
This study indicated that caregivers saw improved quality of life, reduced caregiving burden, lower anxiety and depression symptoms, and improved self-efficacy and coping skills having received psychosocial intervention.

This study indicated that caregivers saw improved quality of life, reduced caregiving burden, lower anxiety and depression symptoms, and improved self-efficacy and coping skills having received psychosocial intervention.
Naval Daver, MD, explains the progress made on 3 abstracts he’s involved with regarding acute myeloid leukemia (AML) at the ASH Annual Meeting and Exposition.
Researchers developed a risk score assessment to measure potential risk for chemotherapy-induced heart failure
Courtney DiNardo, MD, MSCE, elaborated on interim phase II results regarding enasibenib plus azacitidine in patients with newly diagnosed acute myeloid leukemia, and the results from the QUAZAR trial.

The associate professor at The Ohio State University Comprehensive Cancer Center explained the goals for the future of the CAR T-cell therapy data in patients with DLBCL.
The medical oncologist from the John Theurer Cancer Center noted the importance of real-world data in determining potentially different toxicity profiles in these BTK-inhibitors.

Though physical activity guidelines are largely based on chronic diseases like cardiovascular disease and diabetes, these data suggest they are important to cancer prevention as well.

The study evaluating itacitinib in combination with corticosteroids in patients with treatment-naïve acute graft-versus-host disease did not produce statistically significant results.

A phase I study showed brentuximab vedotin combined with a standard chemotherapy regimen of mitoxantrone, etoposide, and cytarabine may be safe and well tolerated in patients with relapsed/refractory acute myeloid leukemia.

Diego Villa, MD, FRCPC, elaborated on the progress made with bendamustine and rituximab as induction therapy for transplant eligible and ineligible patients with mantle cell lymphoma.

The expert hematologist from Plymouth University Medical Center discussed the long-term outcomes of patients receiving ibrutinib for mantle cell lymphoma at the ASH Annual Meeting and Exposition.
The Ohio State University Comprehensive Cancer Center expert discussed the ongoing Alliance A041702 trial at the ASH Annual Meeting and Exposition.

The Willamette Valley Cancer Institute and Research Center expert talks about the results of the ELEVATE TN trial at the ASH Annual Meeting and Exposition.

Bijal D. Shah, MD, discusses the progress made regarding CAR T-cell therapy and mantle cell lymphoma.


The associate professor at The Ohio State University Comprehensive Cancer Center discussed the implications of her analysis of the CAR T-cell therapy tisagenlecleucel for patients with diffuse large B-cell lymphoma at the ASH Annual Meeting & Exposition.


The Swedish Cancer Center expert discussed the addition of polatuzumab vedotin to a bendamustine-rituximab regimen at the ASH Annual Meeting & Exposition.

Andre H. Goy, MD, MS, from Hackensack University Medical Center, discussed ways to address the extension of survival for patients with DLBCL who achieved a complete remission at the ASH Annual Meeting & Exposition.
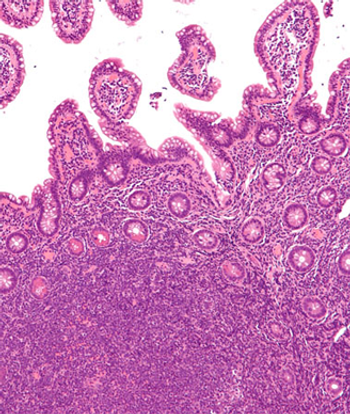
The ZUMA-II trial suggested that patients with relapsed/refractory mantle cell lymphoma resistant to prior therapies may benefit from the autologous anti-CD19 CAR T-cell therapy.

Matthew S. Davids, MD, MMSc, discussed his phase I/II study of duvalisib combined with venetoclax for patients with relapsed/refractory CLL and SLL at the ASH Annual Meeting & Exposition.
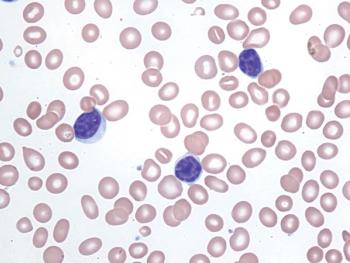
The combination of ibrutinib and rituximab demonstrated superior progression-free survival in older patients with previously untreated chronic lymphocytic leukemia.
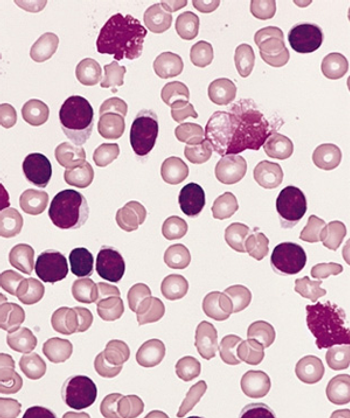
The triplet regimen consisting of acalabrutinib, venetoclax, and obinutuzumab appeared highly active as frontline therapy for patients with chronic lymphocytic leukemia.
Lisocabtagene maraleucel induced high response rates in patients with aggressive relapsed/refractory large B-cell lymphoma.
Treatment with lenalidomide and rituximab improved progression-free survival, compared with placebo in patients ≥70 years old with indolent non-Hodgkin lymphoma.