Lymphoma
Latest News
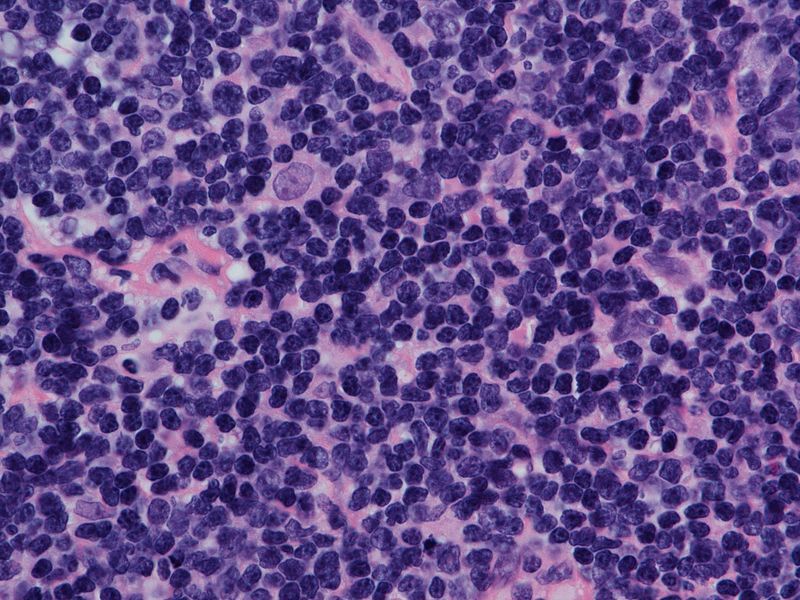
Brexu-cel Yields Consistent Efficacy in R/R Mantle Cell Lymphoma in SOC Setting
Latest Videos

CME Content
More News

The approval for pirtobrutinib in the treatment of patients with relapsed or refractory mantle cell lymphoma was based on data from the phase 1/2 BRUIN trial.
Hun Ju Lee, MD, reviews results from part C of the phase 2 SGN35-27 trial for patients with early-stage classical Hodgkin lymphoma treated with brentuximab vedotin plus nivolumab, doxorubicin, and dacarbazine.

An expert from The University of Texas, MD Anderson Cancer Center says that a brentuximab vedotin–based combination was well-tolerated in patients with advanced-stage Hodgkin lymphoma, according to results presented at 2022 ASH.

An expert from Rutgers Cancer Institute discusses ongoing research for mosunetuzumab in relapsed/refractory follicular lymphoma, as well as the importance of deploying the agent in the community setting.

An expert from Rutgers Cancer Institute indicates that mosunetuzumab may limit unmet needs commonly associated with CAR T-cell therapy such as cost, tolerability, and access.

LP-284, which now has orphan drug designation from the FDA for mantle cell lymphoma, yielded positive preclinical data at the 2022 American Society of Hematology Annual Meeting and Exposition.

An expert from Rutgers Cancer Institute reviews data that lead to the approval of mosunetuzumab for patients with relapsed/refractory follicular lymphoma.

In a population of patients with patients with mantle cell lymphoma and follicular lymphoma, zandelisib plus zanubrutinib did not increase the rate or severity of class-related adverse effects.
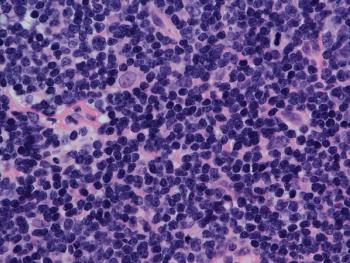
Lenalidomide plus rituximab consolidation therapy prior to bendamustine/rituximab induction did not significantly improve progression-free survival in patients with mantle cell lymphoma in the phase 2 NCTN E1411 trial.
The biologic license application for glofitamab for managing relapsed or refractory large B-cell lymphoma is supported by findings from the phase 1/2 NP30179 study.

Japanese patients with relapsed/refractory large B-cell lymphoma can now receive treatment with axicabtagene ciloleucel following its approval.
Treatment with the BTK inhibitor ibrutinib plus the CAR-T cell therapy tisagenlecleucel produced a high rate of durable responses in patients with relapsed/refractory mantle cell lymphoma after they stopped treatment at 6 months, according to early data from the TARMAC trial.
Bradford S. Hoppe, MD, MPH, and Omran Saifi, MD, offer a peer perspective on research by Gavin Jones, MD, and colleagues into radiation therapy in diffuse large B-cell lymphoma.
Acalabrutinib produced promising response rates in combination with lenalidomide and rituximab in previously untreated patients with mantle cell lymphoma.

Expert hematologist-oncologists discuess the E7438-G000-101 clinical trial and consider the EZH2 inhibitor tazemetostat as a treatment for relapsed/refractory follicular lymphoma.

The FDA’s decision to approve mosunetuzumab marks the first bispecific antibody approved to treat follicular lymphoma.
Gavin Jones, MD, and colleagues explore the landscape of radiation therapy in diffuse large B-cell lymphoma.
Referring responders with chemotherapy-sensitive relapsed/refractory diffuse large B-cell lymphoma who achieved a partial response or better to transplantation resulted in an improved overall survival vs those undergoing additional lines of therapy.

In a conversation during the 2022 American Society of Hematology Annual Meeting, an expert from the University of Texas MD Anderson Cancer Center, spoke to how treatments have improved for patients with mantle cell lymphoma.
Real-world data associate axicabtagene ciloleucel with temporarily worse quality of life in patients with diffuse large B cell lymphoma, transformed follicular lymphoma, or follicular lymphoma, which improves within 1-year post-infusion.
Treatment with induction and maintenance ibrutinib combined with chemoimmunotherapy and autologous stem cell transplant resulted in statistically significantly improved outcomes in a younger population with mantle cell lymphoma.
Lisocabtagene maraleucel was found to have superior efficacy in the second-line over standard of care therapy for patients with relapsed/refractory large B-cell lymphoma.
Patients with with primary central nervous system lymphoma experienced prolonged progression-free survival and a reduction in risk of death following treatment with high-dose chemotherapy and autologous stem cell transplant compared with non-myeloablative chemoimmunotherapy.
Mosunetuzumab produced durable responses with a tolerable toxicity profile in patients with relapsed/refractory follicular lymphoma, according to an updated analysis of the phase 2 GO29781 study.
The phase 2 ELARA trial indicated continued durable responses when patients with relapsed/refractory follicular lymphoma were treated with tisagenlecleucel.