
The immunotherapeutic rindopepimut with bevacizumab yielded a significant survival improvement in relapsed glioblastoma patients with a EGFRvIII mutation.

The immunotherapeutic rindopepimut with bevacizumab yielded a significant survival improvement in relapsed glioblastoma patients with a EGFRvIII mutation.

A phase I trial of an oncolytic polio/rhinovirus vaccine was safe and showed promising efficacy in patients with recurrent glioblastoma.

Treating newly diagnosed glioblastoma with ��“tumor treating fields” is a safe and effective therapeutic option, according to a new trial.

A combination of bevacizumab and lomustine showed promise in a randomized phase II trial of patients with recurrent glioblastoma, according to study results.
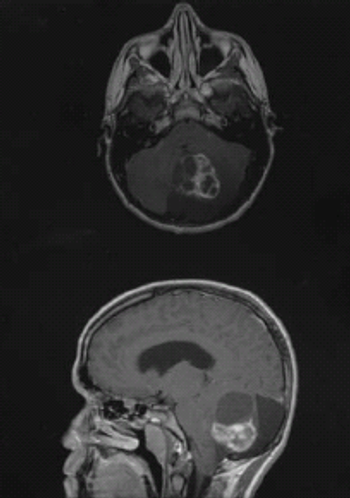
The addition of procarbazine, CCNU, and vincristine to RT in patients with low-grade glioma prolongs progression-free and overall survival vs RT alone.
As part of our Society of Neuro-Oncology annual meeting coverage, we discuss quality of life issues and neurologic rehabilitation in patients with neuro-oncologic diseases.

Prevention of CNS seeding early in the metastatic disease course using drugs with both intra- and extracranial activity will be crucial to improving outcomes in patients with breast cancer brain metastases.

Brain metastases arising from breast cancer constitute a clinically unmet need and a situation that portends a poor prognosis with few therapeutic options.
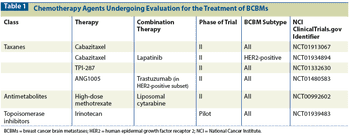
In this overview, we will review recent developments in the management of breast cancer brain metastases and current prospective trials of systemic therapies specifically for patients with breast cancer brain metastases, with a focus on novel pathway-specific therapies.

For many women, the prospect of tumors growing in their brain that may eventually impact their ability to communicate, interact, and remember is terrifying.

High-dose chemotherapy plus conventional radiotherapy resulted in a high 3-year overall survival in children and adolescents with newly diagnosed medulloblastoma and supratentorial primitive neuroectodermal tumor.

Addition of the drug armodafinil did not improve measures of fatigue in patients with gliomas undergoing treatment with radiotherapy, according to the results of a study presented at the 2014 ASCO Annual Meeting.
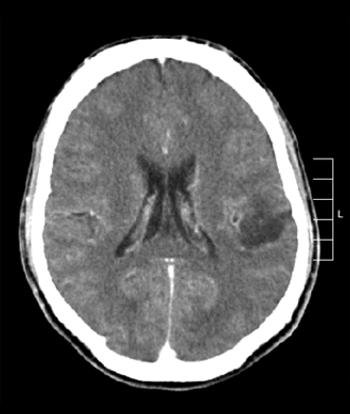
Researchers identified a six-gene signature that can help to predict the 3-year survival outcome for patients with grade II or grade III gliomas, independent of the patient’s histology, grade, and IDH1 mutations status.
A phase II trial evaluating the use of a dendritic cell vaccine, ICT-107, has shown that the immunotherapy had a positive effect on progression-free survival in patients with glioblastoma.
Positron emission tomography using [18]F-fluorothymidine as a tracer failed to distinguish true progression of glioblastoma from pseudoprogression in a small single-center study presented at the 2014 ASCO Annual Meeting.

As part of our coverage of the 2014 American Society of Clinical Oncology (ASCO) Annual Meeting, we discuss how molecular diagnosis in medulloblastoma affects clinical decision-making.
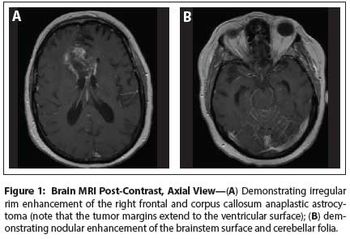
The patient is a 58-year-old woman who was diagnosed at an outside hospital with a World Health Organization (WHO) grade III non–contrast-enhancing right frontal anaplastic astrocytoma, with spread into the genu of the corpus callosum.

Significant progress has been made in defining molecular signatures in diffuse gliomas. The clinically significant genetic alterations identified to date probably represent the tip of the iceberg, since new, potentially significant biomarkers are continuously described.
We review the current data regarding the prognostic and predictive value of IDH mutation and 1p/19q codeletion in gliomas. We also discuss possible management algorithms using these biomarkers to tailor surgical and adjuvant therapy for specific diffuse gliomas.

Results of two phase III trials, presented at ASCO, on the addition of bevacizumab (Avastin) to standard therapy in newly diagnosed glioblastoma found that the drug added no benefit.

A turning point in therapy followed the observation that patients with AO tumors with chromosome 1p and 19q codeletion had better outcomes when treated with irradiation and PCV than did non-codeleted anaplastic oligodendroglioma patients.

In light of the high bar that must be met for results to be truly practice-changing, and of the long period of time before survival results are mature in an indolent disease, the primary endpoint for clinical trials in anaplastic oligodendroglial tumors needs rethinking.

Although important questions still remain regarding chemotherapy choice, sequence, and dosing, the answers to which will require additional large phase III trials, radiotherapy alone is no longer appropriate therapy for 1p/19q codeleted anaplastic oligodendrogliomas.
The combination of whole-brain radiation therapy and the EGFR inhibitor erlotinib showed a promising response rate and was well tolerated in a new phase II trial of patients with brain metastases from non-small-cell lung cancer.
Higher levels of the enzyme kallikrein 6 (KLK6) are associated with glioblastoma multiforme, the most common type of brain tumor, according to a new study from researchers at the Mayo Clinic.