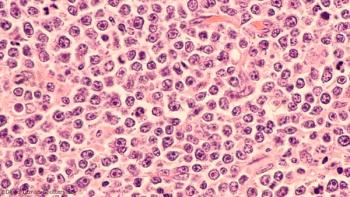
A new study looks into whether disease stage at diagnosis affects the occurrence and location of a second primary malignancy in DLBCL.
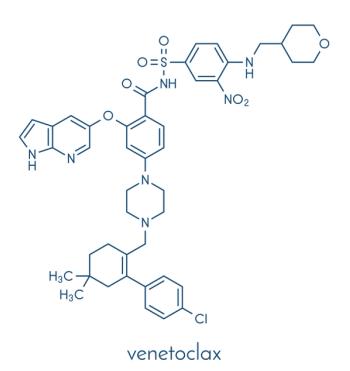
With FDA-approved indications for both chronic lymphocytic leukemia and acute myeloid leukemia, and continued investigation within multiple disease states, venetoclax has become an exciting oral targeted therapy among oncologists.
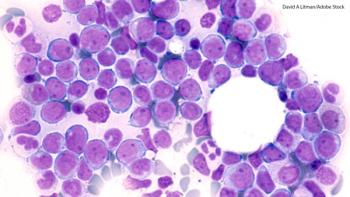
In this study, FLT3-IRAK1/4 inhibitor (NCGC1481) removed adaptively resistant FLT3-mutant AML cells.
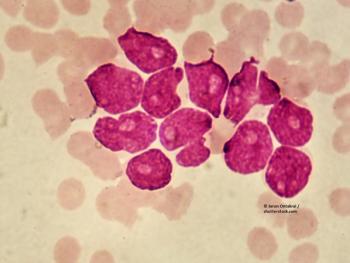
Prognostic signature associated with AML relapse risk potential harbors gene subsets that apply to only certain patient subgroups.
While ibrutinib plus rituximab may improve progression-free survival in chronic lymphocytic leukemia, it is a costly option for some patients.
A total of 30 patients were enrolled in an expansion cohort for relapsed/refractory primary mediastinal B-cell lymphoma and received nivolumab and brentuximab vedotin.
Delays in CAR T-cell therapy may significantly decrease gains in survival and productivity for patients with diffuse large B-cell lymphoma and pediatric acute lymphoblastic leukemia.
Researchers looked at the pre-transplant PET/CT Deauville scores of patients with relapsed or refractory diffuse large B-cell lymphoma treated with R-DHAC to see if patients with a higher score had a higher risk for treatment failure.
The US Food and Drug Administration recently approved gilteritinib (Xospata), in addition to final trial data from the phase 3 ADMIRAL trial, making it the new standard of care for acute myeloid leukemia.

ONCOLOGY discussed therapy options, including chimeric antigen receptor (CAR)-T-cell therapies for pediatric acute lymphoblastic leukemia (ALL), with Susan R. Rheingold, MD, Medical Director of the Oncology Outpatient Clinic and attending physician with the Cancer Center at Children’s Hospital of Philadelphia.

A new report suggests targeting the Gal9/TIM3-axis could help boost chances of complete remission in patients with acute myeloid leukemia.
Researchers utilized a targeted next-generation sequencing (NGS) panel developed at Oregon Health & Science University to assess the clearance of mutations after therapy, clonal evolution at relapse, and combinations of mutations.

The CLARITY trial looked at measurable residual disease negativity in 54 patients with relapsed or refractory chronic lymphocytic leukemia who received ibrutinib in combination with venetoclax.
While many patients with follicular lymphoma did well with this new regimen, the majority of those who did have disease progression had transformed disease.